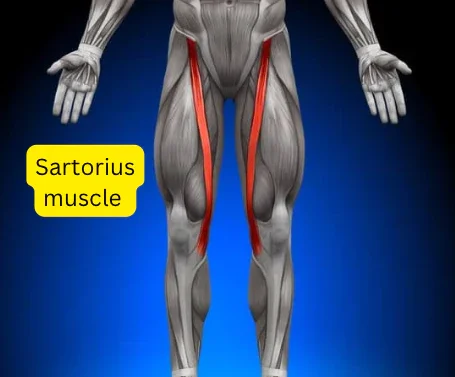
Overview
The Sartorius muscle is the longest muscle in the human body, stretching diagonally across the front of the thigh from the anterior superior iliac spine (hip bone) to the medial surface of the tibia near the knee. Its unique, ribbon-like structure gives it the ability to act across both the hip and knee joints, making it one of the most functionally versatile muscles in the lower limb. The Sartorius muscle assists in hip flexion, abduction, and external rotation, while also contributing to knee flexion. Together, these actions enable smooth, coordinated movements such as crossing one leg over the other, sitting in a tailor’s position, walking, running, or changing direction rapidly.
A Sartorius strain occurs when the muscle fibers or its tendon become overstretched, partially torn, or completely ruptured due to excessive tension or sudden, forceful movements. This can happen during activities that involve sprinting, sudden pivots, kicking, or abrupt acceleration and deceleration, which place high stress on the hip flexors and inner thigh muscles. In some cases, prolonged overuse or muscle fatigue can also lead to microscopic tears, resulting in pain and functional limitation.
Individuals suffering from a Sartorius strain often experience sharp or aching pain in the front or inner part of the thigh, tenderness near the hip or knee joint, and difficulty lifting or moving the leg freely. In moderate to severe cases, swelling, bruising, or muscle stiffness may also occur, making it challenging to perform everyday activities such as climbing stairs, running, or even walking comfortably.
At DMPhysios, a trusted physiotherapy clinic in Noida known for its expertise in spine and sports rehabilitation, Sartorius strain is treated with a personalized, evidence-based rehabilitation plan. The focus is not only on pain relief but also on restoring optimal muscle strength, flexibility, and balance. Each program is tailored to the individual’s specific condition and activity level, ensuring a safe return to daily and athletic function. The physiotherapists at DMPhysios emphasize long-term recovery through patient education, progressive exercise therapy, and movement retraining, helping patients prevent recurrence and regain full confidence in movement.
Symptoms
The symptoms of a Sartorius strain can vary depending on the severity of the injury, but commonly include:
- Sharp or dull pain along the front or inner thigh.
- Tenderness or swelling near the hip or inner knee region.
- Pain during hip flexion (lifting the thigh) or when crossing the legs.
- Muscle weakness and stiffness in the thigh.
- Discomfort when walking, running, or climbing stairs.
- A popping sensation at the time of injury in severe cases.
- Bruising or mild discoloration if small blood vessels are damaged.
Mild Sartorius strain symptoms may only cause minor discomfort, while severe strains can significantly limit daily movement and athletic performance.
Types of Sartorius Strain
While Sartorius strain is not typically divided into subtypes based on location, it can be classified by severity into three main grades:
Grade I (Mild Sartorius Strain)
- Involves small microtears in the muscle fibers.
- Minimal pain and little to no loss of strength or function.
- Commonly seen in individuals who suddenly increase activity level.
Grade II (Moderate Sartorius Strain)
- Partial tearing of the muscle fibers.
- Noticeable pain, swelling, weakness, and limited hip or knee movement.
- Pain increases with activities involving leg lifting or rotation.
Grade III (Severe Sartorius Strain)
- Complete rupture of the Sartorius muscle or tendon.
- Severe pain, significant swelling, and bruising.
- Inability to use the affected leg normally.
- May require prolonged rest or surgical evaluation in rare cases.
At DMPhysios, every patient with Sartorius strain is carefully assessed to determine the grade of injury, which guides the intensity and design of the rehabilitation program.
Causes
A Sartorius strain can develop from multiple factors that overstress the muscle. Common causes include:
- Sudden acceleration or deceleration during sports such as football, tennis, or basketball.
- Overstretching movements, especially while performing lunges, squats, or dance routines.
- Direct trauma to the front or inner thigh.
- Overuse due to repetitive hip flexion and rotation in running or cycling.
- Poor warm-up routines leading to stiff muscles before high-intensity activity.
- Muscle imbalances between the Sartorius and surrounding hip or thigh muscles.
- Weakness in the core or hip stabilizers, causing overcompensation by the Sartorius muscle.
Understanding these causes helps physiotherapists at DMPhysios design specific preventive and recovery strategies that address not just the muscle injury but also its underlying biomechanical issues.
Risk Factors
Certain individuals are at greater risk of developing a Sartorius strain, including:
- Athletes involved in sprinting, martial arts, or football.
- Dancers and gymnasts who frequently perform leg rotations or extensions.
- People with tight hip flexors or inadequate stretching routines.
- Individuals with poor posture or altered gait mechanics.
