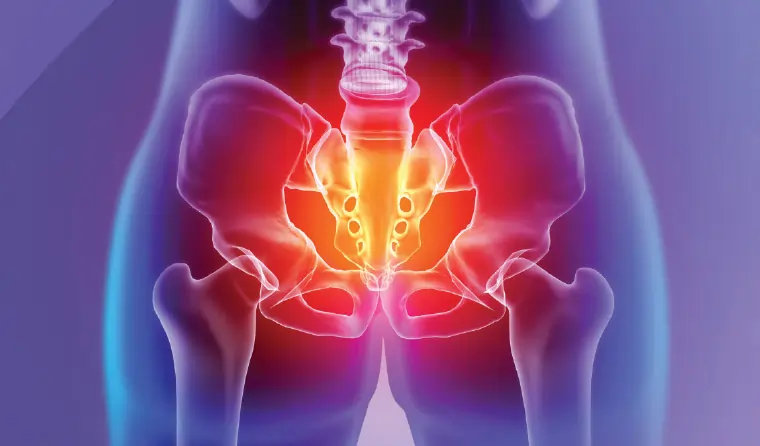
Chronic Pelvic Pain: The Overlooked Musculoskeletal Cause And How Physiotherapy Can Help?
Article Overview
- What Is Chronic Pelvic Pain?
- The Hidden Musculoskeletal Link
- Why Medications and Scans Often Don’t Solve It?
- Imaging Shows Structure, Not Function
- Medications Provide Symptom Relief, Not Correction
- The Pain-Spasm Cycle
- How Physiotherapy at DMPhysios Can Help?
- Who Should Consider Physiotherapy for Pelvic Pain?
- A Different Way to Understand Pelvic Pain
- The Emotional Impact of Chronic Pelvic Pain

C
hronic pelvic pain is one of the most frustrating and misunderstood conditions affecting both women and men. It is persistent, emotionally draining, and often resistant to conventional treatment approaches. Many individuals spend months—or even years—undergoing investigations, consulting multiple specialists, and trying different medications, yet the pain continues.
When blood tests are normal and imaging reports say “no significant findings,” patients are often left confused and helpless. Some are told it is stress-related. Others are advised to simply “manage it.” But persistent pelvic pain is never imaginary. It always has a cause.
In many cases, the missing piece of the puzzle lies not in the organs—but in the muscles, joints, fascia, and nerves surrounding the pelvis. Understanding the musculoskeletal contribution to pelvic pain can completely change how we approach treatment and recovery.
What Is Chronic Pelvic Pain?
Chronic pelvic pain (CPP) is defined as pain located in the lower abdomen or pelvic region that persists for more than six months. It may be constant or intermittent, mild or severe, sharp or dull. The discomfort can affect daily activities, sleep, work performance, and emotional well-being.
The pain may be felt in:
- Lower abdomen
- Groin region
- Perineum
- Lower back
- Hips
- Tailbone area
In women, pelvic pain may worsen during menstruation, ovulation, or intercourse. In men, it may present as deep aching in the perineal region, discomfort during sitting, or symptoms similar to prostatitis.
Chronic pelvic pain is commonly associated with conditions such as:
- Endometriosis
- Interstitial cystitis
- Chronic prostatitis
- Irritable bowel syndrome
However, a significant number of individuals with pelvic pain do not have clear pathology on imaging or laboratory tests. When no obvious cause is found, frustration increases—for both patient and practitioner.
This is where the musculoskeletal system must be considered.
The Hidden Musculoskeletal Link
The pelvis is not merely a container for organs. It is a structural and functional hub connecting the spine, hips, and lower limbs. It houses a complex network of muscles, ligaments, fascia, and nerves that work together to support movement, posture, breathing, bladder and bowel control, and sexual function.
When any part of this system becomes dysfunctional, pain can arise—even if internal organs are healthy.
1. Pelvic Floor Muscle Dysfunction
The pelvic floor is a group of muscles forming a supportive base at the bottom of the pelvis. These muscles help control urination, bowel movements, and support pelvic organs.
While weakness is commonly discussed, chronic pelvic pain is more often linked to excess tension or overactivity of the pelvic floor muscles.
When these muscles remain in a guarded or contracted state for long periods, they may develop:
- Trigger points
- Reduced blood flow
- Nerve irritation
- Referred pain patterns
Symptoms may include:
- Burning or aching pelvic pain
- Pain during intercourse
- Difficulty fully emptying bladder or bowel
- Pain while sitting
Tight muscles do not always appear abnormal on scans, making this condition easy to miss.
2. Sacroiliac Joint Dysfunction
The sacroiliac (SI) joints connect the spine to the pelvis. Even subtle stiffness or instability in these joints can produce pain that radiates to the groin, lower abdomen, buttocks, or inner thigh.
Because this pain mimics gynecological or urological conditions, it is frequently misinterpreted.
3. Myofascial Restrictions
The pelvis contains deep muscles such as the obturator internus, piriformis, adductors, and lower abdominal muscles. When these develop tight bands or trigger points, they can create persistent, poorly localized pelvic pain.
Fascial restrictions from previous surgeries, childbirth, injuries, or inflammation can also limit mobility and contribute to chronic discomfort.
4. Postural and Movement Imbalances
Prolonged sitting, poor posture, stress, abdominal surgeries, pregnancy, or previous lower back injuries can alter pelvic mechanics.
Over time, the body compensates by tightening certain muscles and overloading others. This protective strategy initially prevents injury—but when sustained, it creates chronic pain.
The key point is this: muscle dysfunction does not show up on most imaging tests, yet it can be the primary driver of pelvic pain.
