Overview
Heel spur is a condition marked by persistent heel pain caused by the formation of a bony protrusion, commonly referred to as a heel spur, on the underside of the heel bone—known anatomically as the calcaneus.
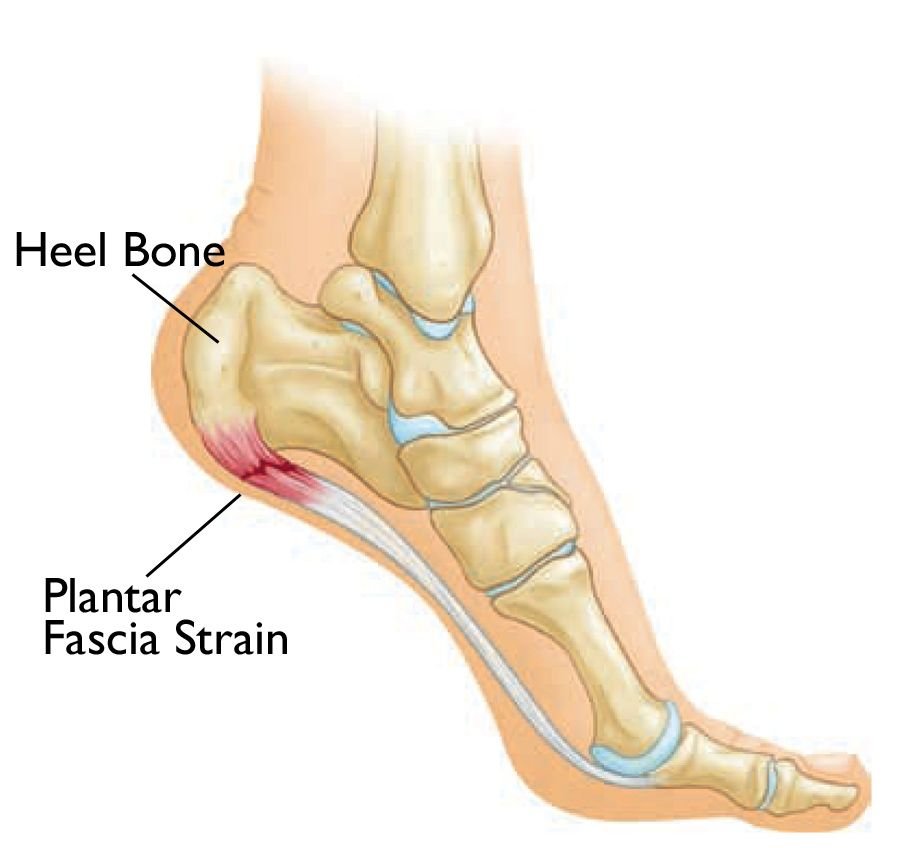
These abnormal bony growths usually develop gradually over time, most often as a response to ongoing stress and microtrauma at the site where the plantar fascia—a dense, fibrous connective tissue structure that spans the sole of the foot—attaches to the heel bone. As repetitive strain continues, the body lays down excess calcium in an attempt to stabilize the irritated area, ultimately resulting in the formation of a spur.
Interestingly, the mere presence of a heel spur does not always lead to pain or discomfort. In fact, many individuals may have a spur visible on an X-ray without experiencing any symptoms.
However, the term heel spur specifically refers to the painful syndrome that arises when this bony growth causes or contributes to irritation, inflammation, or mechanical disruption of the surrounding soft tissues. This is often driven by stress on the plantar fascia, leading to a painful inflammatory response and sometimes involving other nearby structures such as fat pads, tendons, or nerves.
People most commonly affected by heel spur include those who engage in repetitive weight-bearing activities, such as running, walking long distances, or standing for prolonged periods—especially on hard, unforgiving surfaces.
Additionally, individuals with biomechanical abnormalities, such as flat feet, high arches, or improper gait patterns, are at an increased risk. These structural irregularities alter the way forces are distributed across the foot, often placing excessive tension on the plantar fascia and, by extension, the heel bone.
At DMPhysios, a well-established physiotherapy center based in Noida and renowned for its expertise in spine and sports-related conditions, we approach heel spur with a deep understanding of both its anatomical and functional complexities.
Our patient-centered rehabilitation model focuses not only on relieving symptoms but also on correcting the underlying biomechanical faults that contribute to the condition. Whether it involves modifying gait patterns, strengthening the foot’s intrinsic musculature, or utilizing custom orthotic support, our goal is to restore optimal function, prevent recurrence, and help each patient return to pain-free living.
Symptoms
The symptoms of heel spur can vary from mild discomfort to severe pain that limits daily activities. Common signs include:
- Sharp pain in the heel when standing up in the morning (post-static dyskinesia)
- Persistent pain during walking or running
- Swelling and inflammation at the base of the heel
- Tenderness on the underside of the foot near the heel
- Warmth or a burning sensation in the heel
- Difficulty in performing weight-bearing activities
- Stiffness and reduced range of motion in the ankle or foot
In chronic cases, the discomfort from heel spur can lead to changes in gait and posture, potentially causing secondary issues in the knees, hips, or lower back.
