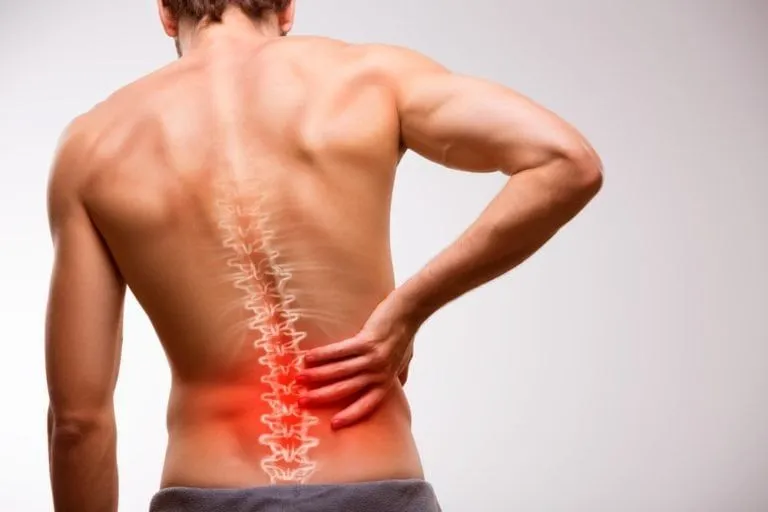
Low back pain (LBP) is one of the most common musculoskeletal complaints in athletes and non‑athletes alike.


Low back pain (LBP) is one of the most common musculoskeletal complaints in athletes and non‑athletes alike. In athletes, chronic low back pain not only impairs performance but often becomes a persistent, frustrating “stiffness‑pain” cycle that resists simple explanations. Among the many anatomical and neuromuscular contributors, one structure that is increasingly gaining attention is the deep lumbar multifidus muscle.
In recent years, researchers using imaging techniques such as shear‑wave elastography have demonstrated that athletes with chronic low back pain often show increased stiffness of the deep multifidus — more so than the superficial portions. This altered stiffness appears to contribute to dysfunction, pain maintenance, and poor recovery if not properly addressed.
What Is Deep Multifidus, and Why Is It Important?
Anatomy and function of the multifidus
The multifidus is a series of small muscles located adjacent to the vertebral column, spanning multiple vertebral levels. In the lumbar spine region, it is a critical part of the paraspinal musculature.
Importantly, the multifidus has layers:
- Deep fibers (segmental multifidus): These attach more locally — from one vertebra to the adjacent one. They act as segmental stabilizers , controlling micro‑movements between vertebrae, resisting shear, and enhancing proprioception.
- Superficial fibers: These span multiple segments and contribute more to gross trunk extension, assistance in load bearing, and postural support.
The deep portion is thus often considered part of the spine’s “fine control” or “local stabilizer” system, complementing global muscles such as erector spinae, obliques, quadratus lumborum, etc.
Because the deep multifidus is intimately involved in controlling small intersegmental motion, its proper function is critical to maintain spinal integrity, reduce microtrauma, and manage load transfer across vertebral joints.
Why the deep multifidus matters in athletes
For athletes, the lumbar spine is under frequent demands: repeated trunk extension, rotation, load carrying, abrupt deceleration, twisting, and more. Even small aberrant intersegmental movements (or micro-instability) can gradually accumulate stress. The deep multifidus helps damp these perturbations:
- It helps resist small shear and torsional forces between adjacent vertebrae
- It contributes to proprioceptive feedback and neuromuscular reflex control
- It acts as a first responder to sudden perturbations, stiffening to maintain alignment
- Its proper coordination ensures that larger trunk muscles don’t overcompensate or overload passive structures
Thus, when the deep multifidus becomes dysfunctional — e.g., with increased stiffness, delayed activation, atrophy, or fatty infiltration — the balance of spinal control is disrupted. Over time, this may predispose to pain, irritation of joints or discs, and maladaptive movement patterns.
What Does “Increased Stiffness” Mean?
Stiffness, in a biomechanical / physiological sense, refers to resistance to stretch or deformation under load. In muscles, stiffness is a composite of passive (resting) properties and active tension (tone, co-contraction).
