Overview
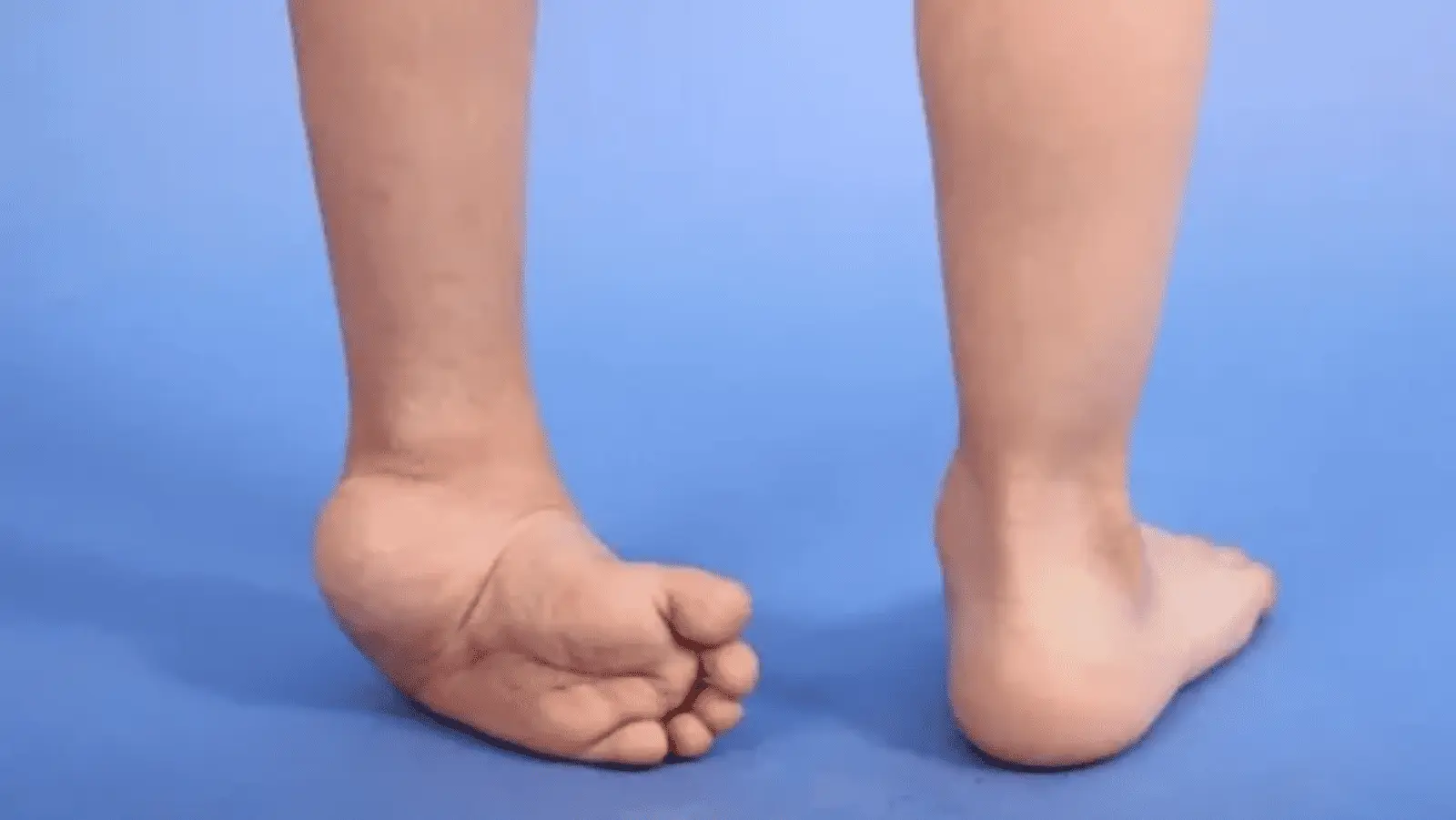
Clubfoot, medically known as Congenital Talipes Equinovarus (CTEV), is a complex and common congenital deformity that primarily affects the bones, muscles, tendons, and ligaments of the foot and ankle. It is characterized by the foot being abnormally twisted downward and inward, giving it a distinct, often rigid appearance.