Why Medications and Scans Often Don’t Solve It?
When pelvic pain persists, patients typically undergo:
- Ultrasound
- MRI
- Blood investigations
- Hormonal treatment
- Antibiotics
- Painkillers
These interventions are essential to rule out serious pathology. However, they often fail to provide long-term relief when the root cause is mechanical or muscular.
Imaging Shows Structure, Not Function
Scans are excellent at identifying structural abnormalities such as cysts, tumors, or inflammation. But they cannot assess:
- Muscle tightness
- Trigger points
- Joint micro-instability
- Movement dysfunction
- Neuromuscular coordination
A muscle in chronic spasm may appear completely normal on MRI.
Medications Provide Symptom Relief, Not Correction
Painkillers and anti-inflammatory drugs reduce discomfort temporarily. Hormonal therapy may help specific gynecological conditions. Antibiotics treat infection.
However, none of these treatments:
- Restore pelvic joint mobility
- Release overactive muscles
- Correct faulty movement patterns
- Rebalance muscle coordination
As a result, symptoms often return when medication is discontinued.
The Pain-Spasm Cycle
Chronic pelvic pain frequently becomes a self-sustaining loop:
Pain → Muscle guarding → Reduced circulation → Increased sensitivity → More pain
Unless muscle tension is directly addressed, this cycle continues indefinitely.
Nervous System Sensitization
Long-standing pain can make the nervous system hypersensitive. The brain begins to interpret normal sensations as threatening. This phenomenon, known as central sensitization, amplifies pain perception.
Physiotherapy plays an important role in calming this response through graded movement, education, and neuromuscular retraining.
How Physiotherapy at DMPhysios Can Help?
At DMPhysios, chronic pelvic pain is approached from a comprehensive musculoskeletal perspective. Rather than focusing solely on symptoms, the goal is to identify the mechanical and functional contributors.
1. Comprehensive Assessment
A detailed evaluation may include:
- Pelvic alignment analysis
- Lumbar spine mobility testing
- Hip joint examination
- Pelvic floor muscle tone assessment
- Breathing pattern evaluation
- Core muscle coordination testing
This thorough assessment helps identify the true source of dysfunction.
2. Pelvic Floor Muscle Relaxation
If muscle overactivity is present, treatment focuses on:
- Myofascial release techniques
- Trigger point therapy
- Gentle manual therapy
- Relaxation and down-training exercises
- Diaphragmatic breathing
Strengthening is introduced only after normal muscle tone is restored.
3. Joint Mobilization
Restricted sacroiliac or lumbar joints are treated with manual therapy techniques to restore normal movement. Improved joint mobility reduces abnormal stress on surrounding muscles.
4. Core and Hip Rehabilitation
Targeted exercises improve coordination between:
- Deep abdominal muscles
- Pelvic floor
- Diaphragm
- Hip stabilizers
Balanced muscle function reduces mechanical strain and prevents recurrence.
5. Nervous System Regulation
Education about pain, graded exposure to movement, and breathing techniques help calm central sensitization.
The aim is not just pain reduction—but restoration of normal function.
Who Should Consider Physiotherapy for Chronic Pelvic Pain?
You may benefit from physiotherapy if:
- Investigations are normal but pain persists
- Pain worsens with sitting or movement
- You experience pain during or after intercourse
- You feel pelvic heaviness without infection
- You have chronic lower back pain associated with pelvic discomfort
- You had childbirth or abdominal surgery
- Antibiotics have not relieved prostatitis-like symptoms
Individuals diagnosed with conditions such as Endometriosis or Chronic prostatitis may still have a musculoskeletal component contributing to their symptoms.
Physiotherapy can complement medical management and improve overall outcomes.
A Different Way to Understand Pelvic Pain
Chronic pelvic pain is often viewed as a mysterious internal issue. But what if we understood it differently?
The body is designed to protect itself. When stress, injury, inflammation, or emotional strain occurs, muscles tighten to guard vulnerable areas.
This guarding is helpful initially. But if the tension remains long after the original trigger has resolved, it becomes problematic.
The pelvis plays a central role in:
- Movement
- Posture
- Breathing
- Stability
- Organ support
Any disruption in coordination between these systems can create ongoing discomfort.
Instead of asking, “What is wrong with my organs?” a more useful question may be:
“Is my body stuck in protection mode?”
When this perspective shifts, treatment shifts as well—from suppressing symptoms to restoring balance.
The Emotional Impact of Chronic Pelvic Pain
Persistent pain affects more than physical health. It can lead to:
- Anxiety
- Sleep disturbances
- Relationship strain
- Reduced physical activity
- Fear of movement
Addressing pelvic pain through physiotherapy often improves confidence and emotional well-being, as patients regain control over their bodies.
Long-Term Benefits of Physiotherapy
With consistent care, individuals often report:
- Reduced pain intensity
- Improved sitting tolerance
- Better bladder and bowel function
- Comfortable intimacy
- Improved posture
- Increased activity levels
Most importantly, they regain trust in their body.
Final Thoughts
Chronic pelvic pain is complex—but it is not untreatable.
When medications and scans fail to provide answers, it does not mean the pain is imaginary. It may simply mean that the musculoskeletal system has been overlooked.
The pelvis is a dynamic structure requiring coordination between muscles, joints, fascia, and nerves. When this system is imbalanced, persistent pain can develop—even in the absence of visible pathology.
Physiotherapy offers a structured, evidence-based approach to identify and correct these dysfunctions. By restoring movement, normalizing muscle tone, and calming the nervous system, recovery becomes possible.
Understanding pelvic pain from a musculoskeletal perspective provides hope—and a practical path forward for those who have struggled silently for far too long.