When we talk about increased stiffness in the deep multifidus, especially in the context of low back pain, we usually refer to:
- Passive stiffness: The tissue’s non-contractile resistance (e.g., connective tissue, fibrosis, extracellular matrix changes, collagen cross‑linking) when stretched or manipulated.
- Active/neuromuscular stiffness: Elevated baseline muscle tone, increased resting motor unit firing, or neural facilitation that causes the muscle to resist lengthening even before voluntary contraction.
Imaging studies using shear wave elastography quantify stiffness in terms of Young’s modulus or kilopascals (kPa), indicating how much force is needed to deform the tissue.
Importantly, “increased stiffness” is not always beneficial. While a certain degree of stiffness aids stability, excessive stiffness impairs adaptability: the muscle cannot relax or lengthen efficiently, reducing its capacity to respond dynamically to changing loads or sudden perturbations.
In the deep multifidus, excessive stiffness may reflect:
- Chronic guarding or protective contraction
- Structural changes (fibrosis, collagen deposition, micro‑scarring)
- Neuromuscular maladaptation (overactivity, altered reflexes)
- Reduced elasticity or compliance
Thus, when stiffness becomes pathological, it reduces functional capacity, flexibility, and effective control.
Why Does Deep Multifidus Stiffness Develop in Athletes with Back Pain?
Understanding why stiffness occurs is essential to design effective rehabilitation. The development is multifactorial, involving biomechanical, neural, structural, and behavioral contributors. Below are key pathways:
- Pain‑induced muscle guarding (protective reflex)
When the lumbar spine is subjected to pain or irritation (e.g., disc, facet, soft-tissue), the nervous system often induces increased muscle tone in adjacent stabilizers, including multifidus, to “protect” the region. This guarding initially serves a protective role but, if sustained, leads to chronic overactivity.
Over time, this elevated resting tone causes micro‑damage, connective tissue changes, and reduced capacity to relax — culminating in stiffness.
- Altered motor control and timing
Chronic low back pain is associated with altered neuromuscular control: timing of muscle activation changes, recruitment patterns shift, and inhibitory pathways get disrupted. This can cause the deep multifidus to stay in a semi‑contracted state even when not needed, rather than toggling between relaxed and active states.
Because the deep fibers are supposed to engage only in precise, low-level recruitment, their overuse or persistent activation is maladaptive.
Additionally, some studies indicate that motor control (e.g. isometric multifidus activation) can influence cortical changes (M1 motor area excitability) and thus perpetuate altered neurocontrol.
- Repetitive microtrauma and cumulative load
Athletes often expose the lumbar spine to repeated stresses — extension, rotation, load transfers, twisting, sudden deceleration, and asymmetric forces. Over time, microtrauma may occur in soft tissues (ligament, facet joints, paraspinal musculature).
As a response, localized fibrosis or micro‑scarring may develop, stiffening the muscle to “stabilize” the region. This is akin to how overused muscle groups elsewhere develop increased tone or tightness.
- Disuse, inhibition, and compensatory adaptation
Pain often leads to certain movements being “avoided.” If the athlete suppresses trunk movement or spinal micro-motions, the multifidus may gradually lose its dynamic range and adaptability. The deep fibers might also undergo fatty infiltration or atrophy over longer periods (as seen in chronic LBP imaging studies).
Subsequently, the system may “lock in” a stiffer behavior as compensation: global muscles and ligaments may take over, which further reduces dynamic capacity of the deep multifidus.
- Training imbalance, technique errors, and biomechanical overload
Athletes often have strengths and movement patterns that bias certain muscle groups. For instance:
- Overemphasis on trunk extension or hyperextension
- Imbalanced core training (e.g. superficial muscles dominate over local stabilizers)
- Poor lifting or load transfer technique
- Asymmetries or imbalances in hip, pelvis, or lower limb mechanics
These can overload the lumbar region and chronically strain multifidus, pushing it to adopt a stiffer state to resist perturbations.
