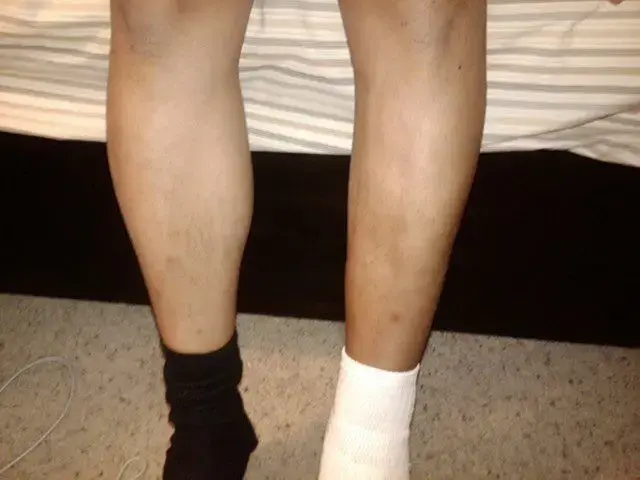
Overview
Muscle atrophy refers to a gradual wasting or loss of muscle tissue, which leads to a measurable reduction in muscle mass, strength, and overall function. Rather than being a disease in itself, it represents a visible sign of deeper underlying issues such as chronic illnesses, injuries, prolonged inactivity, or certain lifestyle patterns.
When muscles are not used regularly, or when their nerve supply is impaired, the muscle fibers begin to shrink, lose tone, and weaken. Over time this can significantly compromise mobility, reduce stamina, impair daily activities, and negatively affect posture, balance, and overall health if it is not addressed promptly.
At DMPhysios, a leading clinic in Noida renowned for its expertise in spine and sports conditions and its strong focus on patient-centered rehabilitation, muscle atrophy is regarded as a major clinical priority.
The team recognizes that this condition can affect both athletes and non-athletes alike, from people recovering from injuries or surgeries to individuals with sedentary jobs. By combining early screening, thorough assessment, and evidence-based physiotherapy interventions, DMPhysios aims to reverse or minimize the impact of muscle loss, rebuild strength and endurance, and restore patients to their optimal level of physical function and quality of life.
Symptoms
The signs of muscle atrophy are often gradual but noticeable if one pays attention. Common symptoms include:
- Visible muscle loss: Muscles appear smaller or shrunken, especially in limbs.
- Weakness: Decreased strength in the affected muscle group.
- Limited mobility: Difficulty in performing activities like climbing stairs, lifting objects, or even standing up from a chair.
- Fatigue: Muscles tire quickly during activities.
- Asymmetry: One limb may look smaller than the other due to disuse or injury.
- Joint discomfort: Secondary stiffness or pain due to weakened muscles no longer stabilizing joints effectively.
At DMPhysios, therapists assess these symptoms using advanced tools and functional testing to measure muscle strength and performance. This helps in designing a targeted plan to reverse muscle atrophy effectively.
Types of Muscle Atrophy
Although muscle atrophy broadly refers to muscle wasting, it can be classified into different types based on its cause:
- Disuse Atrophy
This occurs when muscles are not used for prolonged periods—such as during bed rest, immobilization in a cast, or sedentary lifestyle. It is reversible with exercise and rehabilitation. - Neurogenic Atrophy
Caused by injury or disease of the nerves that supply muscles (such as peripheral neuropathy, spinal cord injuries, or conditions like amyotrophic lateral sclerosis). This type progresses faster and is harder to reverse. - Cachectic Atrophy
Associated with chronic diseases like cancer, heart failure, or severe infections. It results from systemic inflammation and poor nutrition.
Understanding the type of muscle atrophy is essential for designing the correct treatment plan. At DMPhysios, clinicians conduct thorough assessments to distinguish between these types and address the root cause.
Causes
There are many reasons why muscle atrophy can occur. Common causes include:
- Immobilization or inactivity (bed rest, cast, or sedentary habits)
- Nerve injuries or compression (e.g., herniated discs, peripheral nerve entrapment)
- Aging (sarcopenia) leading to gradual loss of muscle mass and strength
- Chronic diseases like cancer, kidney failure, COPD, or heart failure
- Malnutrition or inadequate protein intake
- Hormonal imbalances such as in Cushing’s disease or hyperthyroidism
- Trauma or surgery that restricts movement
- Neuromuscular disorders (ALS, muscular dystrophy, polio history)
Because the causes of muscle atrophy are varied, proper diagnosis is critical. DMPhysios offers comprehensive evaluation protocols, including physical assessment, movement analysis, and collaboration with medical specialists when needed.
Risk Factors
Certain individuals are at greater risk for developing muscle atrophy, including:
- Older adults with decreased activity levels
- Individuals with sedentary jobs or lifestyles
- Patients recovering from fractures, ligament injuries, or joint replacements
- People with chronic illnesses (diabetes, COPD, heart disease)
- Malnourished or underweight individuals
- Those with neurological injuries or diseases
- Athletes with prolonged immobilization after injury
Recognizing these risk factors allows early intervention. DMPhysios, as a patient-centered rehabilitation clinic in Noida, emphasizes prevention and education for at-risk populations to reduce the incidence of muscle atrophy.
