Overview
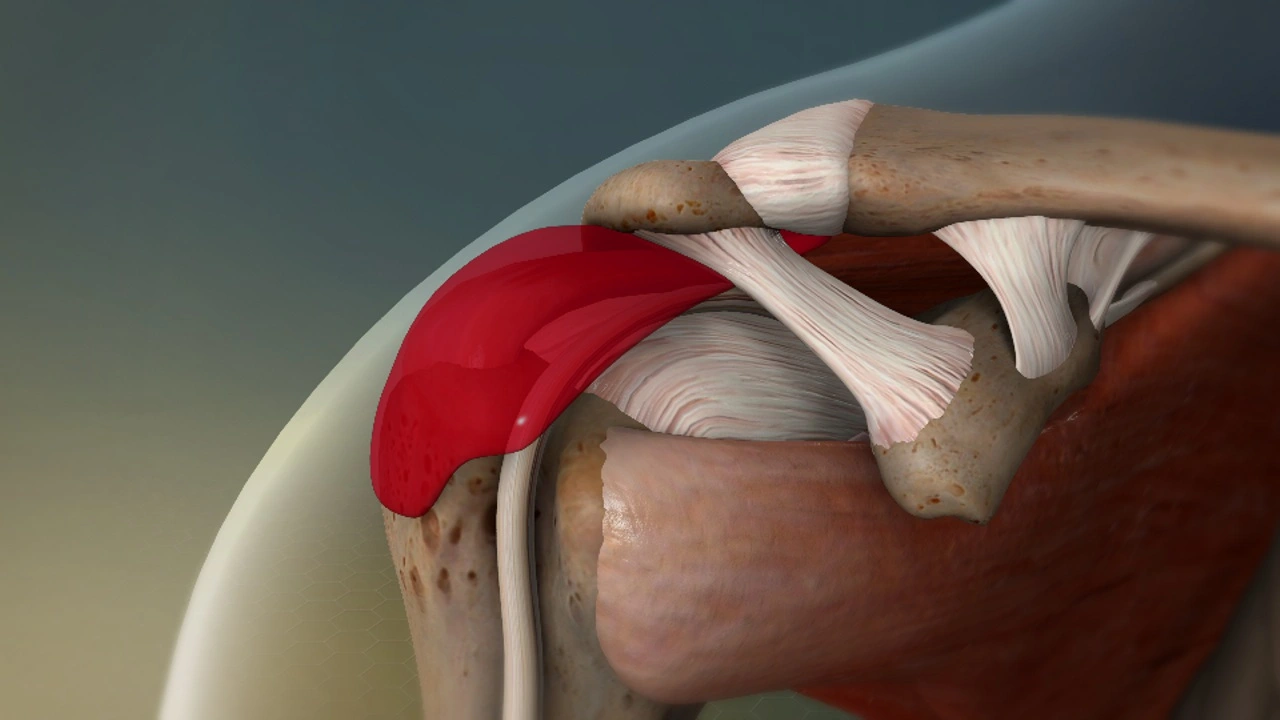
The shoulder joint is one of the most mobile yet complex joints in the human body. Its extensive range of motion allows us to perform countless daily activities, from lifting objects to throwing a ball. However, this very mobility also makes the shoulder susceptible to several inflammatory and overuse conditions. One such painful and often overlooked condition is Subdeltoid bursitis.
Subdeltoid bursitis refers to inflammation of the subdeltoid bursa, a small, fluid-filled sac that lies between the deltoid muscle and the shoulder joint capsule. The bursa acts as a cushion, reducing friction between muscles, tendons, and bones during movement. When it becomes inflamed, swollen, or irritated, shoulder mobility is restricted and pain intensifies, especially during lifting or overhead activities.
At DMPhysios, a leading physiotherapy clinic located in Noida that specializes in spine and sports conditions with a patient-centered rehabilitation approach, we often treat individuals suffering from Subdeltoid bursitis helping them regain pain-free movement through personalized physiotherapy programs. Understanding the underlying causes, symptoms, and treatment options is the first step toward effective recovery.
