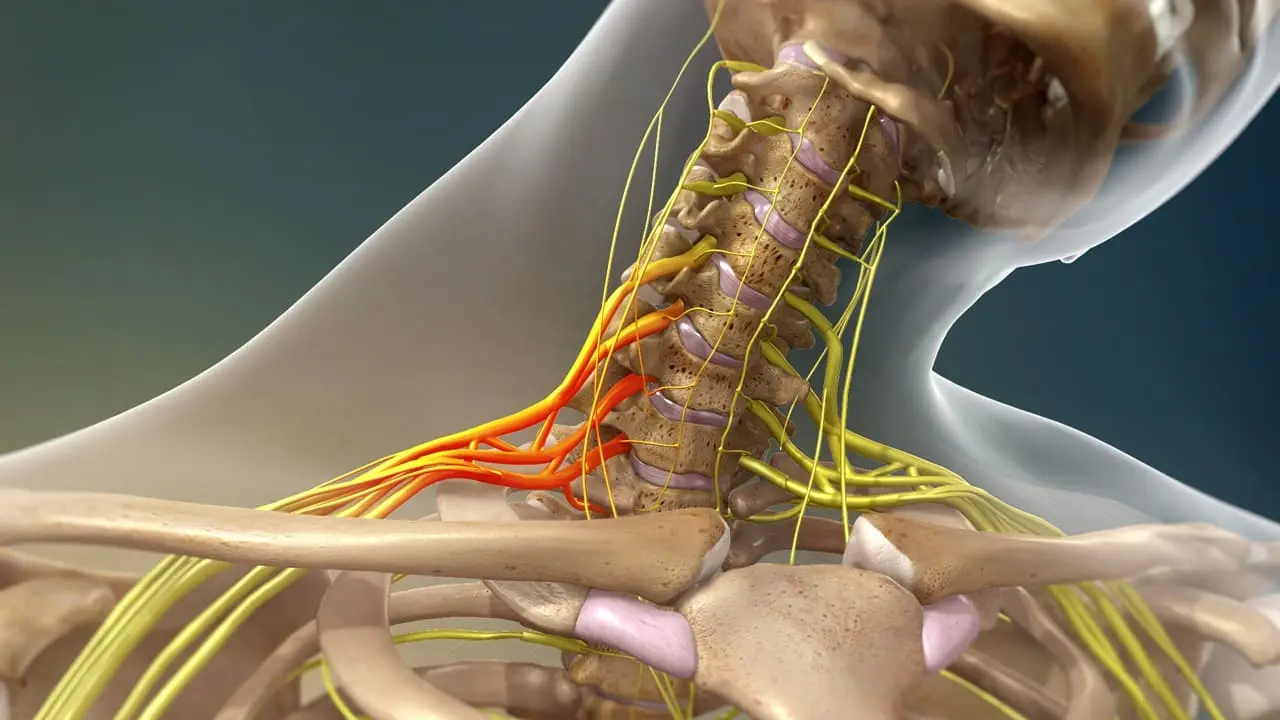
Overview
The cervical plexus is a network of nerves located deep in the neck, formed by the anterior rami of the first four cervical spinal nerves (C1–C4). These nerves play a vital role in providing sensory and motor innervation to parts of the neck, shoulders, and diaphragm. A cervical plexus injury refers to any damage, compression, or irritation to this nerve network, leading to pain, weakness, numbness, or functional loss in areas supplied by it.
Because the cervical plexus controls essential movements such as head rotation, neck flexion, and diaphragm function (via the phrenic nerve), even a mild cervical plexus injury can significantly impact a person’s daily life, breathing patterns, and posture.
At DMPhysios, a leading physiotherapy and rehabilitation center in Noida specializing in spine and sports conditions, our experts emphasize a patient-centered rehabilitation approach to restore nerve function, relieve pain, and rebuild confidence in movement after a cervical plexus injury.
Symptoms
The symptoms of a cervical plexus injury vary depending on which specific nerves are involved and the severity of the damage. Common symptoms include:
- Neck pain and stiffness: Usually radiating towards the shoulder or jaw.
- Numbness or tingling: Particularly in areas like the ear, neck, or upper chest.
- Muscle weakness: Difficulty turning the head or elevating the shoulder.
- Loss of sensation: Over the skin of the neck or parts of the scalp.
- Breathing difficulty: If the phrenic nerve (C3–C5) is affected.
- Voice changes or swallowing issues: If the injury extends deeper into the cervical region impacting motor control.
In severe cases, patients may also experience shoulder droop or partial paralysis of neck muscles. Early identification and targeted treatment are crucial for preventing long-term complications from a cervical plexus injury.
Types of Cervical Plexus Injury
While there are no rigidly defined “types,” cervical plexus injuries can be classified based on the nerve components or mechanism of damage:
- Upper Cervical Plexus Injury (C1–C2):
Leads to pain at the base of the skull, reduced head movement, and muscle tightness around the upper neck. - Middle Cervical Plexus Injury (C3–C4):
Causes sensory loss in the lateral neck and shoulder, and may affect motor control in neck flexion. - Lower Cervical Plexus Injury (C4–C5, overlapping with brachial plexus):
Results in shoulder weakness, tingling down the arm, and possibly diaphragmatic involvement. - Phrenic Nerve Injury:
As part of the cervical plexus, damage here affects the diaphragm, leading to breathing issues.
At DMPhysios, clinicians perform detailed nerve and muscle assessments to pinpoint the exact type and extent of cervical plexus injury, ensuring treatment is tailored to individual needs.
Causes
Several causes can contribute to a cervical plexus injury, ranging from direct trauma to postural or medical complications:
- Whiplash injuries: Sudden acceleration–deceleration accidents that overstretch neck nerves.