- Those with previous thigh or groin injuries.
- Middle-aged adults who suddenly return to intense activity after long breaks.
- People with weak quadriceps or adductor muscles, which force the Sartorius to work harder than usual.
Recognizing these risk factors allows early intervention and customized training programs at DMPhysios, ensuring patients remain active without recurring injury.
Treatment
The treatment for Sartorius strain depends on its severity but generally focuses on pain control, healing, and progressive restoration of muscle strength. The common management plan includes:
1. Rest and Activity Modification
- Avoid activities that aggravate pain, especially running or leg crossing.
- Use crutches in severe cases to offload pressure from the affected leg.
2. Ice Therapy
- Apply ice packs for 15–20 minutes every few hours during the first 48 hours to reduce pain and swelling.
3. Compression and Elevation
- Gentle compression using elastic bandages helps control swelling.
- Elevating the leg can assist with circulation and healing.
4. Pain Relief
- Non-steroidal anti-inflammatory drugs (NSAIDs) may be prescribed for short-term pain management.
5. Gradual Return to Activity
- Once acute pain subsides, controlled stretching and strengthening exercises begin under physiotherapist supervision.
For an optimal recovery, physiotherapy plays the central role in restoring strength, flexibility, and functional movement. That’s where the expertise of DMPhysios, Noida’s trusted sports and spine rehabilitation clinic, becomes invaluable.
Physiotherapy Treatment
At DMPhysios, physiotherapy for Sartorius strain is comprehensive, evidence-based, and tailored to each patient’s needs. The treatment progresses through several structured phases:
Phase 1: Acute Phase (Pain and Inflammation Control)
- Modalities: Ice therapy, ultrasound, or gentle electrical stimulation to reduce pain and swelling.
- Manual therapy: Soft tissue release or gentle myofascial techniques to relieve tension in surrounding muscles.
- Positioning: Avoiding positions that overstretch the Sartorius, such as excessive hip abduction or external rotation.
Phase 2: Flexibility and Range of Motion Restoration
- Gentle stretching exercises targeting the Sartorius and hip flexors once pain subsides.
- Active assisted movements to maintain hip and knee mobility.
- Foam rolling around the thigh to release muscle tightness.
Common early-stage exercises include:
- Seated knee bends
- Supine heel slides
- Gentle standing hip flexor stretches
Phase 3: Strengthening Phase
Once the range of motion improves, strengthening exercises begin to rebuild muscle endurance and balance.
Examples of exercises include:
- Straight leg raises (focusing on controlled hip flexion)
- Side-lying hip abductions
- Mini squats and step-ups
- Theraband resisted hip flexion
This phase also includes strengthening of supporting muscles, the quadriceps, gluteus medius, adductors, and core muscles to improve overall pelvic stability.
Phase 4: Neuromuscular and Functional Training
This phase focuses on retraining the muscle to work effectively during functional and sport-specific activities.
Interventions include:
- Balance and proprioception exercises (e.g., single-leg stands, wobble board).
- Coordination drills and controlled directional changes.
- Gradual progression to jogging, running, or sport-specific movements.
At DMPhysios, advanced techniques like Dry Needling, Accelerated Healing Therapy, or Manual Therapy may be integrated when appropriate to accelerate healing and tissue regeneration.
Phase 5: Return to Sports or Daily Activity
Before clearance for return to play or normal activity, patients undergo performance testing to ensure full strength and pain-free mobility. Physiotherapists at DMPhysios ensure that the patient’s movement patterns are corrected and that no compensations remain that might risk reinjury.
Prevention
Preventing a Sartorius strain involves maintaining flexibility, strength, and proper biomechanics. Here are key preventive strategies:
- Warm-up and stretch thoroughly before engaging in sports or workouts.
- Strengthen the hip flexors, adductors, and core to support balanced movement.
- Include dynamic mobility exercises for the hip and thigh in regular training.
- Avoid overtraining and allow adequate recovery between sessions.
- Maintain good posture and correct gait mechanics to reduce stress on the Sartorius muscle.
- Use proper technique in sports that involve sudden leg movements or rotations.
- Gradually increase intensity when starting new physical routines.
Regular physiotherapy check-ups at DMPhysios can help identify early signs of muscle tightness or imbalance, allowing early intervention before a Sartorius strain occurs.
Conclusion
A Sartorius strain can significantly impact daily movement, athletic performance, and overall comfort. Early diagnosis, appropriate management, and guided physiotherapy are key to complete recovery. Ignoring symptoms or returning to activity too soon can lead to chronic pain or recurring injuries.
At DMPhysios, a trusted physiotherapy clinic in Noida specializing in spine and sports conditions, the focus is on patient-centered rehabilitation that goes beyond symptom relief. The experienced team designs personalized recovery plans that target the root cause of the Sartorius strain, ensuring lasting results and full return to activity.
If you are experiencing thigh or hip pain that may indicate a Sartorius strain, don’t wait for it to worsen. Visit DMPhysios today for expert assessment, hands-on treatment, and a customized rehabilitation program designed to restore your movement, strength, and confidence.