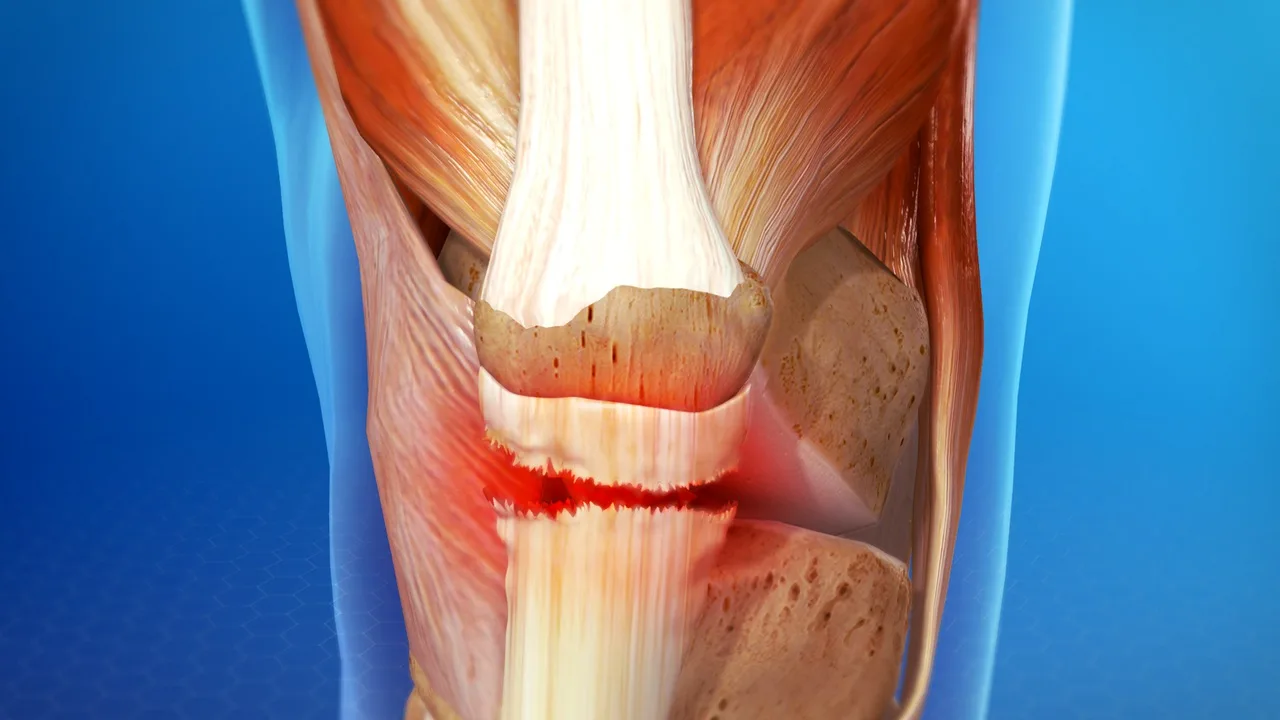
Overview
A patellar tendon rupture is one of the most serious injuries that can affect the front of the knee. It involves a complete or partial tearing of the strong tendon that links the kneecap (patella) to the shinbone (tibia). This tendon is a vital part of the knee’s extensor mechanism — the system of muscles and tendons that allows you to straighten your leg. Every time you rise from a chair, walk across a room, climb a set of stairs, jump, or run, the patellar tendon transmits powerful forces between the quadriceps muscles and the lower leg.
When a patellar tendon rupture happens, that connection is suddenly lost. The knee loses its ability to extend properly, and movements that were automatic just moments before — such as standing, lifting the leg, or taking a step — can become nearly impossible. Even minor activities like getting in and out of a car or walking on level ground can feel unstable or painful.
Although it occurs less frequently than many other knee injuries, a patellar tendon rupture is considered a major orthopaedic emergency. The injury often requires prompt diagnosis, surgical repair of the torn tendon, and a carefully structured, progressive rehabilitation program to restore normal knee function. Without proper treatment, complications such as chronic weakness, patellar malalignment, and persistent loss of mobility can develop.
At DMPhysios, a renowned clinic based in Noida that focuses on spine and sports conditions through a patient-centred rehabilitation model, our multidisciplinary team understands how life-changing a patellar tendon rupture can be. We provide thorough assessments, evidence-based treatment plans, and personalised rehabilitation protocols designed not only to repair the tendon but also to restore strength, movement, and confidence so patients can safely return to their daily activities and sports.
Symptoms
Recognizing the symptoms early is crucial for prompt treatment. A patellar tendon rupture typically presents with the following signs:
- Sudden, severe pain at the front of the knee during activity or trauma.
- Swelling and bruising immediately after injury.
- Inability to straighten the knee or perform a straight-leg raise.
- A palpable gap or defect just below the kneecap where the tendon has torn.
- The patella may appear higher than normal (patella alta) on visual inspection or imaging.
- A feeling of instability or the knee “giving way.”
If any of these symptoms occur, immediate medical attention is necessary. Clinics like DMPhysios in Noida are equipped to evaluate and guide patients with suspected patellar tendon rupture.
Types of Patellar Tendon Rupture
While all cases involve a disruption of the patellar tendon, the injury can be classified based on severity and extent:
- Partial Patellar Tendon Rupture
- Only part of the tendon fibers tear.
- Some ability to extend the knee may remain.
- Often treated conservatively with bracing and physiotherapy.
