Overview
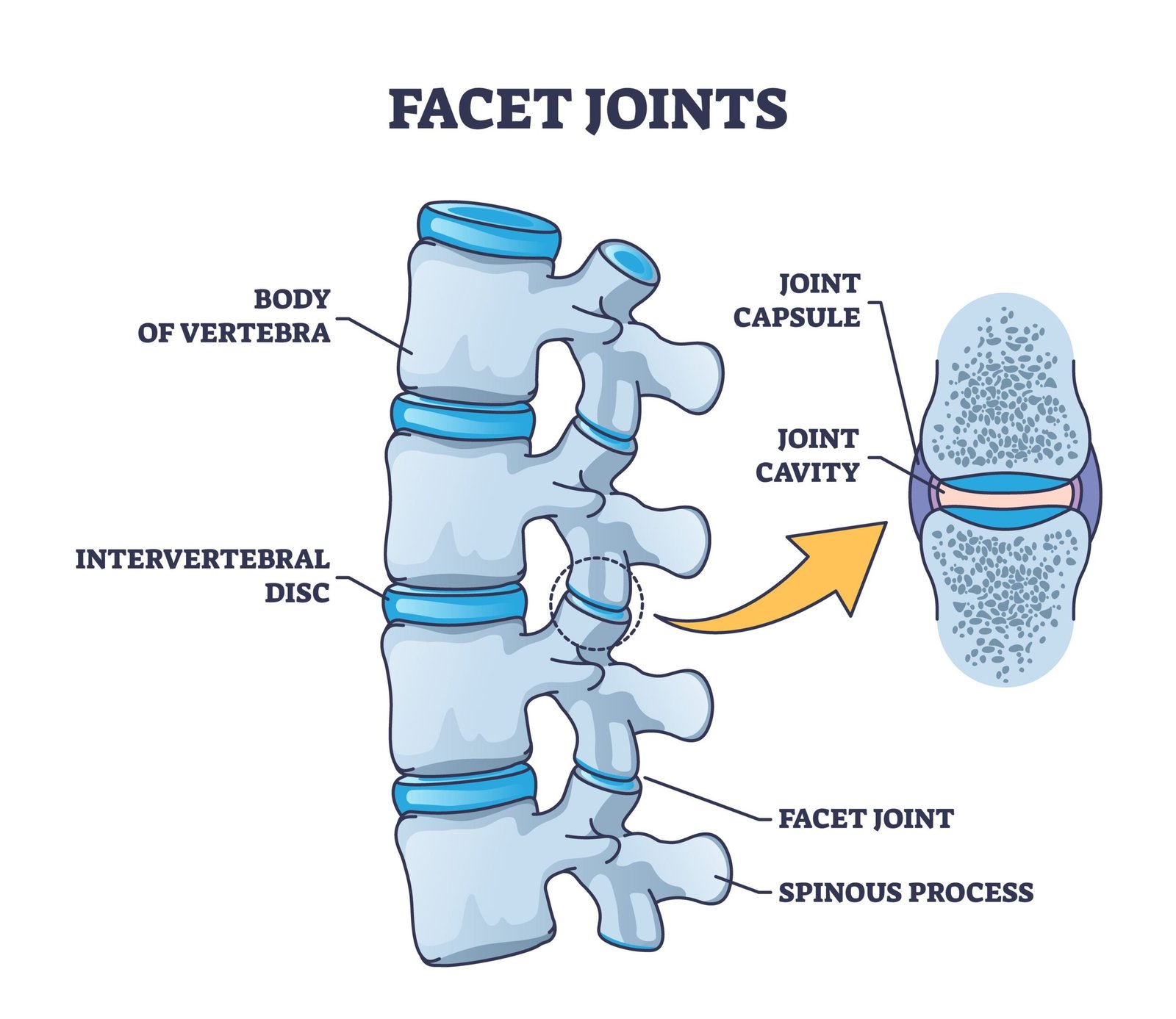
Facet Joint Syndrome, medically known as facet arthropathy or zygapophysial joint syndrome, is a frequently encountered yet often underrecognized source of spinal discomfort and chronic back pain. This condition develops when the facet joints—small but crucial articulations located on the posterior side of each vertebra—undergo degeneration, inflammation, or mechanical stress.
These joints play a vital role in guiding and limiting the motion of the spine, ensuring both stability and mobility during daily activities like bending, twisting, and standing upright. Each spinal segment from the neck (cervical spine) down to the lower back (lumbar spine) includes a pair of facet joints. When these joints become dysfunctional due to wear-and-tear, trauma, or postural imbalances, they can cause localized pain, joint stiffness, and restricted spinal movement, often radiating to nearby structures. Symptoms typically vary depending on the region involved—cervical facet joint syndrome may cause neck pain and headaches, while lumbar involvement may lead to lower back discomfort and referred pain into the buttocks or thighs.