- Surgical complications: Especially after procedures involving the neck, thyroid, or cervical spine.
- Prolonged poor posture: Chronic strain on cervical muscles compresses neural structures.
- Nerve entrapment: Due to tight muscles (like the scalene or sternocleidomastoid) or soft tissue adhesions.
- Infections or inflammation: Such as meningitis or local infections causing nerve irritation.
- Cervical disc herniation or spondylosis: Compressing nerve roots contributing to the plexus.
- Birth trauma: In newborns, excessive neck traction during delivery can cause similar nerve injuries.
Understanding the root cause is the foundation of rehabilitation, which is why DMPhysios conducts detailed postural, neural, and orthopedic evaluations before initiating treatment.
Risk Factors
Certain factors increase the likelihood of developing a cervical plexus injury:
- Repeated sports trauma (e.g., wrestling, rugby, or martial arts).
- Previous neck surgeries or fractures.
- Poor ergonomic setup during desk work.
- Chronic cervical disc issues or arthritis.
- Diabetes or metabolic disorders causing neuropathy.
- Aging, which leads to degenerative changes and reduced tissue resilience.
Athletes and professionals who maintain sustained head-forward posture are particularly at risk, an aspect DMPhysios often addresses through preventive education and ergonomic correction sessions.
Treatment
The treatment for a cervical plexus injury depends on its cause and severity but generally includes:
- Medical Management:
- Anti-inflammatory medications and nerve pain relievers.
- Corticosteroid injections for inflammation control.
- Surgery (rare cases) to release trapped nerves or remove compressive lesions.
- Rest and Immobilization:
Initial rest may help acute inflammation subside. In certain cases, a soft cervical collar is used briefly. - Heat or Cold Therapy:
Reduces pain and muscle spasm, improving blood flow to the affected region.
However, long-term recovery from a cervical plexus injury is best achieved through comprehensive physiotherapy, which focuses on restoring function, strength, and posture.
Physiotherapy Treatment
At DMPhysios, physiotherapy for cervical plexus injury follows a highly structured, patient-centered approach focused on progressive recovery and long-term prevention. The rehabilitation protocol typically includes:
1. Pain and Inflammation Control
- Modalities used: Ultrasound therapy, TENS (Transcutaneous Electrical Nerve Stimulation), Accelerated Healing Therapy and gentle heat packs.
- Purpose: To desensitize the irritated nerve fibers and enhance local circulation.
2. Soft Tissue Mobilization
- Gentle myofascial release or trigger point therapy is used to reduce muscle tension in the sternocleidomastoid, scalene, and upper trapezius.
- These techniques relieve compression on the cervical plexus and improve mobility.
3. Postural Realignment
- Postural correction exercises target the deep cervical flexors and scapular stabilizers.
- Key exercises include:
- Chin tucks
- Scapular retraction and depression drills
- Thoracic extension on foam roller
- At DMPhysios, posture training is emphasized not only for recovery but also for long-term neck health.
4. Nerve Gliding Exercises
Specific neural mobilization techniques help maintain nerve flexibility and reduce adhesions.
For example, cervical lateral flexion with arm abduction can mobilize the nerve gently without overstretching.
5. Strengthening Phase
Once pain reduces, strengthening exercises are introduced for cervical and shoulder girdle muscles to protect the plexus.
Examples include:
- Isometric neck strengthening (against gentle resistance).
- Shoulder shrugs and resistance band exercises.
- Progressive resistance training for upper back muscles.
6. Breathing and Diaphragm Control (if Phrenic Nerve Involved)
- Breathing retraining exercises enhance respiratory control and coordination.
- Diaphragmatic breathing with manual facilitation is used when necessary.
7. Proprioceptive and Functional Training
- Balance and proprioception exercises improve neck stability and reduce recurrence risk.
- Activities like wall ball stabilization or laser-guided cervical retraining are common in advanced rehab stages at DMPhysios.
8. Ergonomic and Lifestyle Correction
- Patients are educated about workstation setup, sleeping posture, and safe lifting techniques.
- Therapists at DMPhysios customize ergonomic plans for working professionals to prevent repetitive stress on the cervical region.
Through these evidence-based interventions, DMPhysios ensures that recovery from a cervical plexus injury is not just about pain relief but also about restoring confidence, control, and long-term functionality.
Prevention
While not all cases can be prevented, adopting the following measures significantly reduces risk:
- Maintain proper posture while working or using digital devices.
- Strengthen neck and upper back muscles regularly.
- Warm-up adequately before sports activities.
- Avoid prolonged static positions by taking frequent breaks.
- Use ergonomic supports for chairs, monitors, and pillows.
- Treat cervical spine conditions early before they compress nerves.
At DMPhysios, prevention is as vital as treatment. Patients recovering from a cervical plexus injury are guided through ongoing exercise and education sessions to avoid recurrence and sustain neck health.
Conclusion
A cervical plexus injury can deeply affect daily life from simple neck movements to breathing and posture. Early diagnosis and a personalized rehabilitation plan make all the difference in recovery.
At DMPhysios, a reputed physiotherapy clinic in Noida specializing in spine and sports conditions, the focus is always on patient-centered rehabilitation. Their expert team combines manual therapy, exercise science, and advanced technology to address every component of a cervical plexus injury, ensuring patients return to their active lifestyles stronger and more aware of their body mechanics.
If you or someone you know is struggling with neck pain, weakness, or nerve-related discomfort, don’t wait for it to worsen. Visit DMPhysios in Noida today for a comprehensive assessment and personalized rehabilitation program that puts you at the center of recovery.