Overview
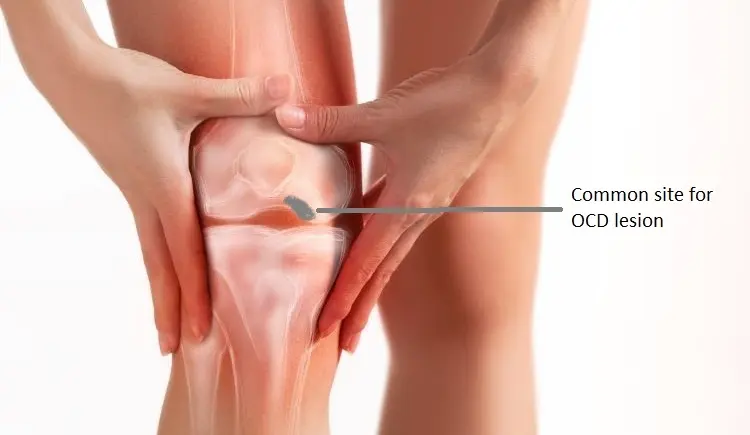
Osteochondritis Dissecans (OCD) is a relatively uncommon but clinically important joint disorder in which a fragment of bone and its overlying cartilage gradually lose strength due to reduced blood supply. As circulation diminishes, the affected section of bone weakens and may eventually separate partially or completely from the surrounding joint surface. This process leads to irritation, pain, swelling, stiffness, and at times mechanical symptoms such as joint locking or catching.
Although Osteochondritis Dissecans can occur in several joints of the body, it is most frequently seen in the knee, particularly in the femoral condyles. It may also affect the ankle, elbow, and, less commonly, other load-bearing joints. The impact of the condition varies: some individuals experience mild discomfort, while others struggle with significant mobility restrictions and instability.
If not identified and managed in time, Osteochondritis Dissecans can lead to chronic joint dysfunction, progressive degeneration of cartilage, and even early-onset osteoarthritis. This makes timely recognition and intervention essential, especially for athletes, physically active individuals, and adolescents who are still in their growth phase. The condition is of special concern in sports medicine and physiotherapy because repetitive stress, overuse injuries, and growth-related changes often play a key role in its development.
Comprehensive care from a multidisciplinary perspective is vital. Clinics such as DMPhysios in Noida, which specialize in spine and sports conditions and emphasize patient-centered rehabilitation, provide tailored treatment plans. Their expertise ensures that each patient receives a combination of medical evaluation, physiotherapy, and long-term preventive guidance, helping restore joint function and prevent recurrence.
Symptoms
The symptoms of Osteochondritis Dissecans vary depending on the severity of the lesion and whether the fragment of bone/cartilage has detached. Common symptoms include:
- Joint Pain: Usually worsens with physical activity and improves with rest.
- Swelling and Tenderness: Particularly after exercise or prolonged activity.
- Joint Locking or Catching: If the loose fragment interferes with smooth joint movement.
- Decreased Range of Motion: Stiffness or inability to fully extend or bend the joint.
- Weakness or Instability: Feeling that the joint may “give way” during activity.
- Clicking or Grinding Sensation: Especially when the fragment has separated.
In children and adolescents, pain may initially seem mild but can progress rapidly if ignored.
Types of Osteochondritis Dissecans
Osteochondritis Dissecans can be classified based on stability and severity:
- Stable OCD:
- The bone and cartilage are damaged but remain in place.
- More common in younger patients, often heals with conservative treatment.
- Unstable OCD:
- The fragment is partially detached or completely loose inside the joint.
- Causes mechanical symptoms like locking and requires surgical intervention.
Additionally, OCD may be staged radiologically:
- Stage I: Small lesion, intact cartilage.
- Stage II: Larger lesion, partially detached.
- Stage III: Fragment completely detached but not displaced.
- Stage IV: Fragment detached and displaced within the joint (loose body).
Causes
While the exact cause of Osteochondritis Dissecans is not fully understood, several contributing factors are recognized:
- Repetitive Stress: Microtrauma from sports such as football, basketball, or gymnastics.
- Ischemia (Poor Blood Supply): Reduced circulation to a section of subchondral bone.
- Genetic Predisposition: Family history may increase risk.
- Rapid Growth in Adolescents: Growth spurts can stress developing bones.
- Previous Injury: Direct trauma to the joint can initiate OCD.
