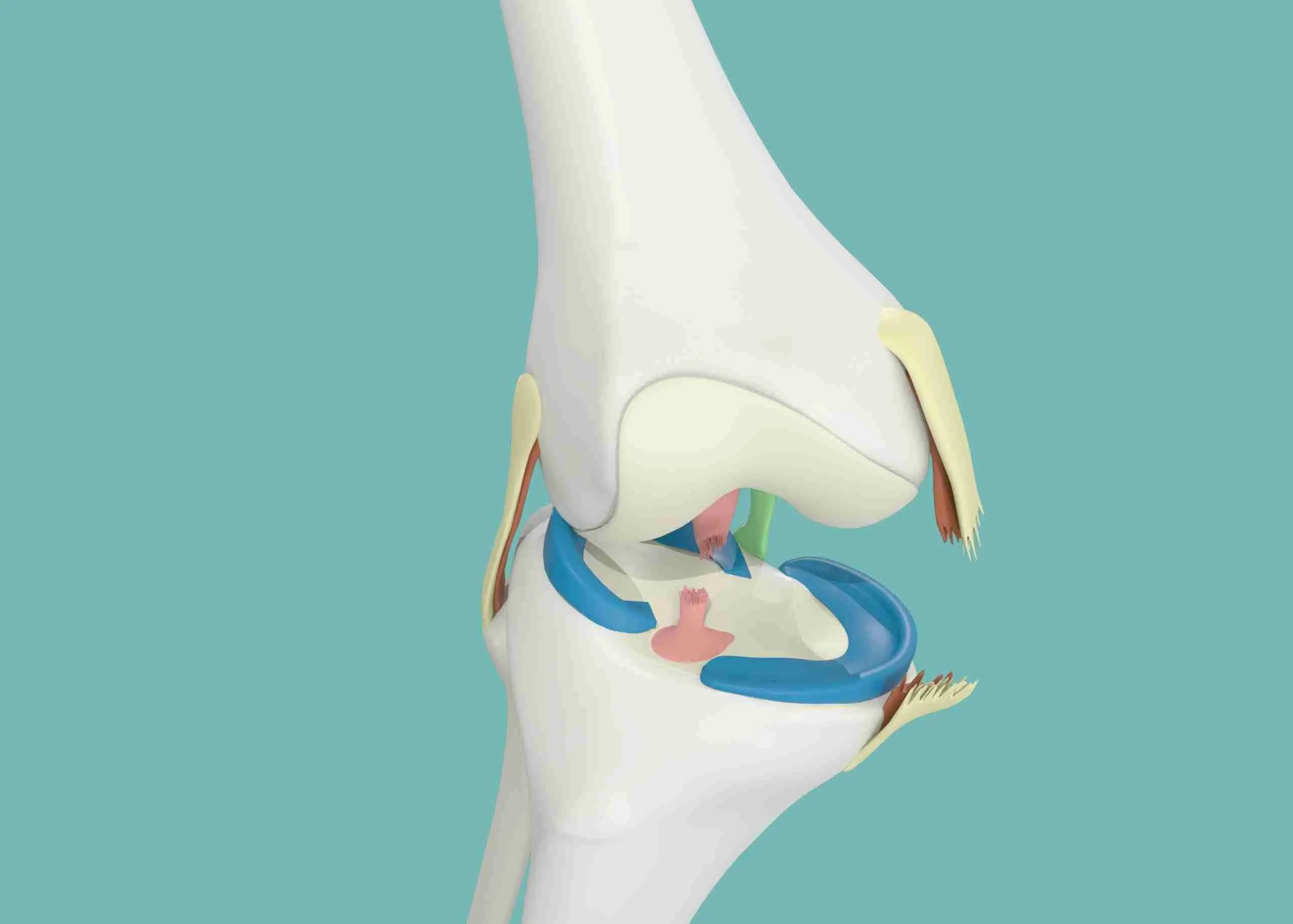
Overview
A Medial Collateral Ligament Injury, often abbreviated as MCL injury, refers to damage to one of the four major ligaments in the knee that stabilizes and supports movement.
