Overview
The hypoglossal nerve, also known as the twelfth cranial nerve (CN XII), plays a crucial role in controlling the movements of the tongue. It innervates all the intrinsic and most extrinsic muscles of the tongue, allowing for articulation, swallowing, and maintaining airway patency. When this nerve is compromised, the result is known as a hypoglossal nerve injury, a condition that can significantly impair speech, swallowing, and overall oral motor control.
Hypoglossal nerve injury may occur due to trauma, surgical complications, tumors, or neurological diseases. Although it is less common than other cranial nerve lesions, its functional consequences can be distressing and long-lasting. Early diagnosis and rehabilitation, especially physiotherapy interventions play a key role in improving function and quality of life.
At DMPhysios, a leading physiotherapy and rehabilitation clinic in Noida, patients suffering from hypoglossal nerve injury receive comprehensive, patient-centered care designed to restore muscle coordination, strength, and swallowing control through evidence-based rehabilitation programs.
Symptoms
The symptoms of hypoglossal nerve injury depend on the severity and whether the damage is unilateral (affecting one side) or bilateral (affecting both sides). Common symptoms include:
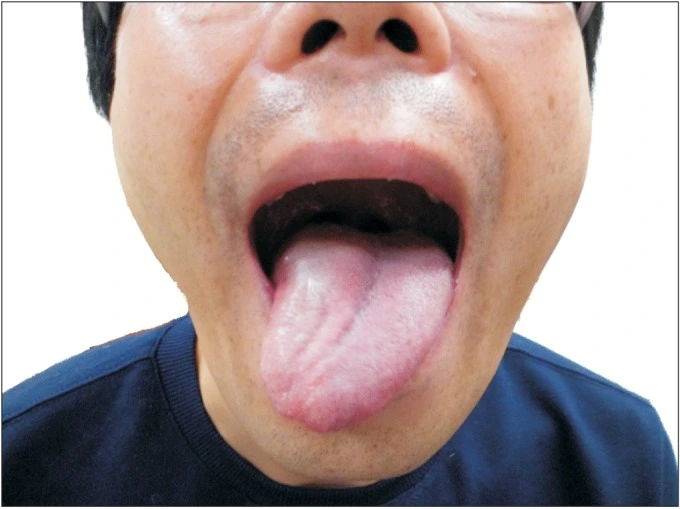
- Tongue Deviation: When the patient sticks out their tongue, it deviates toward the side of the lesion due to unopposed muscle action.
- Atrophy of the Tongue Muscles: Wasting and thinning of the tongue muscles on the affected side are common in chronic cases.
- Dysarthria: Difficulty in articulating words and speaking clearly due to poor tongue control.
- Dysphagia: Trouble swallowing food or liquids, which can increase the risk of aspiration.
- Fasciculations: Small involuntary twitching movements on the surface of the tongue.
- Reduced Tongue Strength: Difficulty in moving the tongue laterally or pushing food during chewing.
- Speech Fatigue: The patient may notice speech becoming slurred after prolonged talking.
In bilateral hypoglossal nerve injury, the patient may face severe swallowing and speech problems, inability to protrude the tongue, and even airway obstruction in extreme cases.
Types of Hypoglossal Nerve Injury
1. Unilateral Hypoglossal Nerve Injury:
This type affects only one side of the tongue. It is the most common presentation and usually occurs after trauma, surgery, or localized compression.
2. Bilateral Hypoglossal Nerve Injury:
This rare form affects both sides of the nerve and leads to complete paralysis of the tongue. It causes significant functional impairment and often requires extensive rehabilitation support.
3. Upper Motor Neuron vs Lower Motor Neuron Lesions:
- Upper Motor Neuron Lesions (e.g., due to stroke or brain injury) lead to contralateral weakness without muscle wasting.
- Lower Motor Neuron Lesions (e.g., due to peripheral nerve damage or tumor compression) cause ipsilateral paralysis with muscle atrophy and fasciculations.
At DMPhysios, identifying the exact type and level of hypoglossal nerve injury helps physiotherapists tailor individualized rehabilitation plans for maximum recovery outcomes.
Causes
The hypoglossal nerve has a long and complex course from the medulla oblongata to the tongue, making it susceptible to injury at multiple levels. Common causes include:
- Surgical Trauma:
- Head and neck surgeries (especially for tumors near the carotid artery or base of the skull).
- Cardiac or cervical spine surgeries where the nerve may be inadvertently stretched or compressed.
- Traumatic Injuries:
- Blunt head or neck trauma.
- Mandibular fractures or dislocations.
- Iatrogenic injuries during intubation.
- Tumors and Mass Lesions:
- Skull base tumors, paragangliomas, or metastases compressing the nerve pathway.
- Vascular Causes:
- Aneurysms or vascular malformations impinging on the nerve.
- Infectious or Inflammatory Conditions:
- Viral infections such as herpes zoster.
- Bacterial infections leading to nerve inflammation.
- Neurological Diseases:
- Multiple sclerosis or motor neuron disease can involve the hypoglossal nerve secondarily.
