Overview
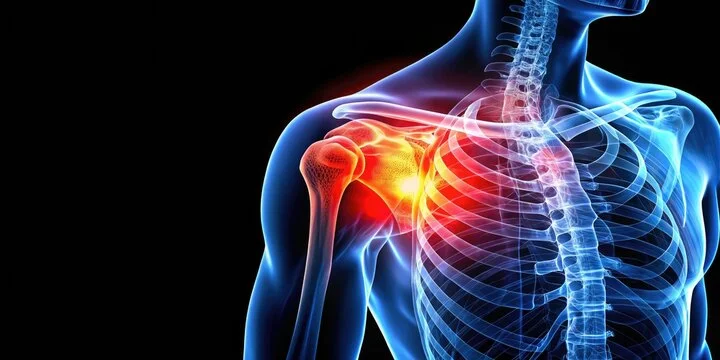
The human shoulder is a marvel of anatomy — highly mobile, versatile, and responsible for a wide range of upper limb functions. But this mobility comes at a cost. It is inherently unstable due to its shallow socket, making it vulnerable to one of the most common joint injuries: shoulder dislocation.
A shoulder dislocation happens when the head of the upper arm bone (humerus) slips out of the glenoid socket of the shoulder blade. This is not just a temporary inconvenience — it’s a serious orthopedic injury that can lead to chronic instability, muscle weakness, joint damage, and long-term disability if not treated properly.
At DMPhysios, a leading physiotherapy clinic located in Noida and specializing in spine and sports-related conditions, we often treat individuals dealing with shoulder dislocations — from athletes to elderly patients, from traumatic injuries to recurrent instability cases. Our focus is on thorough assessment, accurate diagnosis, and structured, patient-centered rehabilitation for long-lasting results.
Symptoms of Shoulder Dislocation
Recognizing a shoulder dislocation is usually straightforward, especially when the injury is acute. However, symptoms can sometimes be misinterpreted, especially in partial dislocations or recurrent cases.
The hallmark symptoms include:
- Sudden, intense pain in the shoulder region after injury or trauma.
- Apparent deformity — the shoulder may look flattened or “squared off” due to the displaced humeral head.
- Restricted movement — patients are typically unable to lift or rotate the arm.
- Swelling and bruising, especially if blood vessels or surrounding tissues are affected.
- Tingling or numbness radiating down the arm, indicating potential nerve compression or traction.
- Muscle spasms, which may further lock the joint in the wrong position.
- Fear of movement, as attempting to use the arm worsens the pain.
Prompt diagnosis and realignment are critical. Left untreated, a shoulder dislocation can result in chronic joint looseness, cartilage damage, and frequent recurrence.
Types of Shoulder Dislocation
Shoulder dislocations are broadly classified based on the direction in which the humeral head exits the glenoid cavity. Understanding the specific type is crucial for deciding the correct line of treatment.
1. Anterior Dislocation
This is the most common type, accounting for approximately 90-95% of all shoulder dislocations. It usually results from a forceful blow to the shoulder or a fall on an outstretched arm, forcing the humeral head forward.
2. Posterior Dislocation
Far less common, this occurs when the humeral head is displaced backward. Posterior dislocations are often seen in patients who’ve had seizures or electric shocks, which cause violent muscle contractions.
3. Inferior Dislocation (Luxatio Erecta)
A rare form of shoulder dislocation where the arm is locked in a raised position. It commonly results from a hyperabduction injury—like falling with the arm stretched overhead—which drives the humeral head downward and out of the shoulder joint.
Each type can have different associated injuries — such as labral tears, capsular damage, or rotator cuff injuries — which must be thoroughly evaluated during the rehabilitation process at DMPhysios.
Causes
A shoulder dislocation can occur due to many reasons, and it is not restricted to professional athletes. The underlying mechanisms often include:
- Trauma or Impact: A direct hit during contact sports, a fall on an outstretched hand, or accidents are the most frequent culprits.
- Repetitive Overhead Motion: Common in swimmers, volleyball players, cricketers, and tennis players. Constant stress can loosen ligaments and eventually cause dislocation.
- Lax Ligaments or Hypermobile Joints: Individuals with generalized ligamentous laxity or genetic connective tissue disorders are more prone to shoulder dislocations.
- Previous Dislocations: Once the joint has been dislocated, the surrounding structures are more likely to stretch or tear, increasing the risk of recurrence.
- Improper Training or Technique: Poor weightlifting form or overtraining can cause excessive strain on the shoulder.
At DMPhysios, our expert team evaluates not only the traumatic history but also postural alignment, muscle balance, and training techniques to identify and treat the root cause effectively.
Risk Factors
There are specific risk factors that increase the likelihood of experiencing a shoulder dislocation. These include:
- Age and Gender: Young males, particularly those aged between 18–30, are at highest risk due to high levels of sports and physical activity.