Symptoms
The symptoms of Subdeltoid bursitis can vary from mild discomfort to severe pain, depending on the extent of inflammation. The onset can be gradual or sudden, particularly after repetitive overhead activity or shoulder trauma. Common symptoms include:
- Pain in the outer shoulder region:
The hallmark symptom of Subdeltoid bursitis is a dull, aching pain on the outer aspect of the shoulder that may radiate down the upper arm. The pain often worsens when the arm is lifted away from the body or during overhead movements. - Tenderness and swelling:
There may be noticeable tenderness upon touching the deltoid area, and swelling might be felt beneath the muscle due to fluid accumulation in the bursa. - Limited range of motion:
Movements such as abduction, flexion, or rotation of the shoulder can become restricted and painful. - Pain at night or when lying on the affected side:
Many patients with Subdeltoid bursitis find it difficult to sleep due to pain when pressure is applied to the shoulder. - Weakness in the shoulder:
Prolonged inflammation can lead to secondary weakness of the rotator cuff and deltoid muscles due to pain inhibition.
If left untreated, Subdeltoid bursitis can lead to chronic inflammation, scar tissue formation, and even impingement-like symptoms that significantly limit shoulder function.
Types of Subdeltoid Bursitis
While Subdeltoid bursitis is generally classified as an inflammatory condition, it can be further described based on its underlying cause:
- Acute Subdeltoid Bursitis:
Caused by a sudden injury, infection, or overuse. It presents with sharp pain, redness, and warmth. - Chronic Subdeltoid Bursitis:
This develops gradually due to repetitive strain, postural issues, or degenerative shoulder conditions. The pain is often dull and persistent. - Septic Subdeltoid Bursitis:
A rare form caused by bacterial infection within the bursa, leading to severe pain, fever, and systemic symptoms. This requires medical intervention.
At DMPhysios, the physiotherapy experts carefully evaluate the type of Subdeltoid bursitis before creating a tailored rehabilitation plan that aligns with the patient’s condition, activity level, and goals.
Causes
Several factors can lead to inflammation of the subdeltoid bursa. Common causes include:
- Repetitive overhead movements:
Sports like swimming, tennis, baseball, or occupations such as painting or lifting overhead can irritate the bursa. - Direct trauma:
A fall, blow, or sudden jerk to the shoulder can cause acute inflammation. - Rotator cuff dysfunction:
Weakness or imbalance in the rotator cuff muscles can alter shoulder mechanics, leading to increased friction on the subdeltoid bursa. - Poor posture:
Forward head or rounded shoulder posture compresses the bursa over time, causing irritation. - Degenerative conditions:
Arthritis or tendon degeneration can increase mechanical stress around the shoulder joint. - Systemic inflammatory diseases:
Conditions like rheumatoid arthritis or gout may also lead to Subdeltoid bursitis due to excessive inflammatory response. - Improper exercise techniques:
Lifting heavy weights with poor form can overload the shoulder stabilizers and irritate the bursa.
Understanding the root cause is crucial for effective management. At DMPhysios, our physiotherapists conduct thorough biomechanical assessments and use diagnostic reasoning to identify the specific triggers behind each case of Subdeltoid bursitis.
Risk Factors
Certain factors increase the likelihood of developing Subdeltoid bursitis, including:
- Age above 40 years
- Occupations involving repetitive shoulder use
- Poor shoulder mechanics or muscular imbalance
- Previous shoulder injuries
- Sedentary lifestyle leading to weak stabilizing muscles
- Inflammatory or metabolic diseases (e.g., diabetes, gout)
Recognizing and modifying these risk factors early can prevent recurrence and chronic shoulder dysfunction.
Treatment
The treatment of Subdeltoid bursitis depends on its severity and underlying cause. The goal is to reduce pain and inflammation, restore normal shoulder mechanics, and prevent recurrence.
1. Rest and Activity Modification
Avoiding aggravating movements, especially overhead or heavy lifting, is essential during the acute phase. However, complete immobilization should be avoided as it can cause stiffness.
2. Cold and Heat Therapy
Cold packs during the early stages help reduce inflammation and pain. Once acute inflammation subsides, gentle heat therapy improves blood circulation and promotes healing.