Treatment
The treatment of muscle atrophy depends on its underlying cause. Broadly, treatment goals focus on:
- Restoring muscle mass and strength through targeted exercises
- Addressing underlying medical conditions like nerve injuries or chronic illnesses
- Improving nutrition to support muscle recovery
- Enhancing mobility and functional independence
Medical interventions may include:
- Physical therapy and rehabilitation
- Medications for nerve pain or inflammation (if neurogenic)
- Nutritional supplements (protein, amino acids, vitamins)
- Surgery or nerve repair in selected cases
- Assistive devices to support mobility during recovery
However, the cornerstone of managing muscle atrophy remains physiotherapy and active rehabilitation—an area where DMPhysios excels.
Physiotherapy Treatment
At DMPhysios, physiotherapy is at the heart of muscle atrophy management. The clinic’s approach is patient-centered, evidence-based, and tailored to individual needs. Below is a detailed outline of physiotherapy strategies:
1. Comprehensive Assessment
Therapists at DMPhysios begin with a thorough evaluation:
- Muscle strength grading (using MMT scales)
- Range of motion testing
- Functional movement analysis
- Posture and gait assessment
- Identifying compensatory patterns
This baseline data guides the treatment plan and tracks progress.
2. Progressive Resistance Training (PRT)
One of the most effective interventions for reversing muscle atrophy is resistance training:
- Use of free weights, resistance bands, or machines
- Gradual increase in load and repetitions to stimulate hypertrophy
- Focus on both concentric and eccentric contractions
- Multi-joint functional exercises (squats, step-ups, push-pulls)
3. Neuromuscular Re-Education
For neurogenic muscle atrophy, retraining the brain-muscle connection is crucial:
- Electrical stimulation (NMES) to activate dormant muscles
- Biofeedback to improve voluntary control
- Balance and coordination drills
4. Stretching and Mobility
Tight muscles and joints can limit recovery:
- Passive and active stretching to maintain flexibility
- Joint mobilizations to improve range of motion
- PNF stretching techniques for enhanced results
5. Functional Training
At DMPhysios, emphasis is placed on functional recovery, not just isolated strength:
- Sit-to-stand training
- Gait training for lower limbs
- Reaching and lifting tasks for upper limbs
- Sport-specific drills for athletes
6. Core and Postural Stabilization
Weak core muscles can worsen muscle atrophy in limbs:
- Core strengthening (planks, dead bugs, bird dogs)
- Posture correction exercises
- Breathing exercises to enhance stability
7. Patient Education
Education is an integral part of the program at DMPhysios:
- Teaching self-exercises for home programs
- Guidance on nutrition and lifestyle changes
- Strategies to prevent reoccurrence of muscle atrophy
8. Monitoring and Progression
Regular reassessment ensures that:
- Exercises remain challenging yet safe
- Load is progressively increased
- Functional outcomes are tracked
By combining these evidence-based interventions, DMPhysios helps patients rebuild muscle mass, regain strength, and return to their normal or athletic activities faster.
Prevention
While some causes of muscle atrophy are unavoidable (such as nerve injuries), many cases can be prevented or minimized:
- Stay Active: Engage in regular physical activity including strength training and aerobic exercise.
- Balanced Nutrition: Ensure adequate protein intake, vitamins, and minerals.
- Early Mobilization: After injury or surgery, begin gentle movements as soon as medically safe.
- Avoid Prolonged Sedentary Time: Take breaks from sitting to stretch or walk.
- Monitor Chronic Conditions: Manage diseases like diabetes or COPD proactively.
- Rehabilitation Compliance: Follow prescribed physiotherapy programs to avoid reoccurrence.
DMPhysios places a strong focus on preventive strategies, offering workshops and individualized plans for people at risk of muscle atrophy—from office workers to athletes and older adults.
Conclusion
Muscle atrophy is a significant health issue that can impact independence, quality of life, and athletic performance. However, with early recognition, correct diagnosis, and a structured treatment plan, its effects can often be reversed or minimized. Physiotherapy plays a central role in recovery by restoring muscle mass, strength, and function through evidence-based exercise, neuromuscular re-education, and patient-centered care.
At DMPhysios, a premier clinic in Noida for spine and sports conditions, the team of expert physiotherapists specializes in designing customized programs to tackle muscle atrophy at its root. Whether you’re an athlete recovering from injury, an older adult aiming to maintain strength, or someone managing a chronic condition, DMPhysios provides comprehensive, patient-focused rehabilitation to help you regain control over your health.
Take the first step toward reversing muscle atrophy today—book an appointment with DMPhysios and experience tailored, expert care designed just for you.