Overview
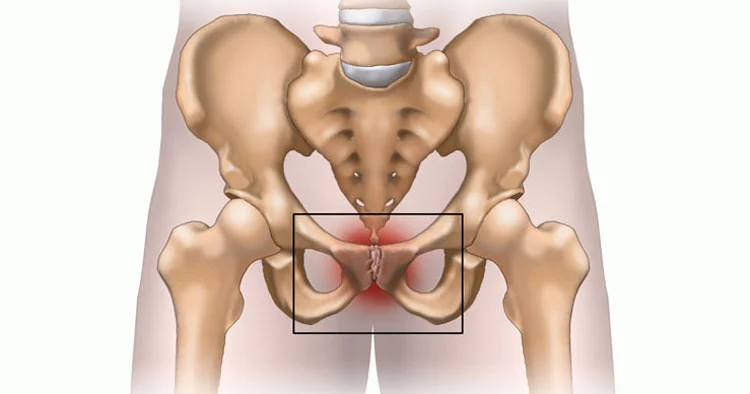
Osteitis Pubis is a painful, non-infectious inflammation of the pubic symphysis, the fibrocartilaginous joint that connects the left and right pubic bones at the front of the pelvis. This joint, although small, plays a crucial role in stabilizing the pelvis during movement.
In Osteitis Pubis, the irritation and inflammation may not only affect the joint itself but can also involve the surrounding soft tissues—including muscles, tendons, and ligaments—resulting in a cascade of discomfort and functional limitations.
This condition is most commonly observed in athletes and individuals with high levels of physical activity, particularly those engaged in sports that involve frequent twisting, sprinting, cutting, or kicking motions.
Sports such as football, rugby, hockey, athletics, and even long-distance running can impose repetitive stress on the pelvis, leading to microtrauma and inflammation over time.
The hallmark of Osteitis Pubis is chronic groin or pelvic pain that typically worsens with activity and may cause stiffness, reduced range of motion, and significant performance decline.
If left unaddressed, the condition can become debilitating, limiting not only athletic capability but also basic daily activities such as walking, climbing stairs, or rising from a seated position.
Fortunately, with early diagnosis and a comprehensive rehabilitation strategy, Osteitis Pubis is a manageable and treatable condition. A targeted approach that includes physiotherapy, movement correction, muscle rebalancing, and guided return-to-sport programs can lead to full recovery.
At DMPhysios, a leading spine and sports rehabilitation clinic based in Noida, patients receive evidence-based and patient-centered care specifically tailored to treat Osteitis Pubis.
The expert physiotherapy team at DMPhysios designs individualized programs that not only alleviate pain but also address the root causes of dysfunction, helping individuals regain full mobility and return to their active lifestyle safely and efficiently.
Symptoms of Osteitis Pubis
The hallmark symptom of Osteitis Pubis is pain in the central lower pelvis or groin region. The discomfort typically develops gradually and intensifies with physical activity. Common symptoms include:
- Deep, aching pain in the groin or lower abdomen
- Pain that worsens with activities such as running, kicking, or getting out of a car
- Tenderness over the pubic symphysis
- Pain with resisted hip adduction
- Difficulty climbing stairs or performing sit-ups
- Stiffness in the lower abdominal and inner thigh region
- Clicking or grinding sensation in the pelvis
At DMPhysios, thorough clinical evaluations help differentiate Osteitis Pubis from other groin-related conditions like adductor strains or inguinal hernias.
Types of Osteitis Pubis
Though not officially categorized into distinct subtypes, Osteitis Pubis is often functionally classified based on the underlying mechanism or cause:
1. Traumatic Osteitis Pubis
Caused by direct trauma or overuse injury, particularly in athletes. Repetitive stress leads to inflammation and microtrauma in the pubic joint.
2. Post-surgical Osteitis Pubis
Seen in patients who have undergone pelvic or urological surgeries such as prostatectomy or bladder repair. The inflammation may result from surgical manipulation around the pubic symphysis.
3. Pregnancy-related Osteitis Pubis
In some women, the pubic symphysis loosens due to hormonal changes during pregnancy, leading to inflammation and pain. Though not common, it can occur postpartum.
At DMPhysios, proper identification of the type of Osteitis Pubis plays a critical role in designing a personalized rehabilitation protocol tailored to the individual’s needs.
Causes of Osteitis Pubis
Several mechanisms can lead to the onset of Osteitis Pubis, including:
- Repetitive microtrauma from sports or manual labor
- Pelvic muscle imbalance, especially between the adductors and lower abdominal muscles
- Pelvic instability or asymmetry
- Poor biomechanics, particularly in athletes with faulty running patterns
- Direct trauma to the groin or lower abdomen
- Post-operative stress following urogenital or gynecological surgery
Identifying the underlying cause is essential for long-term recovery. DMPhysios uses a multidisciplinary approach, including musculoskeletal assessment, gait analysis, and movement screening, to trace the root cause of Osteitis Pubis in each patient.