3. Medications
Non-steroidal anti-inflammatory drugs (NSAIDs) may be prescribed to manage pain and swelling. In some persistent cases, corticosteroid injections into the bursa may be considered to reduce inflammation.
4. Physiotherapy Treatment
Physiotherapy plays a crucial role in both recovery and prevention of Subdeltoid bursitis, and this is where DMPhysios excels. With a patient-centered rehabilitation philosophy, DMPhysios focuses on restoring functional movement and long-term shoulder health through evidence-based interventions.
Physiotherapy Treatment
At DMPhysios, physiotherapy management of Subdeltoid bursitis follows a structured, stage-wise approach, aimed at relieving pain, restoring mobility, and enhancing strength and stability.
Stage 1: Pain Relief and Inflammation Control
- Cryotherapy: Application of ice packs for 10–15 minutes several times a day helps in reducing acute inflammation.
- Electrotherapy: Modalities like Teacr, US, TENS may be used to decrease pain and promote healing in the affected bursa.
- Gentle Passive Movements: Therapist-assisted movements help maintain mobility without overstraining the shoulder.
Stage 2: Restoration of Mobility
Once pain is controlled, the focus shifts toward regaining normal range of motion:
- Pendulum exercises to promote gentle joint movement.
- Active-assisted shoulder flexion, abduction, and rotation exercises to prevent stiffness.
- Capsular stretching to release tightness around the shoulder joint.
At DMPhysios, each exercise is prescribed with precision, ensuring that no compensatory movement patterns worsen the irritation.
Stage 3: Strengthening and Stability Training
As pain decreases and mobility improves, strengthening the rotator cuff and scapular stabilizers becomes vital:
- Isometric shoulder strengthening for deltoid and rotator cuff.
- Resistance band exercises focusing on external rotation, abduction, and scapular retraction.
- Closed-chain exercises (like wall push-ups) for dynamic stabilization.
The physiotherapists at DMPhysios emphasize functional strengthening that mimics real-life shoulder mechanics, ensuring sustainable recovery.
Stage 4: Posture and Biomechanics Correction
Improper posture, especially rounded shoulders, often contributes to Subdeltoid bursitis. Postural correction exercises, ergonomic advice, and scapular control drills are integral to treatment at DMPhysios.
Stage 5: Return to Activity and Prevention of Recurrence
Gradual reintroduction to sports or occupational activities is guided by the physiotherapist. Techniques include:
- Functional training to restore overhead movement efficiency.
- Education on lifting and reaching techniques to prevent re-injury.
- Maintenance exercise programs for long-term shoulder health.
This holistic approach ensures that patients not only recover but also build resilience against future shoulder issues.
Prevention
Prevention is always better than cure. Some effective preventive measures include:
- Maintain good posture: Avoid slouched or rounded shoulders while sitting or working.
- Warm-up before activity: Proper stretching and warm-up routines prevent sudden overload on the shoulder.
- Gradual progression of exercise intensity: Increase weights or repetitions slowly to prevent overuse injuries.
- Strengthen rotator cuff and scapular muscles: Balanced shoulder muscle strength reduces friction over the bursa.
- Ergonomic work setup: Ensure your desk or workstation allows the shoulders to stay relaxed.
- Avoid repetitive overhead strain: Take breaks during activities like painting, cleaning, or lifting.
At DMPhysios, preventive care is a cornerstone of our rehabilitation process. We educate each patient on posture, ergonomics, and self-care to maintain long-term musculoskeletal health.
Conclusion
Subdeltoid bursitis may seem like a minor irritation initially, but if ignored, it can severely impact shoulder mobility and day-to-day function. Early diagnosis, timely physiotherapy intervention, and proper postural correction are key to complete recovery.
At DMPhysios, located in Noida, our expert physiotherapists specialize in treating Subdeltoid bursitis and other spine and sports-related conditions using evidence-based, patient-centered rehabilitation programs. Whether your pain stems from overuse, poor posture, or previous injury, the goal at DMPhysios is simple to restore your shoulder’s natural function and help you move freely again.
Don’t let shoulder pain hold you back. Visit DMPhysios today for a comprehensive assessment and personalized treatment plan to overcome Subdeltoid bursitis because at DMPhysios, your recovery is our priority.