Risk Factors
Individuals more likely to develop Osteochondritis Dissecans include:
- Adolescents and Young Adults: Especially those involved in high-impact sports.
- Athletes: Particularly those in sports requiring repetitive jumping, running, or pivoting.
- Male Predominance: OCD is reported more frequently in boys.
- Family History: Genetic factors may play a role.
- Repetitive Joint Overuse: From both recreational and competitive sports.
Treatment
The treatment plan depends on the patient’s age, the stability of the lesion, and the severity of symptoms.
Non-Surgical Management
- Rest and Activity Modification: Avoiding high-impact sports.
- Immobilization: Temporary use of braces or crutches to reduce stress.
- Medications: NSAIDs to relieve pain and swelling.
- Physiotherapy: Structured programs designed to restore function (detailed later).
Surgical Management
If conservative measures fail, surgery may be required:
- Drilling (Microfracture): Stimulates blood flow to heal the lesion.
- Fixation: Securing the fragment back into place with pins or screws.
- Osteochondral Autograft/Allograft: Transplanting cartilage and bone to repair defects.
- Fragment Removal: In cases of completely detached loose bodies.
Physiotherapy Treatment
Physiotherapy plays a central role in managing Osteochondritis Dissecans, both in conservative care and post-surgical rehabilitation. At DMPhysios in Noida, patient-centered rehabilitation is prioritized, ensuring recovery is tailored to individual needs.
Goals of Physiotherapy:
- Reduce pain and inflammation.
- Restore joint range of motion.
- Strengthen surrounding muscles for stability.
- Correct biomechanical issues to prevent recurrence.
- Facilitate safe return to sports.
Stages of Physiotherapy Management:
1. Acute Phase (Pain & Inflammation Control)
- Cryotherapy: Ice packs to control swelling.
- Rest and Protected Weight Bearing: Crutches or braces.
- Gentle Passive Movements: To maintain flexibility without stressing the lesion.
2. Early Rehabilitation (Restoring Mobility & Strength)
- Range of Motion (ROM) Exercises:
- Heel slides (for knees).
- Gentle ankle pumps (for ankle OCD).
- Isometric Strengthening:
- Quadriceps sets, gluteal squeezes.
- Avoiding high-load exercises.
3. Progressive Strengthening
- Closed Kinetic Chain Exercises: Mini squats, step-ups, wall sits.
- Hip and Core Strengthening: To reduce joint stress.
- Balance and Proprioception Training: Using wobble boards, single-leg stance.
4. Functional Training
- Low-Impact Cardio: Cycling, swimming.
- Plyometric Drills: Introduced gradually for athletes.
- Sport-Specific Drills: Only when pain-free and cleared by the therapist.
5. Post-Surgical Rehabilitation (if applicable)
- Initial immobilization followed by progressive ROM.
- Gradual weight-bearing under physiotherapist supervision.
- Muscle strengthening and gait re-education.
- Advanced proprioception and return-to-sport training.
At DMPhysios, physiotherapists emphasize evidence-based rehabilitation protocols, ensuring safe recovery while addressing individual biomechanical issues.
Prevention
While not all cases can be prevented, especially those due to genetics or growth-related factors, certain strategies can reduce risk:
- Avoid Overtraining: Incorporate rest days in training schedules.
- Cross-Training: Mix sports to reduce repetitive stress.
- Proper Warm-Up & Cool-Down: Reduces strain on joints.
- Strength & Flexibility Programs: Maintain balanced muscle support.
- Early Medical Attention: Address joint pain promptly to prevent worsening.
Clinics like DMPhysios in Noida also provide injury prevention programs that help athletes identify risk factors and build resilience against conditions like Osteochondritis Dissecans.
Conclusion
Osteochondritis Dissecans is a significant joint condition that can impair mobility, athletic performance, and long-term joint health if not managed properly. Early diagnosis, appropriate treatment, and structured rehabilitation are critical to achieving full recovery.
With specialized care available at DMPhysios in Noida, patients benefit from patient-centered rehabilitation that integrates medical treatment and physiotherapy for optimal outcomes. Whether managed conservatively or surgically, physiotherapy remains the cornerstone of recovery—helping individuals return safely to daily life and sports.If you or someone you know is experiencing joint pain, swelling, or locking symptoms, don’t ignore it. Contact DMPhysios, Noida’s trusted clinic for spine and sports conditions, to receive expert guidance and a personalized rehabilitation plan.