At DMPhysios, a reputed physiotherapy clinic located in Noida that specializes in spine and sports injuries, we frequently diagnose and treat facet joint syndrome in individuals of all age groups. Our emphasis on patient-centered rehabilitation allows us to design comprehensive and customized treatment plans that not only target pain relief but also address the underlying biomechanical imbalances contributing to the condition. Whether the cause is degenerative arthritis, poor posture, or post-injury compensation, our experienced physiotherapists at DMPhysios are committed to restoring spinal function, improving mobility, and enhancing our patients’ overall quality of life through holistic care.
Symptoms of Facet Joint Syndrome
The symptoms of facet joint syndrome vary depending on the region of the spine affected. However, some hallmark signs include:
- Localized spinal pain: Often described as a dull, aching discomfort, usually near the center of the back.
- Stiffness: Most noticeable after resting for a while or first thing in the morning.
- Radiating pain: May spread to the buttocks, thighs, shoulders, or upper arms without following a specific nerve pattern.
- Pain worsens with movement: Particularly during spinal extension, twisting motions, or side bending.
- Tenderness over the affected joint.
- Muscle spasms: In the surrounding musculature as a protective response.
Patients at DMPhysios often report significant difficulty with everyday movements, such as bending over, lifting objects, or turning their head, highlighting the impact of facet joint syndrome on quality of life.
Types of Facet Joint Syndrome
Facet joint syndrome is classified based on the specific region of the spine affected. Each region presents with distinct symptoms and movement limitations. Below are the three main types:
1. Cervical Facet Joint Syndrome (Neck Region)
- Involves the facet joints in the cervical spine (C1–C7 vertebrae).
- Common symptoms:
- Localized neck pain, especially on one side.
- Pain radiating to the shoulders, upper back, or base of the skull.
- Stiffness and difficulty turning the head, especially in the morning.
- May lead to headaches (often tension-type or cervicogenic).
- Aggravating factors:
- Prolonged poor posture (e.g., looking at screens, reading).
- Sudden neck movements or sleeping in awkward positions.
- Common in office workers, students, and individuals with poor ergonomic habits.
- At DMPhysios, cervical cases are treated with posture correction, neck stabilization, and manual therapy to restore full range of motion.
2. Thoracic Facet Joint Syndrome (Mid-Back Region)
- Affects the thoracic spine (T1–T12 vertebrae), which connects to the rib cage.
- Less common, but still impactful on mobility and function.
- Common symptoms:
- Mid-back pain, often described as a dull ache.
- Pain between the shoulder blades or near the scapula.
- Discomfort when taking deep breaths or twisting the torso.
- Stiffness or tightness along the rib cage or upper back.
- Often misdiagnosed as muscular strain or costovertebral dysfunction.
- Aggravating factors:
- Poor sitting posture.
- Prolonged computer use or driving.
- At DMPhysios, careful differentiation is made to ensure accurate diagnosis and targeted thoracic mobility work.
3. Lumbar Facet Joint Syndrome (Lower Back Region)
- The most common type, affecting the lumbar spine (L1–L5 vertebrae).
- Primary cause of mechanical low back pain in adults.
- Common symptoms:
- Aching or sharp pain in the lower back, especially during or after standing.
- Referred pain to the buttocks, hips, or back of thighs.
- Stiffness and limited extension (arching the back increases pain).
- Pain that improves with sitting or forward bending.
- Often confused with disc herniation or sciatica, but without nerve-related symptoms like tingling or numbness.
- Aggravating factors:
- Standing or walking for long periods.
- Hyperextension of the spine or heavy lifting with poor mechanics.
Understanding the type is crucial for appropriate treatment—an approach consistently implemented at DMPhysios, where individual diagnosis dictates the rehabilitation path.
Causes of Facet Joint Syndrome
Several factors can lead to facet joint syndrome, including:
- Degenerative changes: Aging leads to cartilage breakdown and joint inflammation.
- Repetitive strain: Due to poor posture, heavy lifting, or twisting motions.
- Trauma or injury: Whiplash injuries or spinal compression can damage the joints.
- Disc degeneration: Loss of disc height can increase pressure on facet joints.
- Joint instability: Weak muscles or ligamentous laxity contributing to excessive spinal motion.
At DMPhysios, we thoroughly assess the contributing causes using clinical examination, posture assessment, and imaging (if needed) to ensure a targeted approach to facet joint syndrome.
Risk Factors
While anyone can develop facet joint syndrome, certain factors increase susceptibility:
- Age over 50: Due to degenerative changes in spinal structures.
- Occupational strain: Jobs involving heavy lifting, prolonged sitting, or repetitive motion.