Risk Factors
Some individuals are at a higher risk of developing Osteitis Pubis, including:
- Athletes involved in high-impact or multidirectional sports (e.g., footballers, runners)
- Women during or after pregnancy
- Post-surgical patients, especially after pelvic surgeries
- Individuals with poor core stability
- Those with muscle imbalances or previous groin injuries
- People with uneven leg lengths or altered gait mechanics
At DMPhysios, addressing these risk factors through corrective exercise, manual therapy, and posture correction plays a crucial role in preventing recurrence.
Treatment Options for Osteitis Pubis
Effective management of Osteitis Pubis involves a combination of rest, physical rehabilitation, pain management, and in some cases, medical or surgical intervention. Here’s an overview of the standard treatment protocol:
1. Rest and Activity Modification
- Complete or partial rest to avoid aggravating activities
- Temporarily ceasing sports that involve running, jumping, or kicking
2. Medications
- NSAIDs (non-steroidal anti-inflammatory drugs) like ibuprofen to reduce pain and inflammation
- Occasionally, corticosteroid injections may be administered for persistent cases
3. Ice and Heat Therapy
- Ice application in the early stages to reduce inflammation
- Heat therapy to loosen tight muscles and improve circulation during recovery
4. Shockwave Therapy or Ultrasound
- Can be used in chronic cases to enhance tissue healing and reduce fibrosis
Physiotherapy Treatment
DMPhysios, based in Noida, is highly regarded for its patient-centered rehabilitation approach in managing Osteitis Pubis. The treatment focuses on restoring muscle balance, improving core stability, reducing pain, and preventing recurrence.
Comprehensive Physiotherapy Protocol:
1. Initial Phase (Pain Management and Protection):
- Electrotherapy: Accelerated Healing Therapy to reduce pain and inflammation
- Cryotherapy: Regular icing sessions to manage acute symptoms
- Pelvic Bracing or Taping: To provide support and reduce shear stress
2. Intermediate Phase (Mobility and Strength Restoration):
- Gentle stretching of the adductors, hip flexors, and lower back
- Manual therapy for soft tissue release and joint mobilization
- Isometric core strengthening exercises (e.g., transverse abdominis activation, dead bug progression)
- Pelvic stabilization drills, including bridging and bird-dogs
- Progressive adductor loading starting from isometrics to resisted movements
3. Advanced Phase (Functional Restoration):
- Dynamic core strengthening, including planks, side planks, and Swiss ball work
- Neuromuscular retraining, emphasizing balance and proprioception
- Sport-specific drills, including cutting, sprinting, and agility training
- Return-to-play protocol, customized per the individual’s sport
4. Gait and Biomechanical Corrections:
- Detailed running and walking analysis
- Correction of leg length discrepancy, pelvic tilt, and foot mechanics
The experts at DMPhysios work closely with each patient to ensure the treatment is not only curative but also preventative. Each rehab plan is monitored and adjusted based on the patient’s progress.
Prevention of Osteitis Pubis
Preventing Osteitis Pubis involves maintaining muscular balance, optimal biomechanics, and avoiding overuse. Key preventive strategies include:
- Proper warm-up and cool-down routines
- Strengthening the core and pelvic muscles
- Avoiding training overload and incorporating rest periods
- Using proper technique in sports and exercises
- Wearing appropriate footwear to support biomechanics
- Addressing any biomechanical abnormalities, such as pelvic tilt or flat feet, with physiotherapy or orthotic support
At DMPhysios, clients undergo biomechanical screening and movement assessments even during the prevention phase, ensuring potential risk factors are mitigated before symptoms arise.
Conclusion
Osteitis Pubis may be a challenging condition, particularly for athletes and active individuals, but it is entirely manageable with the right approach. Timely diagnosis, activity modification, and a structured rehabilitation protocol are crucial to successful recovery. Left untreated, this condition can become chronic and severely affect quality of life.
DMPhysios, located in Noida, offers specialized care for patients suffering from Osteitis Pubis, ensuring comprehensive evaluation, evidence-based physiotherapy, and individualized attention. The clinic’s patient-centered rehabilitation model is designed to address not just the symptoms, but the root cause of dysfunction, ensuring a safe return to daily activities and sports.If you or someone you know is experiencing groin or pelvic pain suggestive of Osteitis Pubis, don’t delay seeking professional care. Reach out to DMPhysios, your trusted partner in spine and sports rehabilitation, and start your journey toward recovery and optimal performance.