Overview
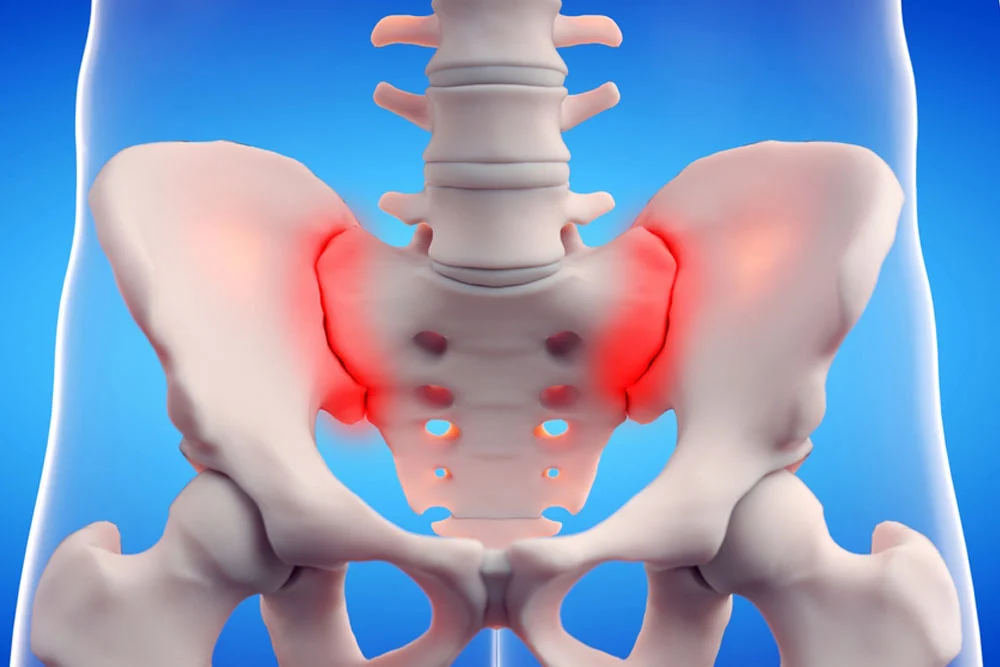
Sacroiliac Joint Dysfunction (SIJD) is a condition that arises when the sacroiliac joints—the small but powerful joints located at the base of the spine where the sacrum meets the iliac bones of the pelvis—stop functioning properly.
These joints are designed to support the weight of the upper body while transferring forces between the spine and legs. Although they allow only a small degree of motion, their stability is critical for activities like walking, standing, and bending.
When there is too much or too little movement in the sacroiliac joints, or if inflammation or degeneration occurs, the result is pain and dysfunction, often mimicking other spinal or hip disorders.
Sacroiliac Joint Dysfunction can be a hidden cause of lower back or buttock pain, making diagnosis and management challenging.
At DMPhysios, a highly respected clinic in Noida known for treating spine and sports conditions through patient-centered rehabilitation, we frequently evaluate and manage cases of Sacroiliac Joint Dysfunction.
Using a combination of clinical expertise, hands-on care, and personalized exercise-based therapy, our goal is to restore normal joint function and relieve persistent discomfort.
Symptoms of Sacroiliac Joint Dysfunction
The symptoms of Sacroiliac Joint Dysfunction can vary depending on the severity and cause but are often localized and distinct when compared to other sources of back pain. Common signs include:
- Discomfort in the lower back, buttock region, or back of the pelvis
- Sharp or stabbing pain during transitional movements, such as standing up from a chair or climbing stairs
- Pain intensifies with extended periods of standing or sitting
- Discomfort may extend to the groin, thigh, or sometimes down to the calf, resembling sciatic pain
- Uneven pain, typically experienced on one side of the lower back or pelvic area
- Feeling of instability or weakness in the pelvis or legs
Many patients report difficulty performing simple daily activities due to pain or stiffness. In some cases, Sacroiliac Joint Dysfunction may coexist with other spinal problems, further complicating the clinical picture.
