Overview
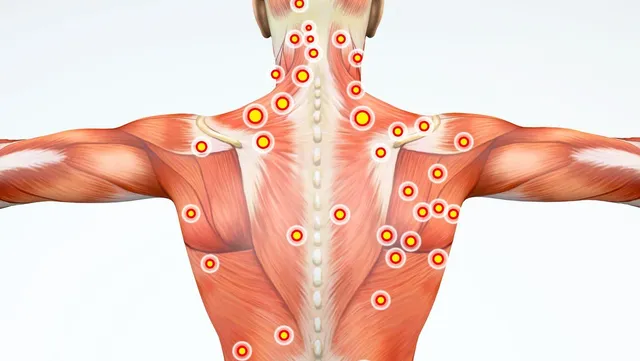
Myofascial Pain Syndrome is a long-term musculoskeletal condition that primarily affects the soft tissues of the body. It is characterized by persistent pain, stiffness, and tenderness in specific muscle groups, usually caused by the development of what are known as trigger points. These trigger points are small, hyperirritable nodules that form within tight bands of muscle fibers. When pressed, they not only produce localized pain but also refer pain to distant regions of the body, often mimicking other disorders. For example, a trigger point in the shoulder may radiate discomfort down the arm, or a trigger point in the neck may cause headaches.
Unlike ordinary post-exercise soreness or temporary muscle fatigue, Myofascial Pain Syndrome does not resolve on its own after a period of rest. Instead, the pain tends to linger, interfere with normal movement patterns, and limit overall functionality. Over time, if left untreated, the condition can affect posture, reduce flexibility, and compromise daily activities such as working, exercising, or even sleeping comfortably.
One of the challenges with Myofascial Pain Syndrome is that it often goes underdiagnosed. The symptoms are frequently mistaken for other musculoskeletal or nerve-related problems such as arthritis, cervical spondylosis, or neuropathies. This misidentification can delay treatment, allowing the condition to progress further and lead to chronic discomfort. Early recognition, accurate diagnosis, and structured management are therefore essential to prevent long-term complications.
At DMPhysios, a well-known clinic in Noida that specializes in spine and sports-related conditions, the emphasis is placed on patient-centered rehabilitation. Their approach to Myofascial Pain Syndrome goes beyond simply alleviating pain — it focuses on addressing the root causes of muscle tension, correcting postural imbalances, and teaching patients effective strategies for long-term relief. With personalized physiotherapy plans, advanced manual therapy techniques, and corrective exercise programs, DMPhysios helps individuals not only recover from Myofascial Pain Syndrome but also regain confidence in their movement and return to a pain-free, active lifestyle.
Symptoms
The symptoms of Myofascial Pain Syndrome vary depending on the affected muscles, but common clinical signs include:
- Localized Muscle Pain – Deep, aching, or throbbing pain in a specific muscle or group of muscles.
- Trigger Points – Palpable knots or nodules within tight muscle bands that are tender to touch.
- Referred Pain – Pain that radiates from the trigger point to other areas (e.g., a trigger point in the shoulder may cause pain down the arm).
- Restricted Range of Motion – Stiffness or difficulty moving joints freely due to muscle tightness.
- Muscle Weakness – Muscles may feel fatigued or weak, especially with repeated use.
- Sleep Disturbances – Pain and stiffness often worsen at night, affecting rest and recovery.
- Tingling or Burning Sensations – Some individuals report neurological-like symptoms due to prolonged muscle tension.
When left untreated, Myofascial Pain Syndrome can contribute to secondary issues like poor posture, chronic fatigue, and reduced physical performance.
Types of Myofascial Pain Syndrome
While Myofascial Pain Syndrome is often classified under a broad category, it can be divided into two primary types based on the behavior of trigger points:
- Active Trigger Point Myofascial Pain Syndrome
- Pain is constant or reproduced even at rest.
- Trigger points are tender and cause referred pain patterns.
- Associated with significant movement restriction and discomfort.
- Latent Trigger Point Myofascial Pain Syndrome
- Pain is not constant but occurs when the trigger point is pressed or stimulated.
- Common in individuals with poor posture, repetitive strain, or sedentary lifestyle.
- Can progress into active trigger points if left unaddressed.
Understanding these types helps clinicians at DMPhysios tailor rehabilitation programs that address both immediate pain relief and long-term prevention.
Causes
The exact cause of Myofascial Pain Syndrome is often multifactorial, but several contributing factors are well-recognized:
- Muscle Overuse – Repetitive movements, sports training, or occupational strain.
- Muscle Injury or Trauma – Accidents, falls, or sudden impacts leading to muscle fiber damage.
- Poor Posture – Prolonged slouching, forward head posture, or incorrect sitting positions.
- Stress and Anxiety – Emotional tension can lead to muscle tightening, forming trigger points.
- Lack of Physical Activity – Sedentary lifestyle reduces circulation and promotes stiffness.
