Overview
Snapping Hip Syndrome (SHS), medically referred to as coxa saltans, is a musculoskeletal condition defined by a distinct audible or palpable snapping or clicking sensation that occurs in or around the hip joint during movement. This phenomenon most commonly presents during dynamic actions such as walking, climbing stairs, rising from a seated position, or swinging the leg, especially into flexion and extension. While the snapping may be painless and considered benign in many individuals, it can become a source of discomfort and concern when associated with pain, inflammation, or restricted mobility.
In more symptomatic cases, Snapping Hip Syndrome can lead to functional limitations, impacting an individual’s ability to perform routine daily activities or participate in sports and physical pursuits. Over time, repetitive friction or irritation caused by the snapping structure—be it a tendon, ligament, or intra-articular component—can contribute to inflammation, soft tissue damage, and chronic dysfunction if not properly managed.
This condition is particularly prevalent among athletes, dancers, gymnasts, runners, and individuals engaged in activities that involve frequent or exaggerated hip flexion and extension. Due to the repetitive motion and high demands placed on the hip joint in these populations, the risk of developing Snapping Hip Syndrome is considerably higher.
At DMPhysios, a leading physiotherapy and rehabilitation clinic based in Noida, with a core focus on spine and sports-related conditions, we understand the multifactorial nature of Snapping Hip Syndrome. Our expert physiotherapists emphasize the importance of early diagnosis, biomechanical assessment, and patient-centered rehabilitation to effectively address the root cause, alleviate symptoms, and prevent progression to more severe musculoskeletal dysfunction. With a commitment to functional recovery and individualized care, DMPhysios offers evidence-based, holistic treatment protocols that restore mobility, strength, and confidence in every patient.
Symptoms
The primary symptom of Snapping Hip Syndrome is the characteristic “snap” felt or heard in the hip. However, other symptoms may accompany this condition:
- Audible or palpable snapping sensation in the hip
- Pain or discomfort, especially during physical activity
- A sense of the hip catching or locking
- Localized tenderness over the front, side, or back of the hip
- Tightness in muscles such as the hip flexors or the iliotibial (IT) band is often present
- Reduced range of motion or flexibility
- Weakness around the hip or pelvis in chronic cases