Types of Heel Spurs
While heel spur generally refers to the pain and mechanical issues related to heel spurs, these spurs themselves can be categorized into:
- Plantar Heel Spur:
- The most common type
- Located underneath the heel bone
- Often associated with plantar fasciitis
- Posterior Heel Spur:
- Develops at the back of the heel
- Frequently associated with Achilles tendinopathy
Although not classified separately in medical literature as distinct “types” of heel spur, understanding the location of the spur is essential for targeted treatment.
Causes
Heel spur is the result of repetitive stress and strain on the foot’s soft tissues. Major contributing factors include:
- Chronic plantar fasciitis: Inflammation of the plantar fascia leads to calcium deposition at its attachment site.
- Overuse and repetitive activities: Long-distance running, jumping, and other high-impact sports.
- Poor foot biomechanics: Flat feet, high arches, or abnormal gait patterns.
- Improper footwear: Lack of arch support or cushioning.
- Age-related degeneration: As we age, the soft tissues in our feet become less flexible and more prone to injury.
- Obesity: Excess body weight increases pressure on the foot, especially the heel.
- Occupational factors: Jobs requiring prolonged standing or walking on hard surfaces.
At DMPhysios, we assess each of these potential causes individually to design a rehabilitation plan specific to the patient’s needs.
Risk Factors
Several risk factors increase the likelihood of developing heel spur:
- Age over 40
- High body mass index (BMI)
- Flat feet or overly high arches
- Prolonged standing or walking
- Poorly fitted or worn-out footwear
- Tight calf muscles and Achilles tendons
- History of foot or ankle injuries
- Previous episodes of plantar fasciitis or Achilles tendinopathy
Understanding and addressing these risk factors is central to treatment and prevention at DMPhysios, Noida’s trusted name in physiotherapy for spine and sports injuries.
Treatment
Treatment of heel spur typically begins with conservative measures and escalates only if symptoms persist.
- Rest and Activity Modification: Avoid activities that aggravate symptoms.
- Ice Therapy: Reduces inflammation and pain.
- Non-steroidal Anti-inflammatory Drugs (NSAIDs): Ibuprofen or naproxen may be prescribed.
- Orthotic Devices: Custom shoe inserts to correct biomechanical faults.
- Corticosteroid Injections: For short-term relief of intense inflammation.
- Night Splints: To stretch the plantar fascia during sleep.
- Shockwave Therapy: Stimulates healing in chronic cases.
- Surgery: Reserved for rare cases where conservative therapy fails after 9–12 months.
While these treatments can reduce pain, heel spur often recurs if the underlying biomechanical or muscular causes are not addressed—this is where physiotherapy plays a pivotal role.
Physiotherapy Treatment
At DMPhysios, we believe that individualized physiotherapy is the cornerstone for resolving heel spur. Our team of experienced physiotherapists in Noida focuses on holistic care involving:
1. Detailed Assessment and Diagnosis
- Gait analysis
- Postural assessment
- Range of motion and muscle flexibility evaluation
- Foot mechanics and arch support assessment
2. Manual Therapy
- Myofascial release for plantar fascia and calf muscles
- Joint mobilizations at the ankle and subtalar joints
- Soft tissue massage to reduce local inflammation
3. Stretching Exercises
- Plantar fascia stretch: Rolling the foot over a frozen water bottle or tennis ball
- Calf stretches: Gastrocnemius and soleus stretches against a wall
- Toe stretches and towel scrunches: To improve intrinsic foot muscle strength
4. Strengthening Protocols
- Foot intrinsic muscle strengthening: Toe curls, marble pickups
- Ankle and lower limb strengthening: Heel raises, resistance band exercises
- Core and glute strengthening: To improve overall biomechanics and reduce lower limb load
5. Taping Techniques
- Low-dye taping: To support the arch and reduce tension on the plantar fascia
6. Electrotherapy Modalities
- Accelerated Healing Therapy: To promote healing and relieve pain.
7. Custom Orthotic Recommendations
- Advice on insoles and supportive footwear to reduce heel impact
8. Gait Retraining and Postural Correction
- Biomechanical correction to prevent recurrence
- Education on proper walking and standing posture
At DMPhysios, every treatment plan for heel spur is customized based on the patient’s age, activity level, and severity of symptoms, ensuring comprehensive and long-term relief.
Prevention
Preventing heel spur is possible with consistent attention to foot health and physical activity habits. Key preventive strategies include:
- Wearing properly fitted, supportive footwear
- Maintaining a healthy weight
- Regular stretching of the calves and plantar fascia
- Avoiding overtraining or sudden increases in activity levels
- Using shock-absorbing shoe inserts if on hard surfaces
- Strengthening foot and ankle muscles regularly
- Cross-training to reduce repetitive strain
DMPhysios not only treats current symptoms but also educates patients on long-term prevention strategies to reduce recurrence and promote foot health.
Conclusion
Heel spur is a common yet often misunderstood cause of heel pain that can significantly limit your daily life, work, and physical activities. Whether you are a sportsperson, a working professional, or a senior dealing with persistent heel discomfort, early diagnosis and a targeted treatment plan are crucial.
At DMPhysios, a leading physiotherapy clinic in Noida known for its excellence in spine and sports rehabilitation, we provide evidence-based, patient-centered physiotherapy care designed to resolve heel spur from the root. Our expert physiotherapists will guide you through each stage of recovery—from pain relief to biomechanical correction and long-term prevention. If you or someone you know is suffering from heel spur, don’t ignore the signs. Pain that starts small can develop into a long-term issue if not addressed early.