- Sedentary lifestyle: Weak core and spinal musculature can lead to mechanical stress.
- Previous spinal injuries: Increase the risk of joint instability or early degeneration.
- Poor posture: Chronic slouching or improper biomechanics increases joint load.
Treatment Options for Facet Joint Syndrome
Management of facet joint syndrome requires a multifaceted approach aimed at reducing inflammation, restoring joint mobility, and strengthening supportive muscles. Treatment options include:
1. Medications
- NSAIDs (Non-steroidal anti-inflammatory drugs) to reduce inflammation and pain.
- Muscle relaxants in case of significant spasms.
- Analgesics for short-term pain relief.
2. Injections
- Facet joint injections with corticosteroids can reduce inflammation and provide temporary relief.
- Medial branch blocks target the nerve supply to the joint and can be diagnostic or therapeutic.
3. Radiofrequency Ablation (RFA)
A minimally invasive procedure that uses heat to disrupt nerve signals from the painful facet joint, offering longer-lasting relief.
4. Surgical Options
Rarely required, but in severe cases, spinal fusion or decompression surgeries may be considered.
While these interventions provide symptomatic relief, they must be paired with physiotherapy to address root causes—a central philosophy at DMPhysios.
Physiotherapy Treatment for Facet Joint Syndrome
At DMPhysios, we offer a personalized and evidence-based physiotherapy program to manage facet joint syndrome effectively. Our approach targets pain relief, movement restoration, muscle strengthening, and long-term prevention. Below are key components of our rehabilitation protocol:
1. Pain Management Techniques
- Manual Therapy: Gentle joint mobilizations and soft tissue release to reduce stiffness and improve mobility.
- Electrotherapy: Accelerated Healing Therapy for pain relief and tissue healing.
- Kinesiotaping: Applied strategically to offload stress from irritated joints and support proper posture.
2. Postural Correction
Facet joint syndrome is often exacerbated by poor posture. Our therapists conduct a thorough postural assessment and provide:
- Ergonomic modifications
- Posture retraining exercises
- Awareness cues for spinal alignment during daily activities
3. Core Stabilization Exercises
Strengthening deep spinal stabilizers like the transversus abdominis and multifidus is crucial. Our programs include:
- Abdominal hollowing
- Bird-dog
- Pelvic tilts
- Dead bugs
- Progressive planks
These exercises enhance spinal stability and reduce stress on the facet joints.
4. Mobility and Stretching Regimen
Restricted range of motion around the spine leads to compensations and joint overload. We employ:
- Thoracic spine mobilizations
- Cat-cow stretches
- Lumbar rotation stretches
- Piriformis and hamstring stretches
- Neck isometrics (for cervical cases)
5. Strengthening and Functional Training
Reinforcing the posterior chain and deep back muscles can relieve load from facet joints:
- Bridges and hip thrusts
- Glute strengthening
- Eccentric back extensions
- Resistance band rows
- Postural control drills
Functional exercises such as squats and lunges with correct spinal alignment are gradually introduced.
6. Education and Self-Management
Patients at DMPhysios are empowered with knowledge about their condition and equipped with home programs, dos and don’ts, and lifestyle guidance to avoid flare-ups.
Our physiotherapists believe in addressing the root cause—not just the symptoms—of facet joint syndrome. This philosophy forms the foundation of every treatment plan at our Noida clinic.
Prevention of Facet Joint Syndrome
Prevention plays a vital role in managing chronic spinal conditions. Tips for avoiding or minimizing facet joint syndrome include:
- Maintain optimal posture during work, driving, and daily activities.
- Engage in regular physical activity that includes strength and mobility training.
- Avoid prolonged static positions, especially sitting.
- Use proper lifting mechanics—lift with the legs, not the back.
- Keep a healthy weight to lessen the strain on your spine
- Incorporate spinal decompression exercises such as child’s pose or hanging from a bar.
- Stretch regularly, especially the hip flexors, hamstrings, and back muscles.
At DMPhysios, we guide each patient on personalized preventive strategies as part of a holistic recovery plan.
Conclusion
Facet joint syndrome is a leading cause of spinal pain, often resulting in restricted mobility and decreased quality of life. Early recognition, appropriate diagnosis, and a structured treatment plan—particularly through targeted physiotherapy—can dramatically improve outcomes.
At DMPhysios, located in Noida, we specialize in treating spinal conditions like facet joint syndrome with a patient-centered approach. Our team of skilled physiotherapists offers advanced rehabilitation protocols tailored to individual needs. We don’t just treat pain—we restore function, improve strength, and empower you with tools to prevent recurrence.
If you’re experiencing chronic neck or back pain that limits your movement and quality of life, don’t wait. Book a consultation with DMPhysios today and take the first step toward lasting relief and recovery.