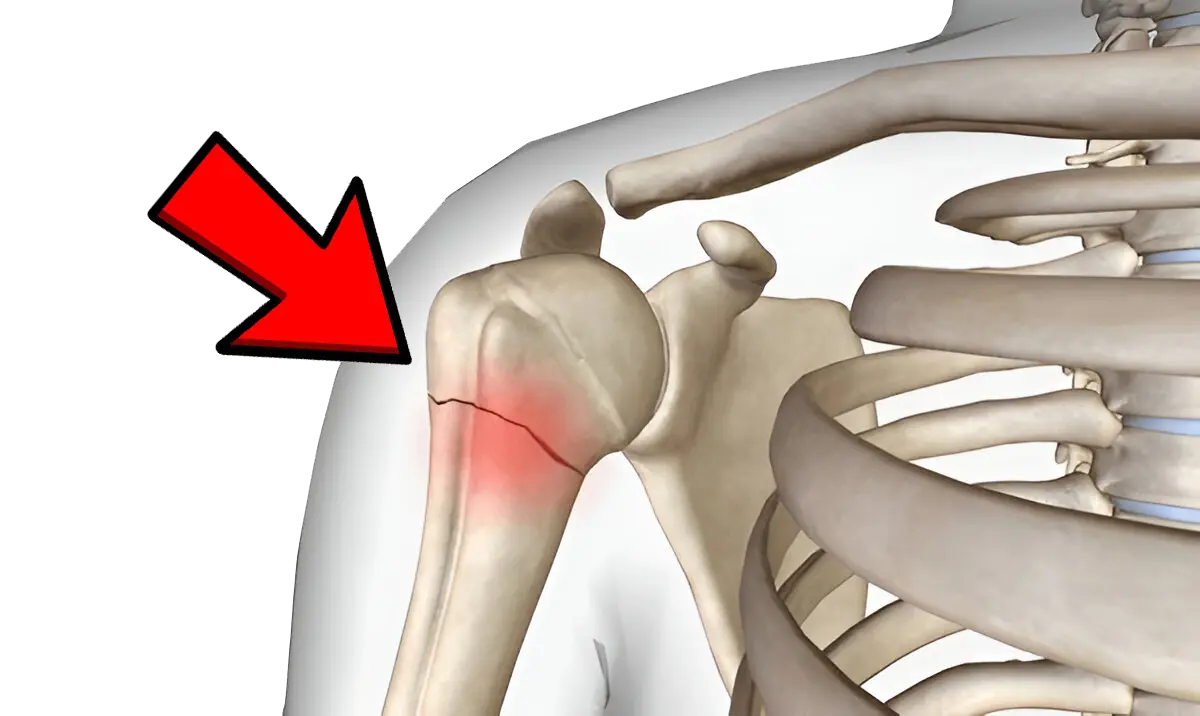
Overview
A post humerus fracture stage describes the period following the initial medical management of a humerus bone fracture, whether it was treated conservatively through casting, splinting, or bracing, or surgically through procedures such as open reduction and internal fixation with plates, screws, or intramedullary nails.
The humerus, running from the shoulder to the elbow, is the main structural support of the upper arm and forms an essential link between the shoulder girdle and the forearm. Because of its role in enabling daily arm movements like lifting, reaching, pushing, and pulling, any fracture to this bone can have a profound impact on a person’s ability to carry out routine tasks.
Once the fracture has healed radiologically, many individuals still experience ongoing issues such as stiffness of the shoulder or elbow, loss of muscular strength, lingering pain, swelling, or altered movement patterns due to disuse or compensatory habits. The phrase post humerus fracture therefore encompasses not just the healed bone but the entire recovery and rehabilitation journey after the initial union—an important phase aimed at regaining normal strength, full range of motion, proper coordination, and functional independence.
At DMPhysios, a highly regarded Noida-based clinic specializing in spine and sports conditions and known for its patient-centered rehabilitation programs, this stage is approached comprehensively. The team develops individualized rehabilitation plans that integrate hands-on therapy, guided exercises, education, and progressive strengthening. This tailored approach helps patients navigate the challenges of the post humerus fracture phase and achieve a safe, complete return to their usual activities and quality of life.
Symptoms
Although the bone may have healed radiologically, a patient in the post humerus fracture stage often presents with a combination of residual symptoms, such as:
- Persistent pain around the fracture site, especially during activity.
- Limited shoulder and/or elbow range of motion.
- Weakness of the upper arm and hand muscles.
- Swelling or mild warmth in the surrounding soft tissues.
- Difficulty performing daily activities like dressing, reaching overhead, or lifting objects.
- Numbness or tingling (if nerves were involved during the initial injury or surgery).
Recognizing these symptoms early allows clinicians, such as those at DMPhysios, to create a targeted rehabilitation program to avoid chronic dysfunction.
Types of Humerus Fractures
The kind of fracture a patient has experienced directly influences their post humerus fracture recovery plan. Common fracture types include:
- Proximal humerus fracture – near the shoulder joint. Patients often develop shoulder stiffness and altered scapulohumeral rhythm.
- Mid-shaft (diaphyseal) humerus fracture – the central portion of the bone. May involve radial nerve injury, affecting wrist and hand function post healing.
- Distal humerus fracture – near the elbow. Frequently leads to elbow stiffness and difficulty in fully extending or flexing the arm.