Consequences of Deep Multifidus Stiffness
Once stiffness is entrenched, a cascade of adverse effects can follow — compounding pain, dysfunction, and risk of re-injury. Key consequences include:
- Reduced segmental mobility and adaptability
Stiffness limits the ability of spinal segments to adjust and flex/extend or rotate subtly. In sports and daily tasks, the spine must adapt to small perturbations; stiff regions cannot respond fluidly, increasing risk of injury elsewhere.
- Altered load transmission and overload of passive structures
If the active stabilizing system (multifidus + deep core synergy) fails to buffer forces, more load is transferred to passive structures—e.g.:
- Intervertebral discs
- Facet joints
- Ligaments
- Joint capsules
Over time, this contributes to degeneration, pain sensitization, and further dysfunction.
- Persistent pain‑stiffness cycle
Stiffness itself can provoke nociceptive inputs (through increased tissue stress, microtrauma, ischemia). That pain perpetuates muscular guarding, which increases stiffness further—a vicious cycle.
Athletes may feel a sensation of “tightness” or “locking” even in absence of acute injury.
- Compensatory movement patterns & secondary injuries
To avoid loading the stiff lumbar spine, the athlete may recruit compensatory motion from neighboring segments (thoracic, hip, pelvis). Over time, these compensations increase the risk of:
- Hip or sacroiliac overuse
- Lumbar-thoracic junction stress
- Asymmetry or overuse in contralateral muscles
- Core fatigue and global instability
- Impaired athletic performance & tolerance
Stiffness limits maximal range, reaction capacity, and adaptability. Athletes may lose speed, agility, or tolerate less aerobic/trunk-endurance load. Training interruptions, suboptimal mechanics, and re-injury risk increase.
Physiotherapy Role: Assessment, Treatment & Prevention
Addressing deep multifidus stiffness requires a multimodal, staged, and targeted physiotherapy approach . Here is a structured framework:
1. Clinical assessment & diagnosis
A thorough assessment is the foundation. Key components include:
a. History & symptom profiling
- Duration, pattern, aggravating / relieving factors
- Sport-specific demands, training load history
- Previous injuries, compensations, asymmetries
- Behavior of stiffness (morning vs evening, after rest, with movement).
b. Palpation, manual testing & muscle tone evaluation
- Tenderness, hypertonicity, stiffness on palpation in paraspinal region
- Assessment of segmental mobility (mobility tests, segmental joint play)
- Observation of movement control (e.g. stoop-squat, lumbar flexion/extension, flexion-relaxation phenomenon)
c. Motor control and activation testing
- Assess whether deep multifidus can be selectively activated (e.g. with “abdominal draw-in” techniques, feedback methods)
- Use static and dynamic tests: e.g. quadruped leg raise, bird-dog, prone extension with minimal activation
- Evaluate timing, recruitment patterns, co-contraction with transversus abdominis, pelvic floor, obliques
d. Imaging & elastography (if available)
- Shear wave elastography (SWE) can quantify stiffness (Young’s modulus) of deep vs superficial multifidus. In athletes with chronic LBP, DLM stiffness is elevated vs controls.
- Ultrasound or MRI may reveal atrophy, fatty infiltration, asymmetry, thickness differences.
- Correlate stiffness findings with clinical pain and functional deficits.
e. Functional and sport‑specific testing
- Movement analysis (lifting, bending, twisting, change-of-direction)
- Assess core endurance, trunk flexion/extension ROM, neuromuscular fatigue
- Pelvis, hip, and lower limb biomechanics (to detect compensatory influences)
From this assessment, you should be able to localize the stiff segments, identify control deficits, and design a staged rehabilitation program.
2. Phase 1: Pain relief, relaxation & reducing guarding
Before attempting to “retrain” a stiff muscle, you often need to reduce pain, guarding, and excessive tone.
a. Manual therapy & soft tissue techniques
- Myofascial release, trigger point release on lumbar paraspinals
- Passive segmental mobilizations (gentle, pain-free)
- Muscle energy techniques to address adjacent joint restrictions
b. Modalities & adjunctive interventions
- Thermal therapy (heat) to enhance tissue extensibility
- Electrotherapy (TENS, IFC) for pain modulation
- Dry needling or instrument-assisted soft tissue mobilization (if trained)
- Ultrasound or shock wave (as adjuncts)
- Neural mobilization (if neural irritability is present)
c. Patient education & posture/behavior strategies
- Teach patients to avoid excessive static postures or sustained flexion/extension
- Encourage micro-movements, frequent positional shifts
- Educate about load management (reducing volume/intensity temporarily)
- Breathing awareness to reduce accessory muscle overactivity
The aim is to reduce hypertonus, allow tissues to soften, and reduce input from nociceptive systems so that retraining becomes effective.
