Overview
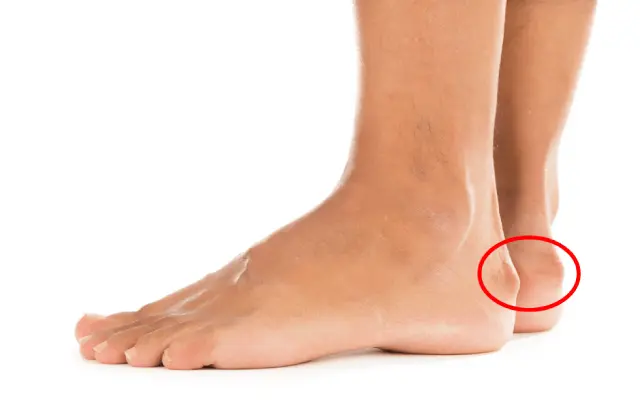
Haglund’s Deformity, often referred to as a “pump bump,” is a painful orthopedic condition marked by a noticeable bony enlargement at the back of the heel, precisely near the attachment site of the Achilles tendon. This bony overgrowth can cause continuous irritation to the surrounding soft tissues, including the retrocalcaneal bursa and the Achilles tendon itself. Over time, this irritation may trigger inflammation, swelling, and persistent discomfort, which often makes even simple day-to-day activities—such as standing for long periods, walking, or running—challenging and uncomfortable.
The condition tends to worsen when individuals wear stiff or rigid footwear, such as high-heeled shoes, formal shoes with hard backs, or tight-fitting sports shoes. These types of footwear press against the heel prominence, increasing friction and leading to further pain and irritation. While Haglund’s Deformity is not a serious or life-threatening medical issue, its effect on mobility, athletic participation, and overall quality of life can be significant, particularly if it is neglected or left untreated for an extended period.
This deformity is frequently seen in active individuals and athletes, but it can affect anyone, especially those with poor foot biomechanics or a predisposition due to genetic foot structure. If not managed properly, the ongoing irritation may progress to chronic bursitis or Achilles tendinopathy, making the condition harder to treat.
At DMPhysios, a leading physiotherapy clinic in Noida with a specialized focus on spine and sports conditions, the treatment approach for Haglund’s Deformity is patient-centered and comprehensive. The clinic’s team of expert physiotherapists works closely with each patient to not only relieve pain and restore mobility but also to address underlying biomechanical issues. By combining advanced physiotherapy techniques, targeted exercise programs, and long-term preventive strategies, DMPhysios ensures that patients can return to their activities with reduced risk of recurrence and improved quality of life.
Symptoms
The signs of Haglund’s Deformity often develop gradually, though in some cases, pain may appear suddenly following repetitive stress or prolonged shoe use. Common symptoms include:
- Prominent bony lump at the back of the heel.
- Heel pain and tenderness, especially where the Achilles tendon attaches.
- Swelling and redness around the heel due to irritation of soft tissues.
- Stiffness in the ankle and Achilles tendon, particularly in the morning or after rest.
- Pain while wearing shoes, especially rigid-backed footwear.
- Difficulty in physical activities such as running, jumping, or even walking long distances.
If untreated, Haglund’s Deformity may lead to secondary issues like Achilles tendinitis or chronic bursitis, further complicating recovery.
Types of Haglund’s Deformity
While Haglund’s Deformity is generally classified as one condition, it can present differently depending on the structures involved:
- Isolated Bony Enlargement – Primarily involving the heel bone prominence without significant tendon involvement.
- Haglund’s Syndrome – When Haglund’s Deformity occurs along with retrocalcaneal bursitis and Achilles tendinitis.
- Bilateral Haglund’s Deformity – Where both heels are affected, which is common in individuals with poor biomechanics or repetitive stress patterns.
Understanding the type and severity helps clinicians at DMPhysios design individualized rehabilitation programs tailored to each patient.
Causes
The development of Haglund’s Deformity is multifactorial and can be attributed to a combination of biomechanical, genetic, and lifestyle-related factors:
- Foot structure – High arches (pes cavus) increase heel pressure, predisposing individuals to this condition.
- Tight Achilles tendon – Increases tension on the heel bone and contributes to irritation.
- Improper footwear – Rigid-backed shoes, like pumps or stiff sneakers, rub against the heel and worsen the deformity.
- Genetics – Family history of foot deformities or abnormal gait patterns increases susceptibility.