- Comminuted fractures – bone broken into multiple pieces; generally require longer rehabilitation and careful progression.
- Open fractures or fractures with soft tissue injury – greater risk of complications like infection and scar adhesion, leading to more intensive post-fracture therapy needs.
Understanding the initial injury type helps the rehab team at DMPhysios structure a stage-wise plan to address specific limitations in the post humerus fracture phase.
Causes
Humerus fractures can occur due to:
- Falls on an outstretched arm (common in elderly or during sports).
- Direct trauma or high-energy accidents (road traffic injuries).
- Pathological fractures due to osteoporosis or tumors.
- Sports injuries or repetitive stress in athletes.
These initial causes often shape the post humerus fracture condition. For example, an elderly patient with osteoporosis may have slower bone healing and weaker muscles, requiring a gentler yet sustained rehab approach at DMPhysios.
Risk Factors
Some patients are at higher risk for complications or prolonged recovery in the post humerus fracture stage:
- Age above 50 years.
- Osteoporosis or other bone-weakening conditions.
- Delayed or improper fracture fixation.
- Nerve injuries (especially radial nerve).
- Prolonged immobilization in a cast or brace.
- Poor compliance with prescribed exercises.
- Co-morbidities like diabetes, smoking, or vascular disease.
Identifying these risk factors early helps the rehabilitation team at DMPhysios adjust the treatment plan to minimize setbacks.
Treatment
Before entering the post humerus fracture phase, patients typically undergo either:
- Conservative treatment: immobilization in a splint, brace, or cast; indicated for non-displaced or stable fractures.
- Surgical treatment: open reduction and internal fixation (ORIF), intramedullary nailing, or external fixation for unstable or displaced fractures.
After bone union, the focus shifts from immobilization to restoring movement and strength. This is where a comprehensive post humerus fracture physiotherapy program becomes indispensable.
Physiotherapy Treatment
Rehabilitation is the cornerstone of functional recovery after a post humerus fracture. At DMPhysios, a Noida-based clinic for spine and sports conditions emphasizing patient-centered rehabilitation, the physiotherapy program is individualized. Below is a stage-wise overview:
1. Initial Phase (Week 0–2 post immobilization removal)
Goals: pain control, reduce swelling, maintain joint mobility of adjacent areas.
- Gentle pendulum exercises for the shoulder.
- Active-assisted range of motion (AAROM) for the elbow, wrist, and hand.
- Isometric contractions of deltoid, biceps, and triceps to maintain muscle tone.
- Soft tissue mobilization and gentle scar massage (if surgical incision present).
- Modalities such as ultrasound or TENS for pain relief.
2. Intermediate Phase (Weeks 3–6)
Goals: restore range of motion, begin active control.
- Gradual progression from AAROM to active range of motion (AROM) of the shoulder and elbow.
- Gentle stretching for pectorals, posterior capsule, and triceps to prevent contracture.
- Scapular stabilization exercises: scapular squeezes, wall slides.
- Progressive strengthening using light resistance bands for rotator cuff and deltoid.
- Posture correction exercises to prevent compensatory patterns.
3. Strengthening Phase (Weeks 6–12)
Goals: rebuild muscle strength, enhance functional use.
- Closed-chain exercises such as wall push-ups.
- Resistance-band exercises for all planes of shoulder motion.
- Elbow flexion/extension with light weights.
- Functional task training (reaching, lifting light objects).
- Neuromuscular re-education for coordination and proprioception.
4. Advanced / Return-to-Function Phase (Week 12 onward)
Goals: full functional restoration and return to sports/work.
- Progressive resisted exercises for rotator cuff, deltoid, biceps, and triceps.
- Plyometric drills (for athletes): medicine ball tosses, push-up progressions.
- Sport-specific or occupation-specific training.
- Advanced scapular control drills to restore normal scapulohumeral rhythm.
- Gradual reintroduction of overhead activities and weight-bearing tasks.
Throughout all these stages, patient education about activity modification, posture, and adherence to the home exercise program is emphasized at DMPhysios to ensure the best outcome in the post humerus fracture phase.
Prevention
While the fracture itself may not always be preventable, many post humerus fracture complications can be minimized by:
- Early initiation of physiotherapy under professional guidance.
- Avoiding prolonged immobilization beyond the recommended time frame.
- Maintaining good nutrition, particularly calcium and vitamin D intake.
- Following safe lifting and activity progression instructions.
- Regular follow-up visits at a specialized rehab center like DMPhysios to monitor progress and adjust exercises.
Preventive strategies reduce the risk of long-term stiffness, weakness, and pain.
Conclusion
A post humerus fracture phase can be challenging, but it is also a window of opportunity for full recovery. Properly guided rehabilitation is the key to restoring normal arm function, preventing chronic pain, and returning to work or sports. At DMPhysios, a renowned clinic in Noida specializing in spine and sports conditions with a patient-centered approach, expert physiotherapists design individualized, evidence-based programs to ensure safe and effective recovery after a humerus fracture.If you or a loved one are struggling with limitations in the post humerus fracture stage, do not wait for the symptoms to resolve on their own. Early, structured intervention makes all the difference. Contact DMPhysios today to book a consultation and begin your journey back to pain-free, confident movement.