- Complete Patellar Tendon Rupture
- The entire tendon is torn, completely detaching the patella from the tibia.
- Full loss of knee extension occurs.
- Typically requires surgical repair followed by rehabilitation.
Understanding whether a rupture is partial or complete is vital for tailoring the management plan at DMPhysios, which emphasizes patient-centered rehabilitation for optimal recovery.
Causes
A patellar tendon rupture often results from a combination of mechanical stress and underlying tendon degeneration. Common causes include:
- Sudden forceful contraction of the quadriceps while the knee is bent (e.g., landing from a jump).
- Direct trauma to the front of the knee.
- Pre-existing tendon degeneration due to chronic conditions like tendinopathy, steroid injections, or systemic diseases.
- Previous knee surgery that weakens the tendon.
At DMPhysios, clinicians assess not just the injury itself but also the contributing factors to prevent recurrence and ensure a comprehensive rehabilitation approach for patellar tendon rupture.
Risk Factors
Certain individuals are more prone to a patellar tendon rupture, especially when one or more of these risk factors are present:
- Athletic activities involving jumping or sprinting.
- Age over 40, where tendon elasticity decreases.
- Chronic knee conditions such as patellar tendinopathy (“jumper’s knee”).
- Systemic diseases like diabetes, lupus, or kidney disease that impair tendon health.
- Use of corticosteroid or fluoroquinolone medications, which can weaken tendons.
- Previous knee injury or surgery, including ACL reconstruction.
Being aware of these risk factors allows clinics like DMPhysios to develop preventive strategies and targeted rehabilitation programs tailored to each patient suffering from patellar tendon rupture.
Treatment
The treatment approach for a patellar tendon rupture depends on the severity of the injury:
Non-Surgical Treatment
- Typically reserved for partial patellar tendon ruptures.
- Involves immobilization of the knee in a brace or cast to allow healing.
- Followed by a structured physiotherapy program to restore strength and mobility.
Surgical Treatment
- Recommended for complete patellar tendon ruptures or severe partial tears.
- The torn tendon is reattached to the patella using sutures, anchors, or other fixation techniques.
- Early surgical repair improves outcomes and reduces complications like quadriceps weakness or patellar maltracking.
At DMPhysios, we collaborate closely with orthopedic surgeons and guide patients through every stage of recovery after patellar tendon rupture surgery, emphasizing patient-centered care and functional restoration.
Physiotherapy Treatment
Rehabilitation is a cornerstone of recovery following a patellar tendon rupture, whether managed conservatively or surgically. At DMPhysios in Noida, our physiotherapy programs are individualized, evidence-based, and focused on patient-centered rehabilitation to ensure optimal outcomes.
1. Acute Phase (0–6 weeks post-injury or surgery)
- Immobilization support: The knee is kept in extension with a brace or splint.
- Pain and swelling management: Ice therapy, gentle compression, and elevation.
- Quadriceps isometrics: Gentle, pain-free contractions to maintain muscle activation without straining the repair.
- Ankle pumps and hip exercises: Maintain circulation and prevent stiffness elsewhere.
2. Early Mobilization Phase (6–12 weeks)
- Gradual increase in knee flexion as allowed by the surgeon.
- Progressive weight-bearing using crutches, then transitioning to full weight-bearing.
- Closed-chain strengthening: Mini-squats, step-ups, and gentle resistance exercises within the safe range.
3. Strengthening Phase (12–20 weeks)
- Progressive quadriceps and hamstring strengthening using resistance bands or light weights.
- Proprioception and balance training: Single-leg stands, wobble board exercises.
- Stationary cycling and pool therapy to enhance mobility without overloading the knee.
4. Advanced Functional Training (20+ weeks)
- Higher-level strengthening: Lunges, leg presses, eccentric quadriceps training.
- Plyometrics and sport-specific drills for athletes, carefully monitored to avoid re-injury.
- Return-to-sport assessment: Functional tests to ensure readiness for high-demand activities.
Every phase at DMPhysios is supervised by experienced physiotherapists who adjust the intensity and progressions based on the individual’s healing status. This patient-centered approach minimizes the risk of complications like stiffness, weakness, or re-rupture after a patellar tendon rupture.
Prevention
While not all injuries can be prevented, certain strategies significantly reduce the risk of a patellar tendon rupture:
- Regular strengthening of the quadriceps and hamstrings to support the knee.
- Flexibility training for the lower limb muscles to reduce stress on the tendon.
- Gradual progression in training intensity, especially in jumping sports.
- Proper warm-up and cool-down routines before and after exercise.
- Managing underlying conditions such as diabetes or tendinopathy.
- Avoiding unnecessary corticosteroid injections into the tendon region.
Clinics like DMPhysios in Noida also offer preventive screening and exercise programs tailored to athletes and high-risk individuals to reduce the likelihood of patellar tendon rupture.
Conclusion
A patellar tendon rupture is a debilitating injury that disrupts knee function and quality of life. Early recognition, appropriate treatment, and a comprehensive rehabilitation plan are crucial for full recovery. At DMPhysios, a trusted clinic located in Noida specializing in spine and sports conditions with patient-centered rehabilitation, our team of physiotherapists and healthcare professionals provides individualized, evidence-based care to help patients regain strength, mobility, and confidence after a patellar tendon rupture.If you or someone you know is experiencing symptoms of a patellar tendon rupture, don’t delay seeking professional help. Contact DMPhysios today for an expert evaluation and a customized rehabilitation program designed to restore your knee’s function and prevent future injuries.