Overview
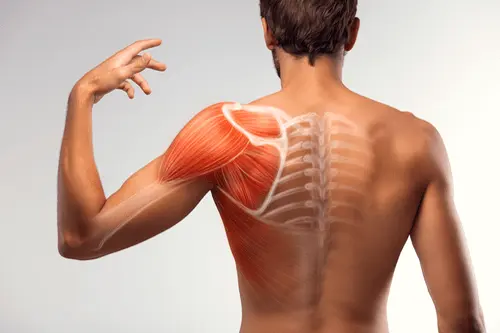
Polymyositis is a rare but potentially disabling chronic inflammatory disease that primarily targets the muscles located closest to the trunk of the body. These include the major muscle groups of the shoulders, hips, thighs, and neck. The word itself is derived from Greek: “poly” meaning many, “myo” referring to muscle, and “itis” indicating inflammation. Together, these terms describe a condition where multiple muscles become inflamed, weakened, and progressively less functional. This muscle involvement can significantly interfere with daily activities, making once-simple movements such as climbing stairs, rising from a chair, lifting objects overhead, or even turning the head and swallowing food, increasingly difficult.
As part of the group of disorders known as idiopathic inflammatory myopathies, Polymyositis is marked by progressive and symmetrical muscle weakness, meaning both sides of the body are typically affected in a fairly equal pattern. This is in contrast to temporary muscle fatigue, which improves with rest. Polymyositis does not simply cause tiredness—it creates a steady decline in muscular strength and endurance if not addressed with timely and appropriate interventions. In more advanced cases, even essential activities such as breathing or speaking may be affected if respiratory or throat muscles are involved.
The exact cause of Polymyositis remains complex and not fully understood, but it is widely believed to be an autoimmune disorder in which the immune system mistakenly attacks healthy muscle fibers. Because of its chronic nature and its impact on fundamental movements, early recognition is critical. With prompt medical attention, the damaging cycle of inflammation and weakness can be slowed, and quality of life preserved.
Successful management of Polymyositis usually requires a multidisciplinary approach, combining medical therapies with targeted rehabilitation strategies. Physicians play a role in controlling inflammation and suppressing immune overactivity, while physiotherapists and rehabilitation specialists help restore strength, endurance, and mobility. Clinics like DMPhysios in Noida, which specialize in spine and sports conditions and emphasize patient-centered rehabilitation, are uniquely equipped to design individualized therapy plans for people living with Polymyositis. Their comprehensive care helps patients not only manage the symptoms but also regain independence in their daily lives.
Symptoms
The symptoms of Polymyositis usually develop gradually over weeks or months. Early signs may be subtle and mistaken for general fatigue, but as the disease progresses, the symptoms become more apparent.
Common Symptoms:
- Muscle Weakness: Most noticeable in proximal muscles (hips, shoulders, thighs, upper arms, and neck).
- Difficulty Performing Daily Activities: Trouble climbing stairs, rising from a seated position, or lifting objects overhead.
- Fatigue and General Malaise: Persistent tiredness even after adequate rest.
- Muscle Pain and Tenderness: Although weakness is more common, some patients may experience discomfort in affected muscles.
- Difficulty Swallowing (Dysphagia): If throat muscles are affected.
- Voice Changes: Hoarseness due to weakness in throat muscles.
- Unintentional Weight Loss: In advanced or untreated cases.
- Breathing Difficulties: If respiratory muscles are affected.
Polymyositis is often accompanied by systemic symptoms such as low-grade fever, joint pain, and general stiffness. Some patients may also experience skin changes similar to dermatomyositis.
Types of Polymyositis
Unlike other myopathies, Polymyositis does not have clear subtypes, but it is sometimes classified based on associations and severity:
- Primary Polymyositis: Classic form affecting proximal muscles without other systemic involvement.
- Overlap Polymyositis: Occurs with other autoimmune diseases such as lupus, scleroderma, or rheumatoid arthritis.
- Polymyositis with Interstitial Lung Disease: Patients develop lung involvement, making the condition more severe.
- Juvenile Myositis: While dermatomyositis is more common in children, rare cases of Polymyositis are also seen.
Causes
The exact cause of Polymyositis is not fully understood, but it is generally considered an autoimmune disorder, meaning the immune system mistakenly attacks the body’s own muscle tissue.
Potential Causes and Contributing Factors:
- Autoimmune Response: T-lymphocytes attack healthy muscle fibers.
- Genetics: Family history of autoimmune diseases increases risk.
- Viral Triggers: Certain viral infections may trigger abnormal immune responses.
- Environmental Factors: Exposure to toxins or certain medications may contribute.
- Associated Autoimmune Conditions: Higher prevalence in patients with other connective tissue diseases.