The medial collateral ligament (MCL) runs along the inner (medial) part of the knee and connects the femur (thigh bone) to the tibia (shin bone). It plays a crucial role in preventing the knee from bending inward (valgus force) and stabilizing the joint during side-to-side motions.
A medial collateral ligament injury can vary in severity from mild stretching (Grade I) to partial tearing (Grade II) or complete rupture (Grade III).
These injuries are most commonly seen in athletes involved in sports that demand quick direction changes, jumping, or direct contact—such as football, basketball, skiing, and wrestling. However, they can also occur due to trauma or sudden twisting movements in non-athletes.
At DMPhysios, a Noida-based clinic renowned for treating spine and sports conditions with patient-centered rehabilitation, we frequently manage patients suffering from medial collateral ligament injuries through personalized treatment protocols and advanced physiotherapy techniques.
Symptoms of Medial Collateral Ligament Injury
The presentation of a medial collateral ligament injury largely depends on the extent of the damage. Common signs and symptoms include:
- Discomfort or pain located on the inner (medial) aspect of the knee
- Swelling and inflammation within a few hours post-injury
- A feeling of instability or “giving way” while walking or pivoting
- Stiffness and difficulty bending or straightening the knee
- Bruising around the medial knee area
- Tenderness to touch along the ligament
- Difficulty bearing weight, especially in higher-grade tears
Early diagnosis and proper management at clinics like DMPhysios in Noida can significantly improve outcomes and prevent chronic knee instability.
Types of Medial Collateral Ligament Injury
Medial Collateral Ligament (MCL) injuries are categorized according to the extent of ligament damage:
Grade I – Mild Sprain
- The ligament is overstretched but not torn.
- Mild tenderness and minimal swelling.
- Usually heals with conservative care in 1–2 weeks.
Grade II – Partial Tear
- A portion of the ligament fibers are torn.
- Moderate pain and swelling.
- Some instability may be present.
- Recovery may take 3–4 weeks with structured physiotherapy.
Grade III – Complete Tear
- The ligament is completely ruptured.
- Severe pain, swelling, and significant instability.
- Often requires bracing and a longer rehabilitation period.
- Surgery is rarely needed unless combined with other ligament injuries (e.g., ACL).
At DMPhysios, our experienced physiotherapists provide individualized care tailored to the specific grade of the medial collateral ligament injury, ensuring optimal recovery and return to function.
Causes of Medial Collateral Ligament Injury
A medial collateral ligament injury typically occurs when the knee is subjected to excessive force from the outside (lateral side), pushing the knee inward. Common causes include:
- Impact to the outer side of the knee, often occurring during contact sports
- Sudden twisting or turning movements
- Slips and falls, especially on uneven ground
- Improper landing mechanics during jumps
- Overuse or repetitive stress on the knee joint
Such injuries are especially prevalent in athletes, although they can also affect non-athletes through daily activities or accidents.
Risk Factors
Several factors can increase the likelihood of sustaining a medial collateral ligament injury, including:
- Participation in high-impact or contact sports (football, rugby, skiing)
- Previous history of knee injuries
- Poor neuromuscular control or improper biomechanics
- Inadequate warm-up and stretching routines
- Muscle imbalances (e.g., weak quadriceps or hamstrings)
- Poor footwear or uneven playing surfaces
At DMPhysios, we emphasize thorough movement assessments and risk profiling to help our clients understand and mitigate these risks.
Treatment Options for Medial Collateral Ligament Injury
Treatment for a medial collateral ligament injury varies based on the severity of the damage. Fortunately, most MCL injuries respond well to conservative (non-surgical) treatment. Key approaches include:
1. Rest and Activity Modification
- Avoiding activities that strain the knee
- Using crutches temporarily if weight-bearing is painful
2. Ice Application
- Reduces swelling and pain during the initial 48–72 hours
3. Compression and Elevation
- Wearing a knee sleeve or elastic bandage
- Elevating the leg to reduce inflammation
4. Bracing
- Functional knee braces offer support, especially for Grade II and III injuries
- Aids in stabilizing the knee and minimizing the risk of additional injury
5. Pain Management
- Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen
- In some cases, corticosteroid injections for persistent inflammation
Surgery is seldom required for isolated MCL injuries. However, if a medial collateral ligament injury occurs alongside damage to other structures such as the ACL or meniscus, surgery may be advised.