In many cases, the snapping can be reproduced by moving the leg in certain ways, which helps with diagnosis. At DMPhysios, our physiotherapists use movement analysis and functional assessment to identify the precise source of snapping and pain.
Types of Snapping Hip Syndrome
Snapping Hip Syndrome can be categorized based on the anatomical structure involved in the snapping. There are three primary types:
1. External Snapping Hip
This is the most common form and occurs when the iliotibial band (ITB) or the gluteus maximus tendon snaps over the greater trochanter (bony prominence on the side of the femur). It is commonly seen in runners and dancers.
2. Internal Snapping Hip
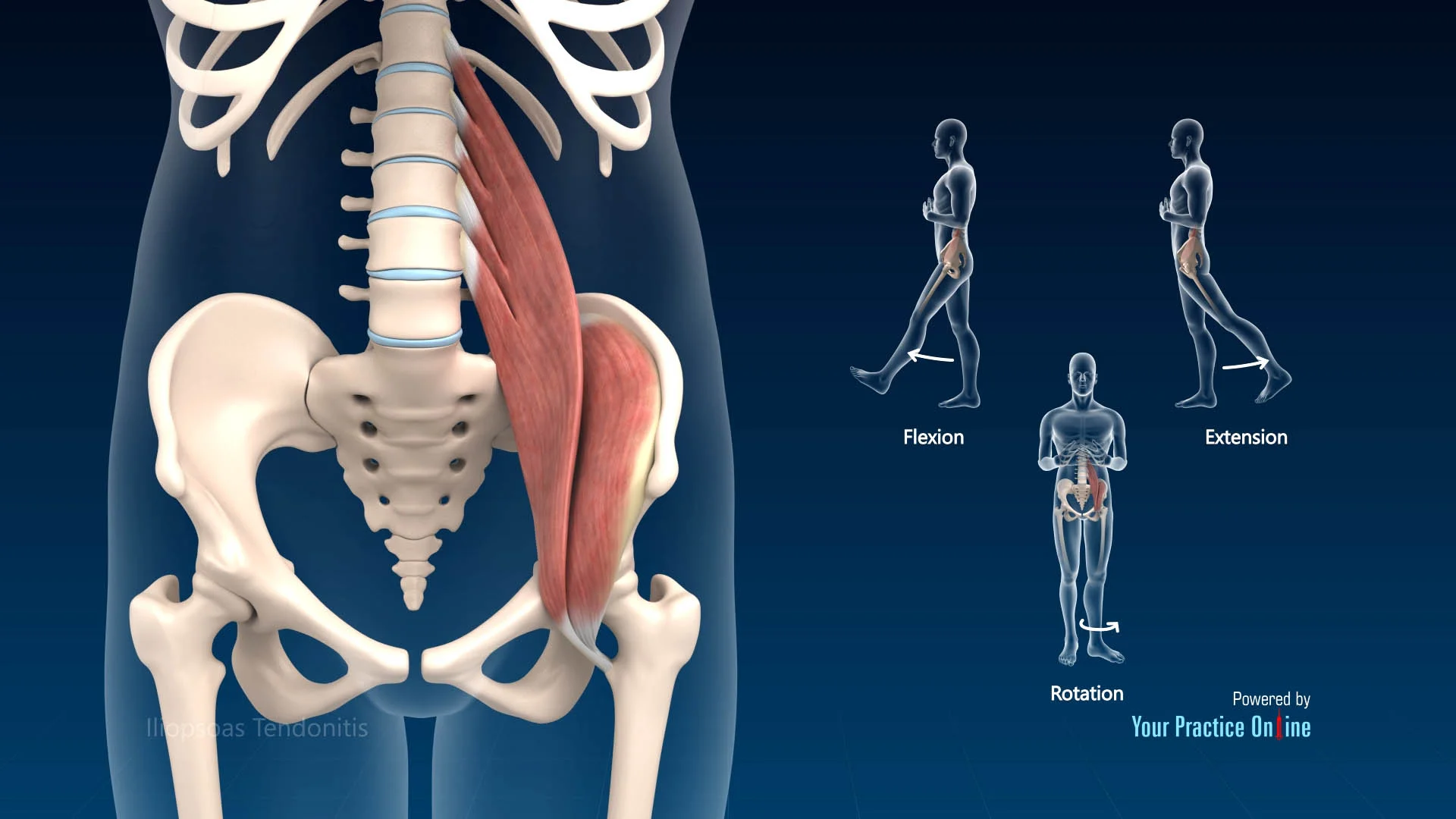
In this type, the iliopsoas tendon snaps over bony structures like the iliopectineal eminence or the femoral head. The snapping typically occurs at the front of the hip and is often described as a deep, internal click or sensation.
3. Intra-articular Snapping Hip
This form is less common and involves structural issues within the hip joint itself, such as labral tears, loose bodies, or cartilage damage. It usually presents with deep joint pain and mechanical symptoms like locking or giving way.
Understanding the specific type of Snapping Hip Syndrome is crucial for effective management. At DMPhysios, we use clinical tests and imaging as needed to distinguish between these types and tailor rehabilitation accordingly.
Causes
The root cause of Snapping Hip Syndrome often lies in repetitive movement, muscle imbalance, or anatomical variations. Common causes include:
- Tightness of the iliotibial band or iliopsoas muscle
- Overuse from sports or repetitive activities
- Muscle imbalances around the hip and pelvis
- Weakness in stabilizing muscles like the gluteus medius
- Structural abnormalities such as leg length discrepancy
- Intra-articular pathology (e.g., labral tear, synovitis)
- Previous injuries leading to altered biomechanics
At DMPhysios, we believe in addressing the underlying biomechanical dysfunctions contributing to Snapping Hip Syndrome, ensuring a holistic and lasting solution for each patient.
Risk Factors
Several risk factors can predispose an individual to Snapping Hip Syndrome:
- Participation in sports involving repetitive hip flexion (e.g., dancing, running, soccer)
- Poor flexibility or lack of dynamic stretching
- Muscle imbalances in the hip-pelvis-lumbar complex
- Improper training techniques or overtraining
- Previous hip or lower back injuries
- Anatomical variations such as a shallow acetabulum
Early identification of risk factors is essential in preventing this condition, especially in athletes. At DMPhysios, our patient-centered approach includes education, biomechanical assessment, and preventive strategies for at-risk individuals.