Types of Sacroiliac Joint Dysfunction
Sacroiliac Joint Dysfunction can present in several mechanical patterns, depending on the nature of the restriction or hypermobility. At DMPhysios, we categorize these patterns to offer precise treatment:
1. Upslip
An upslip occurs when the ilium shifts superiorly on the sacrum. It often results from a fall onto the buttocks, lifting heavy objects incorrectly, or traumatic force through the leg.
It leads to a difference in leg length and discomfort on the involved side.
2. Downslip
A downslip is the inferior migration of the ilium, generally less common than upslip, but can occur with repetitive impact or abnormal gait patterns. Patients may feel discomfort in the groin or posterior hip region.
3. Inflare
In inflared dysfunction, the anterior part of the ilium rotates medially, narrowing the pelvic opening. This leads to anterior hip tightness and pelvic asymmetry, often noted during walking or functional movement tests.
4. Outflare
An outflare involves lateral rotation of the ilium, widening the pelvic opening and often causing altered muscle tension across the hip abductors and deep rotators. This may affect gait mechanics and cause lateral hip pain.
5. Hypermobility / Instability
In some individuals, particularly postpartum women or those with ligamentous laxity, the sacroiliac joint becomes excessively mobile. This leads to instability, muscle overcompensation, and chronic fatigue in the surrounding muscles.
6. Hypomobility / Fixation
Conversely, a fixated sacroiliac joint occurs when the joint becomes “locked” or overly restricted. This leads to stiffness and mechanical pain, particularly during rotational movements.
7. Inflammatory Sacroiliitis
In some autoimmune or rheumatologic conditions, such as ankylosing spondylitis, inflammation of the SI joint (sacroiliitis) leads to chronic pain and joint deterioration.
At DMPhysios, our team performs a detailed clinical and movement-based evaluation to determine the nature of the dysfunction, ensuring treatment is precise and effective.
Causes
A variety of factors can contribute to Sacroiliac Joint Dysfunction, and often the condition arises from a combination of structural, mechanical, and inflammatory issues. Common causes include:
- A direct impact or fall, particularly onto the buttocks or hips
- Pregnancy and childbirth, which stretch and loosen pelvic ligaments
- Leg length discrepancy, causing uneven loading of the SI joints
- Repetitive strain or overuse, especially in athletes and manual laborers
- Degenerative joint disease or arthritis of the SI joints
- Postural abnormalities or improper biomechanics during walking or lifting
- Previous spine surgery or lumbar fusion, which can increase stress on the SI joints
Identifying the cause is essential for long-term resolution. At DMPhysios, we take a comprehensive approach to assessing posture, gait, muscle strength, and movement patterns to pinpoint the underlying contributors to Sacroiliac Joint Dysfunction.
Risk Factors
Several factors increase the likelihood of developing Sacroiliac Joint Dysfunction:
- Female gender, particularly during or after pregnancy
- Hypermobile joints or connective tissue disorders
- Previous pelvic or spinal trauma
- Sedentary lifestyle, leading to muscular imbalances
- Occupations involving heavy lifting or prolonged standing
- Uneven weight distribution, such as carrying a heavy bag on one shoulder
- History of lower back pain or spinal surgery
Proactive assessment and early intervention can significantly reduce the risk of developing chronic SI joint issues. The team at DMPhysios focuses not only on treating symptoms but also on addressing these risk factors to prevent recurrence.
Treatment
The management of Sacroiliac Joint Dysfunction depends on the type and severity of symptoms. A combination of conservative care, education, and manual therapy is usually effective. Rarely, surgical options are considered.
1. Conservative Treatment
- Activity modification: Avoiding positions and movements that aggravate the joint.
- Anti-inflammatory medications: NSAIDs can help reduce pain and inflammation.
- SI joint belts or braces: These support the pelvis and reduce stress on the joint in hypermobility cases.
- Injections: Corticosteroid injections into the joint may provide temporary relief for severe cases.