Physiotherapy Treatment
At DMPhysios, our expert physiotherapists design customized rehabilitation programs that evolve through distinct phases to ensure safe, complete recovery from medial collateral ligament injuries.
1. Acute Phase (0–7 days post-injury)
Goals:
- Reduce inflammation and pain
- Protect the knee joint
- Prevent muscle atrophy
Treatment Modalities:
- Cryotherapy (ice packs)
- Electrotherapy (Accelerated Healing Therapy)
- Knee brace application
- Isometric quadriceps and hamstring activation
- Gentle range-of-motion (ROM) exercises
2. Subacute Phase (1–3 weeks)
Goals:
- Restore joint mobility
- Initiate controlled loading
- Begin functional strength exercises
Physiotherapy Includes:
- Passive and active ROM exercises
- Static and dynamic balance training
- Resistance band exercises for quads, hamstrings, glutes
- Step-ups, mini squats, wall sits (pain-free)
3. Strengthening and Proprioception Phase (3–6 weeks)
Goals:
- Strengthen periarticular muscles
- Improve joint stability and neuromuscular control
Key Interventions:
- Closed kinetic chain exercises (lunges, leg presses)
- Proprioceptive training (balance board, BOSU)
- Gait retraining and treadmill walking
- Soft tissue mobilization techniques
4. Return to Sport / Function Phase (6–12 weeks)
Goals:
- Reintegrate sport-specific movements
- Minimize risk of reinjury
- Enhance dynamic control
Rehab Progression:
- Plyometric drills (jump squats, bounding)
- Agility training (ladder, cone drills)
- Sprinting and directional changes
- Functional testing and re-evaluation
At DMPhysios, every stage of medial collateral ligament injury rehabilitation is carefully monitored. Our Noida-based clinic emphasizes evidence-based protocols, constant progress tracking, and patient education to ensure the best possible outcomes.
Prevention of Medial Collateral Ligament Injury
While it may not be possible to prevent every medial collateral ligament injury, the risk can be significantly reduced through the following measures:
- Proper Warm-Up: Always warm up before physical activity to prepare muscles and ligaments.
- Strength Training: Regular exercises targeting the quadriceps, hamstrings, calves, and hip stabilizers.
- Flexibility Work: Regular stretching of the hamstrings, quadriceps, and adductors.
- Sports Technique Correction: Addressing faulty movement patterns, improper landing mechanics, and excessive inward knee collapse.
- Balance and Proprioception Drills: Especially crucial for athletes recovering from previous injuries.
- Appropriate Footwear: Using sport-specific and terrain-appropriate shoes with good support.
DMPhysios also offers injury prevention programs for athletes and active individuals in Noida, helping reduce the occurrence of medial collateral ligament injuries and other knee pathologies.
Conclusion
A medial collateral ligament injury can be a painful and function-limiting condition, but with the right treatment and rehabilitation plan, full recovery is not only possible—it’s expected. Early diagnosis, appropriate bracing, and a tailored physiotherapy program are the cornerstones of successful management.
At DMPhysios, we specialize in helping patients regain mobility, function, and strength following medial collateral ligament injuries. Our Noida-based clinic, renowned for managing spine and sports injuries, is committed to offering patient-centered rehabilitation backed by clinical expertise and modern therapeutic techniques.
Whether you’re an athlete recovering from a sprain or someone dealing with a traumatic MCL tear, DMPhysios is here to guide you through every phase of your healing journey.If you or someone you know is suffering from a medial collateral ligament injury, don’t delay your recovery. Visit DMPhysios in Noida for an expert evaluation and a personalized physiotherapy program that puts you at the center of care. Book your consultation today and take the first step toward a stronger, more stable knee.