3. Phase 2: Deep multifidus activation & motor re‑education
Once pain and guarding have eased, the next objective is to re-establish selective control and activation of the deep multifidus — without overloading compensatory muscles.
a. drills (isolation first)
- Prone abdominal draw-in with minimal movement
- “Segmental lift” techniques: gently gliding or lifting the vertebra without gross motion
- Use tactile cues and palpation to feel contraction
- Begin in stable positions (prone, quadruped, supine)
b. Feedback-enhanced training
- Real-time ultrasound (rehabilitative ultrasound imaging, RUSI) to visualize multifidus contraction
- Biofeedback or pressure biofeedback (e.g. pressure cuff under abdomen)
- EMG-based feedback (if available)
c. Gradual progression to more challenging positions
- Quadruped leg-raises (bird-dog variation), adding limb movement while maintaining multifidus engagement
- Dead bug, side-bridge, glute-bridges with control
- Integration with transverse abdominis, pelvic floor, obliques
d. Co-contraction and timing emphasis
- Train anticipatory activation: e.g. multifidus pre-activation before limb movement
- Incorporate perturbations (small external disturbances) to force reflexive multifidus recruitment
- Emphasize low-load, high-control tasks initially
This phase may last weeks to months, depending on severity, stiffness, and patient response.
4. Phase 3: Mobility, flexibility, and segmental release
While you want control, you don’t want an overly rigid spine. It is crucial to gradually restore **mobility** in stiff segments to allow the deep multifidus to regain flexibility and adaptability.
a. Segmental mobility drills
- Gentle lumbar facet mobilizations
- Paired segmental stretching (e.g. side-bending, rotation with stabilization)
- Cat-camel, controlled lumbar flexion-extension with stabilization
b. Global flexibility work
- Hamstring, hip flexor, gluteal, quadratus lumborum stretching
- Thoracic spine mobility (extension/rotation) to offload lumbar demand
- Pelvic mobility (motion of sacroiliac joints)
c. Dynamic mobility with control
- Controlled spinal flexion-extension in loaded and unloaded settings
- Pelvic tilts with isometric stabilization
- Progressive integration of movement in multiple planes while maintaining multifidus engagement
5. Phase 4: Strength, endurance & functional integration
Once the multifidus control is re-established and stiffness reduced, you can build resilience, endurance, and strength— always ensuring the deep system remains primary.
a. Endurance and repeated low-load work
- Sustained isometric holds (e.g. bird-dog holds, side planks with control)
- Low-resistance, high-repetition core work
- Integrate with breathing and postural control
b. Functional strengthening & loading
- Progressive loaded trunk exercises (e.g. cable rotations with controlled core)
- Compound lifts (deadlifts, squats) with strict core engagement and technique coaching
- Plyometric and sport-specific drills (jumping, cutting, twisting) with neuromuscular control emphasis
c. Load progression & periodic assessments
- Increase training load gradually, monitor for flare-ups
- Use periodic re-evaluation (stiffness, activation, function) to guide progression
- Incorporate variability to avoid overuse
6. Phase 5: Maintenance, injury prevention & return to sport
Even once symptoms resolve, ongoing maintenance is critical in athletes. The stiff pattern may recur under overload. Strategies include:
Periodic motor control refreshers (e.g. multifidus “tuning” sessions)
- Integration of multifidus activation in warm-up and cool-down routines
- Balanced core training (both stabilization and dynamic strength)
- Monitoring of training load, recovery, biomechanics
- Pre-season screening using elastography or functional tests (if available)
- Education on posture, lifting mechanics, movement hygiene
In essence, the deep multifidus should be an ongoing “guardrail” rather than a one-time rehab target.