This malalignment leads to an abnormal shape and position of the foot, making it difficult for the sole to rest flat on the ground. The deformity is present at birth and may vary significantly in severity from one child to another.
In most cases, clubfoot involves structural changes in both the soft tissues and bony components of the foot, including tightness in the Achilles tendon and shortened ligaments on the inner side of the ankle.
The foot may appear smaller than normal, and the calf muscle on the affected side is often underdeveloped. Because of the abnormal positioning, the foot may resemble the shape of a club, which is where the condition gets its commonly known name—clubfoot.
This condition can occur in one foot (unilateral) or both feet (bilateral), and without timely and appropriate treatment, it can lead to serious functional limitations. Children born with untreated clubfoot may develop an abnormal gait pattern, experience chronic pain, suffer from callosities due to walking on the outer side of the foot, and face lifelong mobility restrictions.
At DMPhysios, a specialized clinic based in Noida that focuses on spine and sports conditions through patient-centered rehabilitation, early identification and individualized treatment of clubfoot are foundational elements of care. We understand that the window for effective treatment is narrow and that initiating corrective strategies within the first few weeks of life can yield outstanding results.
Our dedicated pediatric physiotherapy team works closely with families to ensure that every child has the opportunity to walk independently, participate actively, and develop physically without limitations imposed by clubfoot. Through evidence-based therapy and holistic care models, DMPhysios empowers families and supports children in their journey toward a fully functional and active life.
Symptoms
The signs and symptoms of clubfoot are usually visible at birth. While it is typically painless in newborns, the deformity becomes more problematic with growth and development if untreated.
Common clinical features of clubfoot include:
- The foot (or feet) is twisted inward and downward.
- The sole faces sideways or even upward.
- Tightness or shortening of tendons and ligaments on the inner side of the foot and ankle.
- A visibly smaller or underdeveloped foot and calf muscles on the affected side.
- In severe cases, inability to place the sole of the foot flat on the ground.
Although infants do not feel pain initially, walking becomes challenging later due to improper foot positioning, leading to compensatory gait mechanics and potential long-term complications.
Types of Clubfoot
Clubfoot is broadly classified into the following types:
1. Congenital (Idiopathic) Clubfoot
This is the most common form and occurs without any known cause. It is usually an isolated deformity in an otherwise healthy infant.
2. Syndromic Clubfoot
Occurs in association with neuromuscular or genetic disorders such as arthrogryposis or spina bifida. This type tends to be more rigid and resistant to standard correction methods.
3. Positional Clubfoot
Here, the foot appears twisted due to intrauterine positioning but has normal bone and joint structures. It is more flexible and often corrects itself or requires minimal intervention.
4. Acquired Clubfoot
Though rare, acquired clubfoot may develop later due to trauma, infections, or neuromuscular disease.
At DMPhysios, accurate identification of the type of clubfoot guides the treatment approach, allowing for targeted interventions with greater chances of successful outcomes.
Causes
The exact cause of congenital clubfoot remains unclear in many cases, particularly idiopathic clubfoot. However, several factors are believed to contribute to its development:
- Genetic predisposition: A family history of clubfoot increases the likelihood.
- Neuromuscular abnormalities: Conditions affecting nerve or muscle function during fetal development.
- Abnormal fetal positioning: Reduced amniotic fluid or restricted intrauterine space may contribute to positional deformities.
- Connective tissue disorders: These may interfere with proper tendon and ligament development.
- Environmental factors: Smoking, drug use, and certain maternal infections during pregnancy may be linked to an increased risk.
Risk Factors
Several factors are known to increase the risk of a baby being born with clubfoot:
- Family history of clubfoot
- Male gender (boys are twice as likely as girls)
- Maternal smoking or substance use during pregnancy
- Low amniotic fluid during pregnancy (oligohydramnios)
- Associated congenital anomalies or syndromes
At DMPhysios, a thorough history and detailed assessment allow our physiotherapy and pediatric orthopaedic teams to identify these risks early and begin treatment at the optimal time.