2. Surgical Treatment
Surgery is rarely required but may be considered for severe, chronic Sacroiliac Joint Dysfunction that fails to respond to conservative treatment. SI joint fusion is the most common procedure, aimed at stabilizing the joint and eliminating painful motion.
However, before resorting to invasive options, conservative and rehabilitative approaches—like those offered at DMPhysios—should always be prioritized.
Physiotherapy Treatment
At DMPhysios, our philosophy revolves around restoring natural movement, stability, and strength. Physiotherapy is the cornerstone of managing Sacroiliac Joint Dysfunction, whether the cause is hypermobility, hypomobility, or inflammation.
Here’s how our evidence-based physiotherapy program is structured:
Phase 1: Pain Reduction and Stabilization
- Manual therapy: Gentle mobilizations, muscle release techniques for glutes, piriformis, and hip flexors.
- Taping or bracing: To provide external support and reduce joint irritation.
- Electrotherapy and modalities: Accelerated Healing Therapy, or cryotherapy to ease inflammation.
- Isometric core activation: Initiating engagement of the transverse abdominis and pelvic floor muscles.
Phase 2: Strengthening Core and Pelvic Stabilizers
- Glute strengthening: Bridges, clamshells, side-lying abduction to activate underused muscles.
- Hip and abdominal stability: Functional core exercises like bird-dogs, planks, and dead bugs.
- SI joint stability training: Single-leg stance, step-downs, and controlled pelvic tilts.
Phase 3: Dynamic Control and Movement Retraining
- Postural correction: Teaching neutral spine and optimal pelvic positioning.
- Functional mobility drills: Sit-to-stand, stair climbing, and gait retraining with focus on symmetry.
- Proprioceptive training: Balance boards, BOSU training, and controlled movement transitions.
Phase 4: Return to Activity or Sport
- Sport-specific drills: Tailored to athletes’ needs—pivoting, sprinting, or jumping under proper mechanics.
- Workplace ergonomics: Guidance on posture, lifting, and task modification.
- Education and self-management: Empowering patients with long-term strategies and home programs.
Each treatment plan at DMPhysios is customized based on individual presentation, goals, and progress. Our therapists closely monitor improvement and ensure that patients feel confident in their recovery journey.
Prevention of Sacroiliac Joint Dysfunction
Preventing Sacroiliac Joint Dysfunction requires proactive steps to protect the stability and function of the pelvis and lower spine. Key preventive strategies include:
- Maintaining pelvic alignment through regular mobility and strength exercises
- Strengthening the glutes, abdominals, and lower back muscles
- Using proper lifting techniques
- Avoiding prolonged positions, such as sitting cross-legged or standing unevenly
- Correcting leg length discrepancies or foot mechanics with orthotics if needed
- Postpartum pelvic rehabilitation for women after childbirth
- Staying active and avoiding muscular imbalances due to sedentary habits
At DMPhysios, we offer preventive screening and postural assessments for individuals at risk, including athletes, office workers, and new mothers. Early intervention can prevent mild dysfunction from becoming a chronic condition.
Conclusion
Sacroiliac Joint Dysfunction is a common but often misdiagnosed source of lower back and pelvic pain. Though small in size, the SI joints play a massive role in our daily movement and postural control. When they fall out of balance, the consequences can ripple through the entire spine and lower body.
Fortunately, with early recognition and a well-structured rehabilitation program, most cases of Sacroiliac Joint Dysfunction can be successfully managed without surgery. At DMPhysios, a trusted clinic in Noida specializing in spine and sports conditions, we focus on patient-centered care that goes beyond temporary pain relief. Our goal is to restore your function, prevent recurrence, and empower you to move with confidence.
If you’re experiencing lower back, buttock, or pelvic pain that just won’t go away, it might be more than a simple strain. Let our expert team at DMPhysios evaluate your condition and design a rehabilitation plan tailored just for you.
DMPhysios – Noida’s trusted name in spine and sports physiotherapy. Because you deserve movement without pain.