Risk Factors
Certain factors increase the likelihood of developing a hypoglossal nerve injury, including:
- Neck or skull base surgeries (especially carotid endarterectomy, cervical spine fixation).
- Prolonged intubation or use of airway devices.
- Head and neck trauma or radiation therapy.
- Systemic diseases like diabetes that affect nerve healing.
- Tumors in the posterior cranial fossa or parapharyngeal space.
- Stroke or other central neurological conditions.
Patients with these risk factors should be closely monitored post-procedure or post-trauma for any early signs of tongue dysfunction.
Treatment
The management of hypoglossal nerve injury depends on its underlying cause and severity. Treatment often involves a combination of medical, surgical, and rehabilitation approaches.
- Medical Management:
- Anti-inflammatory medications or corticosteroids for inflammatory causes.
- Antibiotics or antivirals if infections are identified.
- Vitamin B complex supplements to support nerve healing.
- Speech therapy and swallowing retraining to address functional difficulties.
- Surgical Management:
- Nerve decompression or repair in case of compressive lesions.
- Tumor excision if mass effect is present.
- Microsurgical nerve grafting may be considered in select traumatic cases.
While medical or surgical interventions address the root cause, physiotherapy plays a pivotal role in restoring muscle control, preventing atrophy, and retraining functional movements. This is where the expert team at DMPhysios, Noida excels in delivering personalized rehabilitation care.
Physiotherapy Treatment
Physiotherapy is an essential component of recovery for patients with hypoglossal nerve injury. The aim is to re-educate tongue movement, enhance muscle coordination, and improve swallowing and speech.
At DMPhysios, physiotherapists design a patient-centered rehabilitation plan tailored to the individual’s condition, recovery stage, and functional goals.
1. Initial Assessment and Education:
A detailed assessment of tongue movement, strength, speech articulation, and swallowing efficiency is performed. The patient is educated about the nature of their hypoglossal nerve injury, expected recovery timeline, and the importance of consistent rehabilitation.
2. Tongue Mobility Exercises:
These are designed to maintain and gradually improve tongue movement. Examples include:
- Tongue Protrusion: Sticking out the tongue and holding it for 5–10 seconds.
- Lateral Tongue Movement: Moving the tongue side to side.
- Tongue Elevation: Touching the tongue tip to the roof of the mouth.
- Resistance Training: Pressing the tongue against a tongue depressor or finger to build strength.
3. Speech Therapy Integration:
Close coordination between physiotherapists and speech-language pathologists ensures comprehensive management. Articulation and phonation exercises are practiced to enhance clarity and control.
4. Swallowing Retraining:
For patients with dysphagia, retraining exercises focus on tongue-palate coordination, laryngeal elevation, and safe swallowing mechanics. Techniques such as the Mendelsohn maneuver and effortful swallow are incorporated under supervision.
5. Neuromuscular Re-education Techniques:
- Facial and lingual proprioceptive neuromuscular facilitation (PNF) patterns are applied to activate weak muscles.
- Biofeedback training helps patients visualize tongue movement patterns and make corrections in real time.
6. Electrical Stimulation (if indicated):
Surface neuromuscular electrical stimulation (NMES) can be applied under professional supervision to stimulate inactive tongue muscles and promote recovery.
7. Postural and Breathing Training:
Correct neck posture and diaphragmatic breathing help maintain airway control and swallowing efficiency, which are often affected in hypoglossal nerve injury cases.
8. Home Exercise Program:
Patients at DMPhysios receive a custom home exercise plan with specific tongue and jaw exercises to practice daily. This reinforces clinic-based sessions and accelerates recovery.
Prevention
While not all cases are preventable, certain measures can minimize the risk:
- Careful Surgical Planning: Surgeons must take precautions to avoid nerve traction or compression during head and neck operations.
- Proper Airway Management: Gentle intubation techniques and appropriate tube sizing reduce risk during anesthesia.
- Postural Awareness: Avoid prolonged hyperextension of the neck, especially after surgery.
- Early Physiotherapy Intervention: Initiating rehabilitation soon after diagnosis prevents muscle atrophy and functional decline.
- Control of Systemic Conditions: Managing diabetes, hypertension, and vascular health lowers the risk of secondary nerve involvement.
At DMPhysios, preventive physiotherapy counseling is often provided to post-operative and post-trauma patients to safeguard against secondary complications and promote optimal recovery.
Conclusion
A hypoglossal nerve injury can profoundly impact essential daily activities like speaking, swallowing, and even breathing in severe cases. However, with early detection, comprehensive treatment, and focused rehabilitation, significant recovery is achievable.
DMPhysios, a reputed physiotherapy and rehabilitation center in Noida specializing in spine and sports conditions, offers patient-centered rehabilitation programs tailored to the unique needs of each individual suffering from hypoglossal nerve injury. Their expert team combines advanced manual therapy, neuromuscular re-education, and functional training techniques to restore movement, rebuild strength, and regain confidence.
If you or someone you know is experiencing symptoms of hypoglossal nerve injury, don’t delay the recovery process. Visit DMPhysios Noida today for a detailed assessment and a personalized rehabilitation plan designed to help you regain control, improve function, and live without limitations.