- Nutritional Deficiencies – Lack of vitamins (B-complex, Vitamin D, magnesium) may impair muscle health.
- Underlying Conditions – Disorders like fibromyalgia, arthritis, or chronic fatigue syndrome can worsen myofascial pain.
Risk Factors
Certain individuals are more prone to developing Myofascial Pain Syndrome. The risk factors include:
- Age – Most common in adults aged 30–60.
- Occupational Hazards – Desk jobs, repetitive manual labor, or athletes with repetitive training.
- Chronic Stress – High stress levels contribute to sustained muscle tension.
- Poor Ergonomics – Inadequate workstation setup or prolonged device use.
- Sleep Disturbances – Lack of restorative sleep impairs muscle recovery.
- Previous Injuries – Scar tissue and muscle imbalances predispose to trigger points.
At DMPhysios, risk factor management is integrated into patient education, ensuring long-term recovery and prevention of relapses.
Treatment
The treatment of Myofascial Pain Syndrome requires a multi-dimensional approach to relieve pain, release muscle tightness, and restore functional movement. Treatment options include:
- Medications
- Non-steroidal anti-inflammatory drugs (NSAIDs) for pain relief.
- Muscle relaxants for reducing spasms.
- Antidepressants in chronic cases with associated mood disorders.
- Trigger Point Injections
- Local anesthetic or corticosteroid injections to deactivate trigger points.
- Dry Needling
- Insertion of thin needles into trigger points to release muscle tension.
- Massage Therapy
- Manual techniques to improve circulation, relax muscles, and release knots.
- Heat and Cold Therapy
- Heat increases blood flow and eases stiffness.
- Cold reduces inflammation and acute pain.
- Lifestyle Modifications
- Correcting posture, improving ergonomics, and maintaining regular physical activity.
While these methods help, physiotherapy remains the cornerstone of treatment for Myofascial Pain Syndrome, as it not only addresses pain but also corrects underlying dysfunctions.
Physiotherapy Treatment
At DMPhysios, physiotherapy is at the heart of patient-centered rehabilitation for Myofascial Pain Syndrome. A detailed, customized approach ensures long-term results. Physiotherapy management includes:
1. Manual Therapy
- Myofascial release techniques to reduce stiffness.
- Trigger point pressure release to deactivate pain points.
- Soft tissue mobilization to restore muscle elasticity.
2. Stretching Exercises
- Passive and active stretching to elongate tight muscles.
- Post-isometric relaxation techniques.
- Focus on commonly affected areas such as neck, shoulders, and lower back.
3. Strengthening Exercises
- Corrects muscular imbalances.
- Builds endurance in stabilizing muscles.
- Progressive resistance training tailored to the patient’s needs.
4. Posture Correction
- Ergonomic education for work and daily activities.
- Core strengthening and spinal alignment programs.
- Breathing and relaxation exercises to reduce tension.
5. Electrotherapy Modalities
- Ultrasound therapy for deep tissue healing.
- TENS (Transcutaneous Electrical Nerve Stimulation) for pain control.
- Interferential therapy to reduce muscle spasms.
6. Dry Needling & Cupping Therapy
- Effective adjunct therapies used at DMPhysios to deactivate stubborn trigger points and improve blood flow.
7. Patient Education
- Teaching self-management techniques like foam rolling, relaxation exercises, and home-based stretches.
- Preventive strategies to avoid recurrence.
Through this evidence-based approach, DMPhysios ensures patients not only recover from Myofascial Pain Syndrome but also gain the tools to prevent its return.
Prevention
Preventing Myofascial Pain Syndrome is possible with lifestyle modifications and proactive muscle care. Recommended strategies include:
- Maintain good posture during daily activities and work.
- Incorporate stretching breaks during long hours of sitting.
- Engage in regular physical activity, including strengthening and mobility exercises.
- Manage stress with techniques like yoga, meditation, and breathing exercises.
- Ensure proper ergonomics at workstations.
- Use correct form and avoid overtraining during sports or workouts.
- Stay hydrated and maintain a balanced diet rich in muscle-supporting nutrients.
- Prioritize quality sleep for optimal muscle recovery.
Conclusion
Myofascial Pain Syndrome is a chronic but highly manageable condition when addressed with the right treatment strategies. Early diagnosis, physiotherapy, and lifestyle modifications are key to preventing long-term disability and ensuring a pain-free, active life.
At DMPhysios, a Noida-based clinic specializing in spine and sports conditions, patients receive patient-centered rehabilitation that goes beyond short-term relief. By integrating manual therapy, advanced physiotherapy techniques, and education, DMPhysios ensures comprehensive care for individuals struggling with Myofascial Pain Syndrome.If you or someone you know is experiencing persistent muscle pain, stiffness, or trigger points, don’t wait for it to worsen. Book a consultation with DMPhysios today and take the first step toward lasting recovery and pain-free movement.