Treatment
The approach to treating Snapping Hip Syndrome varies based on its underlying type and the intensity of the symptoms. Most cases respond well to conservative management, while surgical intervention is rarely required. The treatment approach generally includes:
1. Rest and Activity Modification
Reducing or avoiding activities that provoke the snapping helps in managing inflammation and pain, especially in the acute phase.
2. Ice and Anti-inflammatory Medications
Ice packs and NSAIDs can help reduce pain and swelling in symptomatic cases.
3. Stretching and Strengthening Exercises
A structured exercise program focusing on stretching tight structures (iliopsoas, ITB) and strengthening weak stabilizers (gluteus medius, deep hip rotators) is key.
4. Manual Therapy
Hands-on techniques by trained physiotherapists at DMPhysios can release tight tissues, improve joint mobility, and correct movement dysfunctions.
5. Corticosteroid Injections
For cases that do not respond to conservative measures, corticosteroid injections may be considered to reduce inflammation, especially when intra-articular structures are involved.
6. Surgical Intervention
Rarely, when conservative treatment fails and intra-articular pathology is confirmed, surgical options like labral repair or tendon release may be considered.
However, most individuals recover fully with a structured physiotherapy program. That’s where DMPhysios, a trusted name in Noida for spine and sports conditions, plays a pivotal role in rehabilitation.
Physiotherapy Treatment
Physiotherapy is the cornerstone of recovery from Snapping Hip Syndrome. At DMPhysios, our expert physiotherapists provide individualized and evidence-based treatment tailored to each type of SHS. Here’s how our approach works:
1. Initial Assessment
- Thorough biomechanical analysis of the hip, pelvis, and spine
- Identification of movement patterns that provoke symptoms
- Functional testing to assess muscle strength, flexibility, and coordination
2. Manual Therapy Techniques
- Myofascial release of iliopsoas or ITB
- Soft tissue mobilization to reduce tightness and improve glide
- Joint mobilizations for lumbar spine, SI joint, and hip joint
3. Stretching Program
- Dynamic and static stretches for:
- Iliopsoas
- ITB and tensor fascia lata
- Quadriceps and hamstrings
- Piriformis and gluteal muscles
4. Strengthening Exercises
- Focus on hip abductors (gluteus medius and minimus)
- Core stabilization exercises
- Closed-chain and proprioceptive drills
- Progressions using resistance bands and weights
5. Neuromuscular Re-education
- Correct faulty movement patterns
- Enhance muscle firing sequence for dynamic control
- Improve balance and coordination
6. Gait and Postural Correction
- Gait retraining to reduce hip stress
- Postural awareness to correct lumbar lordosis or pelvic tilt
7. Functional Training
- Sport-specific drills
- Return-to-sport criteria assessment
- Plyometric training (for athletes)
Every physiotherapy session at DMPhysios is patient-centric, with ongoing reassessment to ensure optimal progress and functional recovery.
Prevention
Prevention of Snapping Hip Syndrome focuses on addressing biomechanical imbalances and optimizing movement. Preventive strategies include:
- Regular stretching of hip flexors and ITB
- Strength training for gluteal and core muscles
- Avoiding overtraining and allowing adequate recovery
- Using proper footwear and training techniques
- Incorporating dynamic warm-up and cool-down routines
- Addressing any postural or alignment issues early
At DMPhysios, our preventive rehab programs are customized for athletes and active individuals to reduce injury risk and enhance performance.
Conclusion
Snapping Hip Syndrome may begin as a minor nuisance, but if left untreated, it can escalate into a painful, performance-limiting condition. Identifying the type and cause is critical to successful treatment. Through conservative care, especially individualized physiotherapy, most people can achieve full recovery and return to their activities without pain or limitation.
If you’re experiencing snapping sensations in your hip or discomfort during movement, don’t ignore it. Let the experts at DMPhysios, Noida’s trusted clinic for spine and sports rehabilitation, help you with a comprehensive, patient-centered approach that not only treats your symptoms but addresses the root cause.Book your appointment today with DMPhysios and take the first step towards pain-free movement and optimal performance.