- Participation in Contact or Overhead Sports: Football, rugby, basketball, swimming, and throwing sports significantly increase shoulder strain.
- History of Previous Dislocations: Once dislocated, the shoulder joint becomes less stable, increasing the likelihood of future injuries.
- Poor Muscle Strength or Imbalance: Weak rotator cuff and scapular muscles fail to provide dynamic joint stability.
- Improper Rehabilitation: Inadequate rehab following a first dislocation can result in recurrent instability and chronic shoulder dysfunction.
DMPhysios focuses not only on treatment but also on long-term risk reduction through education, conditioning, and preventive physiotherapy.
Treatment Options
The treatment approach for a shoulder dislocation depends on several factors — whether it’s a first-time or recurrent injury, the age and activity level of the patient, and the extent of soft tissue damage.
1. Reduction
In the acute phase, the priority is to reposition the humeral head back into the socket. This procedure, known as closed reduction, should only be performed by trained medical personnel to avoid further injury.
2. Immobilization
Following reduction, the arm is typically placed in a sling or immobilizer for a few weeks. This helps the surrounding ligaments and soft tissues to heal.
3. Pain and Inflammation Control
Anti-inflammatory medications, cold packs, and rest are recommended during the initial healing phase. At DMPhysios, modalities such as ultrasound therapy or TENS may also be used to reduce pain.
4. Surgery (in Selected Cases)
Surgical repair may be indicated if:
- There are repeated dislocations (chronic instability)
- The labrum or ligaments are severely torn
- A bony fragment is fractured or the joint has lost congruity
Arthroscopic procedures are commonly used to stabilize the joint while minimizing tissue trauma. Post-surgical rehab is essential for full recovery.
Physiotherapy Treatment (Detailed Protocol at DMPhysios)
Rehabilitation is the cornerstone of shoulder dislocation treatment — not only to restore function but to prevent re-injury. At DMPhysios, our patient-centered physiotherapy protocol addresses each phase of healing with individualized care plans.
Phase 1: Acute/Immobilization Phase (Week 0–2)
Goals:
- Pain reduction
- Inflammation control
- Maintain mobility in surrounding joints
Approach:
- Cryotherapy, TENS, and gentle manual therapy
- Passive mobilization of elbow, wrist, and neck
- Sling support and posture education
Phase 2: Early Mobilization (Week 2–6)
Goals:
- Restore pain-free range of motion (ROM)
- Begin muscle activation
Approach:
- Pendulum exercises
- Active-assisted ROM exercises (flexion, abduction)
- Isometric strengthening of deltoids and rotator cuff
- Scapular stabilization drills
Phase 3: Strengthening and Proprioception (Week 6–12)
Goals:
- Restore strength and dynamic stability
- Improve neuromuscular control
Approach:
- Resistance band exercises (internal/external rotation)
- Closed-chain drills (wall push-ups, ball presses)
- Balance and proprioceptive tasks (wobble board, gym ball)
- Functional lifting patterns and posture correction
Phase 4: Return to Activity (Week 12+)
Goals:
- Full return to sports, work, and daily life
- Prevent re-dislocation
Approach:
- Sport-specific training (throwing, swimming strokes)
- Plyometric and agility drills
- Core and kinetic chain integration
- Shoulder loading tests and return-to-play clearance
Throughout all phases, DMPhysios ensures continuous monitoring and patient feedback, adjusting intensity and exercise progression accordingly. Our focus on manual therapy, individualized exercise plans, and long-term conditioning makes us a trusted rehab destination in Noida.
Prevention
Preventing shoulder dislocation, especially in high-risk individuals, is not only achievable but essential for long-term joint health. Key strategies include:
- Regular strengthening of rotator cuff and scapular muscles
- Proper technique during lifting and athletic activity
- Adequate warm-up and cool-down routines
- Flexibility training, especially for tight pectorals and posterior capsule
- Posture correction, particularly for forward-rounded shoulders
- Rehabilitation compliance after any shoulder injury
DMPhysios also offers preventive care programs — including sports screenings, shoulder stability workshops, and customized home exercise plans — all tailored to help individuals avoid injury recurrence.
Conclusion
A shoulder dislocation is more than just a painful accident — it’s a serious orthopedic event that requires expert diagnosis, careful treatment, and structured rehabilitation. Whether you’re an athlete, an office-goer, or someone recovering from an accident, your recovery journey must be guided by professionals who understand both the injury and the individual behind it.
At DMPhysios, we combine the latest evidence-based techniques with a personal, compassionate touch. Located in Noida and recognized for our excellence in treating spine and sports conditions, our clinic offers a full spectrum of services — from pain management to complete rehabilitation and long-term injury prevention.If you or someone you know is dealing with a shoulder dislocation, don’t delay. Early intervention can make all the difference. Book an appointment with DMPhysios today and take your first step toward strength, stability, and a healthier shoulder.