Treatment
The primary goal of clubfoot treatment is to achieve a functional, pain-free, and plantigrade (flat-bottomed) foot. Most treatment begins shortly after birth and involves non-surgical and, in some cases, surgical interventions.
1. Ponseti Method (Gold Standard)
The Ponseti method is the most widely accepted and effective non-surgical treatment for idiopathic clubfoot. It includes:
- Serial casting: Gentle manipulation followed by the application of plaster casts to gradually correct the deformity. Casts are changed weekly.
- Tenotomy: A minor outpatient procedure to release the tight Achilles tendon, often necessary after the casting phase.
- Foot abduction bracing: After correction, children must wear a foot abduction brace (e.g., Dennis Browne bar) to prevent relapse.
2. French Functional Method
This physiotherapy-led method includes daily stretching, taping, and splinting, commonly used in Europe and by specialized clinics.
3. Surgical Intervention
Reserved for rigid, relapsed, or syndromic clubfoot that does not respond to conservative methods. Surgery may involve soft tissue release, tendon transfers, or bony procedures.
At DMPhysios, collaboration with orthopedic specialists ensures timely surgical referral when necessary, while our physiotherapists play a key role in pre- and post-operative rehabilitation.
Physiotherapy Treatment
Physiotherapy is crucial not only in early correction but also in long-term functional improvement and relapse prevention. At DMPhysios, we offer specialized, child-friendly, and evidence-based physiotherapy protocols for children with clubfoot.
A. Stretching and Mobilization
- Gentle passive stretches to lengthen the shortened tissues around the foot and ankle.
- Focused mobilization of the talocrural, subtalar, and midfoot joints.
- Techniques adapted based on age, severity, and flexibility.
B. Strengthening Exercises
- Strengthening of foot intrinsic muscles and ankle dorsiflexors.
- Use of functional play-based exercises to engage toddlers.
- Weight-bearing activities as tolerated.
C. Gait Training
- Once weight-bearing begins, physiotherapists assess and correct gait deviations.
- Activities include assisted walking, balance training, and proprioceptive drills.
D. Orthotic and Brace Training
- Education on the use and importance of bracing devices.
- Monitoring of brace fit, comfort, and compliance.
E. Parent Education
- Parents are educated to perform daily stretches at home.
- Regular counseling to ensure adherence to bracing schedules and follow-ups.
F. Relapse Management
- DMPhysios closely monitors children at risk of relapse, adjusting therapy intensity or orthotics use accordingly.
Our patient-centered rehabilitation model ensures that every child receives personalized care plans, involving both the child and caregivers to maximize outcomes.
Prevention
While not all cases of clubfoot can be prevented, especially idiopathic types, certain measures may help in risk reduction:
- Proper prenatal care
- Avoidance of smoking and alcohol during pregnancy
- Monitoring fetal development in high-risk pregnancies
- Early diagnosis via prenatal ultrasound (in some cases)
- Timely intervention immediately after birth
Early detection, timely referral, and structured rehabilitation—hallmarks of the care provided at DMPhysios—are the most effective strategies in minimizing the long-term impact of clubfoot.
Conclusion
Clubfoot is a treatable condition with a high success rate, especially when diagnosed early and managed appropriately through conservative or surgical means. At DMPhysios, a Noida-based clinic specializing in spine and sports conditions with a patient-centered rehabilitation philosophy, we offer integrated care for children born with clubfoot.
From expert physiotherapy treatment and parent education to long-term monitoring, our holistic approach ensures the best outcomes for every child. If your child or a loved one has been diagnosed with clubfoot, don’t wait. Early intervention is the key to a normal, pain-free, and active life.If you’re looking for expert treatment and rehabilitation for clubfoot in Noida, trust DMPhysios—where care is tailored, compassionate, and committed.
Book your consultation with DMPhysios today and take the first step toward a confident stride for your child.