Risk Factors
Certain groups of people are more likely to develop Polymyositis:
- Age: Most common between ages 30 and 60.
- Gender: Women are affected more often than men.
- Genetics: Family history of autoimmune diseases increases risk.
- Race: African Americans are more commonly affected compared to other ethnic groups.
- Other Autoimmune Diseases: Coexisting lupus, rheumatoid arthritis, or scleroderma.
- Infections: Viral infections may act as triggers.
Treatment
Treatment of Polymyositis focuses on reducing inflammation, improving muscle strength, and preventing complications. Because it is a chronic condition, treatment is usually long-term and tailored to each patient.
Medical Management:
- Corticosteroids: Prednisone is often the first-line treatment to reduce muscle inflammation.
- Immunosuppressants: Drugs like methotrexate, azathioprine, or mycophenolate mofetil are used if steroids are ineffective or cause side effects.
- Biologic Therapies: Intravenous immunoglobulin (IVIG) or biologic agents may be used in resistant cases.
- Antimalarial Drugs: Hydroxychloroquine is sometimes used if skin involvement is present.
- Symptomatic Care: Pain relievers, nutritional support, and management of swallowing or breathing difficulties.
Physiotherapy Treatment
Physiotherapy plays a central role in the long-term management of Polymyositis. Since the condition weakens muscles, physiotherapy helps restore mobility, strength, and independence in daily activities. At DMPhysios in Noida, patient-centered rehabilitation programs are specifically designed to address muscle inflammation, weakness, and functional limitations associated with Polymyositis.
Goals of Physiotherapy:
- Improve muscle strength and endurance.
- Maintain joint flexibility.
- Enhance balance and posture.
- Reduce pain and stiffness.
- Restore independence in daily living.
- Prevent long-term complications like contractures and muscle atrophy.
Detailed Physiotherapy Interventions:
1. Exercise Therapy
- Strength Training: Light to moderate resistance training with gradual progression. Focus on proximal muscles (hips, thighs, shoulders).
- Aerobic Conditioning: Low-impact activities like walking, cycling, or swimming to improve cardiovascular endurance.
- Range of Motion (ROM) Exercises: To maintain flexibility and prevent stiffness.
- Functional Exercises: Sit-to-stand training, stair climbing practice, and lifting techniques for daily independence.
2. Hydrotherapy
Exercising in water reduces strain on weak muscles while allowing gentle strengthening. This is especially beneficial for patients with severe muscle weakness or joint pain.
3. Posture and Gait Training
Weakness in trunk and hip muscles often leads to postural imbalances. Physiotherapists at DMPhysios correct gait abnormalities, reduce fall risk, and improve alignment.
4. Breathing Exercises
For patients with respiratory muscle involvement, targeted breathing exercises can enhance lung capacity and prevent breathing difficulties.
5. Pain and Fatigue Management
- Heat therapy or gentle massage to reduce muscle discomfort.
- Energy conservation techniques to balance activity with rest.
6. Assistive Devices and Education
- Use of walking aids or orthotics if needed.
- Patient education on pacing activities, ergonomic adaptations, and self-care strategies.
At DMPhysios, the rehabilitation plan for Polymyositis patients is always individualized, meaning that every patient receives a program based on their strength levels, daily limitations, and long-term goals.
Prevention
Since the exact cause of Polymyositis is not completely understood, there is no guaranteed prevention. However, risk can be reduced and progression controlled by:
- Early Diagnosis and Treatment: Seeking medical advice when unexplained muscle weakness appears.
- Regular Exercise: Engaging in supervised physiotherapy to maintain muscle health.
- Healthy Lifestyle: Balanced diet, hydration, and adequate sleep to support immune function.
- Avoiding Triggers: Limiting exposure to infections and toxic substances.
- Routine Monitoring: Regular follow-ups at a specialized rehabilitation center like DMPhysios in Noida can help prevent complications.
Conclusion
Polymyositis is a chronic inflammatory muscle disease that can significantly impact quality of life if left untreated. Characterized by progressive muscle weakness, difficulty in daily activities, and potential systemic complications, it requires timely medical and rehabilitative care. While medications reduce inflammation, physiotherapy is essential to restore strength, mobility, and independence.
At DMPhysios in Noida, a clinic specialized in spine and sports conditions, patients with Polymyositis receive patient-centered rehabilitation programs designed to improve long-term outcomes. With the right combination of medical treatment and physiotherapy, individuals can manage symptoms effectively and lead active, fulfilling lives.If you or your loved one are experiencing persistent muscle weakness or have been diagnosed with Polymyositis, don’t delay seeking professional help. Contact DMPhysios in Noida today for expert guidance, personalized physiotherapy, and comprehensive rehabilitation.