- Overuse or repetitive stress – Common in runners, athletes, or individuals with physically demanding jobs.
- Poor biomechanics – Gait abnormalities, such as excessive supination, can heighten friction at the heel.
Risk Factors
Certain groups are more vulnerable to Haglund’s Deformity:
- Women who frequently wear high heels (“pump bump” origin).
- Athletes involved in running, football, or basketball.
- Individuals with high-arched feet or flat-foot deformities.
- Middle-aged adults with cumulative wear and tear.
- Workers requiring prolonged standing in tight or safety footwear.
At DMPhysios, clinicians emphasize identifying these risk factors early to prevent the condition from worsening.
Treatment
Treatment for Haglund’s Deformity depends on its severity. Most patients benefit from conservative approaches before surgical options are considered.
Non-Surgical Treatments:
- Footwear modifications – Using open-back shoes or shoes with softer heels to reduce friction.
- Heel pads or orthotics – Cushions that reduce pressure and correct biomechanics.
- Icing – To reduce inflammation and pain after activity.
- Anti-inflammatory medications – NSAIDs may be prescribed for pain relief.
- Immobilization – In severe cases, short-term bracing or casting to reduce strain.
Surgical Treatments:
When conservative methods fail, surgical correction may be recommended. This typically involves removing the bony prominence and addressing any associated tendon damage. However, surgery is often the last resort and requires extensive rehabilitation.
Physiotherapy Treatment
Physiotherapy plays a central role in both conservative management and post-surgical recovery of Haglund’s Deformity. At DMPhysios, treatment is patient-centered and tailored to restore normal function, reduce pain, and prevent recurrence.
1. Pain Management
- Cryotherapy – Ice packs or cold therapy reduce acute inflammation.
- Accelerated Healing Therapy – Enhances blood circulation and accelerates healing.
2. Stretching Exercises
- Calf stretches – Lengthening the gastrocnemius and soleus muscles to reduce Achilles tendon strain.
- Heel cord stretches – Performed against a wall to relieve tension at the heel.
- Plantar fascia stretching – Helpful when heel pain overlaps with plantar fasciitis.
3. Strengthening Exercises
- Eccentric calf raises – Strengthens the Achilles tendon and reduces recurrence risk.
- TheraBand resistance training – Improves ankle stability and overall foot mechanics.
- Foot intrinsic strengthening – Exercises like towel scrunches to enhance arch support.
4. Manual Therapy
- Soft tissue mobilization – Reduces muscle tightness in the calf and Achilles region.
- Joint mobilizations – Improves ankle mobility and corrects restricted dorsiflexion.
5. Biomechanical Correction
- Gait training – To correct faulty movement patterns.
- Custom orthotics – Designed to offload stress from the heel and correct foot alignment.
6. Activity Modification
- Guidance on reducing aggravating activities, switching footwear, and gradual return to sports.
7. Post-Surgical Physiotherapy
If surgery is required, rehabilitation focuses on:
- Early range of motion exercises.
- Gradual weight-bearing progression.
- Strengthening of calf and ankle muscles.
- Return-to-sport programs under physiotherapist guidance.
At DMPhysios, the physiotherapy approach is not just about treating symptoms—it emphasizes long-term prevention through education, posture correction, and strengthening strategies.
Prevention
While not every case of Haglund’s Deformity can be avoided, preventive strategies significantly reduce risk:
- Wear appropriate footwear with soft backs and adequate cushioning.
- Stretch regularly, especially calves and Achilles tendons.
- Avoid excessive high heel use to reduce heel pressure.
- Maintain proper foot biomechanics through orthotics if needed.
- Gradually increase activity levels in sports or exercise routines.
- Seek early intervention if heel pain begins, rather than waiting until it worsens.
Conclusion
Haglund’s Deformity may seem like a minor issue at first, but if ignored, it can significantly affect mobility, daily activities, and athletic performance. With proper diagnosis, timely intervention, and comprehensive physiotherapy, most individuals recover without needing surgery.
At DMPhysios, located in Noida and specializing in spine and sports conditions, patients receive individualized, patient-centered rehabilitation for Haglund’s Deformity and other musculoskeletal problems. The clinic combines advanced physiotherapy techniques, education, and preventive care to ensure long-term recovery and improved quality of life.If you or someone you know is struggling with persistent heel pain or suspect Haglund’s Deformity, don’t wait for it to worsen. Book a consultation with DMPhysios today and take the first step toward pain-free mobility and healthier living.