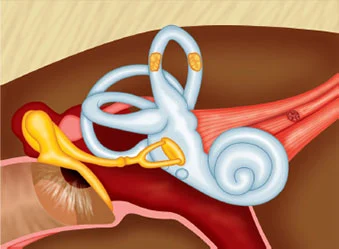
Overview
Superior Canal Dehiscence Syndrome (SCDS) is a rare but increasingly recognized vestibular disorder that affects the inner ear, specifically the superior semicircular canal. In a healthy ear, the bony covering over this canal protects and separates the inner ear from the brain cavity. However, in individuals with SCDS, this protective bony covering is either absent, thinned, or weakened, leading to an abnormal “third window” effect in the inner ear.
This defect causes sound waves and pressure changes to stimulate the inner ear inappropriately, leading to a wide range of auditory and balance-related symptoms. Since the inner ear plays a critical role in both hearing and balance, patients with Superior Canal Dehiscence Syndrome often experience debilitating vertigo, dizziness, hearing disturbances, and difficulty performing daily activities.
At DMPhysios, a leading clinic in Noida for spine and sports conditions with patient-centered rehabilitation, patients with complex vestibular disorders like Superior Canal Dehiscence Syndrome can receive comprehensive care. Through individualized rehabilitation and physiotherapy, symptoms can be better managed, improving quality of life.
Symptoms
The symptoms of Superior Canal Dehiscence Syndrome are unique and often confusing for patients, as they involve both auditory and vestibular components. Common signs include:
Auditory Symptoms
- Autophony: Hearing one’s own voice, breathing, or even eye movements unusually loud inside the head.
- Hyperacusis: Increased sensitivity to everyday sounds, often experienced as painful.
- Conductive hearing loss: A type of hearing loss where sound conduction is impaired due to the abnormal third window.
- Hearing internal body sounds: Patients often report hearing their own heartbeat, footsteps, or even digestive sounds amplified.
Vestibular Symptoms
- Vertigo induced by sound or pressure (Tullio phenomenon): Loud noises or pressure changes trigger spinning sensations.
- Oscillopsia: The sensation that the visual field is moving or bouncing with head motion.
- Dizziness and imbalance: Especially during activities involving straining, coughing, or lifting.
- Nausea and motion sickness: Due to altered vestibular signaling.
These symptoms may vary in severity and can mimic other conditions such as Ménière’s disease, vestibular migraine, or otosclerosis, making diagnosis of Superior Canal Dehiscence Syndrome challenging without specialized testing.
Types of Superior Canal Dehiscence Syndrome
Although not classified into distinct “types,” Superior Canal Dehiscence Syndrome presentations can be broadly grouped based on symptom dominance:
- Auditory-Dominant SCDS
- Patients primarily report autophony, hearing body noises, or conductive hearing loss.
- Vestibular-Dominant SCDS
- Patients primarily present with vertigo, dizziness, and imbalance triggered by sound or pressure.
- Mixed Presentation
- Most patients experience a combination of both auditory and vestibular symptoms.
This classification helps in tailoring treatment and physiotherapy approaches for individuals.
Causes
The exact cause of Superior Canal Dehiscence Syndrome is not fully understood, but several contributing factors are recognized:
- Congenital factors: Some individuals are born with thinner bone over the superior semicircular canal, which may not manifest until later in life.
- Age-related bone changes: Gradual thinning of the bone due to natural aging processes.
- Trauma or head injury: Sudden pressure or blows to the head can disrupt an already thin canal roof.
- Barotrauma: Sudden changes in intracranial or middle ear pressure (scuba diving, heavy lifting, straining, or childbirth).
- Chronic ear disease: Conditions that weaken the bony labyrinth structure.
Risk Factors
Not everyone develops Superior Canal Dehiscence Syndrome, but certain risk factors increase the likelihood:
- Family history of inner ear abnormalities.
- Occupations or hobbies involving frequent exposure to loud noises or barometric pressure changes (pilots, divers, musicians).
- Repeated head injuries (sports-related trauma).
- Aging process with natural bone thinning.
- Pre-existing ear disorders that compromise inner ear structures.
At DMPhysios, clinicians carefully assess a patient’s medical and lifestyle history to determine contributing risk factors and guide prevention strategies.
Diagnosis
The diagnosis of Superior Canal Dehiscence Syndrome usually involves:
- Detailed symptom history and physical examination.
- Audiometric testing (to detect abnormal hearing patterns).
- Vestibular-evoked myogenic potential (VEMP) testing (detects increased sensitivity in the affected canal).
- High-resolution CT scan of the temporal bone (gold standard for identifying dehiscence).
Accurate diagnosis ensures that patients receive the right treatment instead of being mismanaged for unrelated ear or vestibular conditions.
Treatment
Treatment depends on the severity of symptoms and how much daily life is impacted.
Conservative Management
- Observation: For mild symptoms, avoiding known triggers such as loud noises or straining may be sufficient.
- Lifestyle modifications: Avoiding activities that increase intracranial pressure (heavy lifting, scuba diving).
- Medication: Symptomatic relief with vestibular suppressants or anti-nausea medication.
Surgical Treatment
For severe and disabling cases, surgery may be required.
- Resurfacing: Bone graft or cement material is used to cover the dehiscent canal.
- Plugging: The canal is sealed to eliminate abnormal stimulation.
Both surgical procedures are highly specialized and typically performed by neurotologists.
Physiotherapy Treatment
While surgery addresses the structural issue, many patients continue to experience imbalance, dizziness, or reduced confidence in movement. This is where physiotherapy at DMPhysios in Noida plays a crucial role. A patient-centered rehabilitation approach focuses on regaining balance, mobility, and quality of life.
Goals of Physiotherapy
- Improve balance and reduce dizziness.
- Retrain the vestibular system through adaptation and compensation.
- Strengthen neck and core muscles for stability.
- Reduce anxiety related to movement or sound triggers.
- Restore confidence in daily and physical activities.
Physiotherapy Approaches
- Vestibular Rehabilitation Therapy (VRT)
- Customized exercises to promote central nervous system compensation for vestibular deficits.
- Gaze stabilization exercises (e.g., focusing on a target while moving the head).
- Habituation exercises to gradually reduce dizziness triggered by motion.
- Balance Training
- Static and dynamic balance activities on stable and unstable surfaces.
- Walking drills with head movements.
- Functional training for safe navigation in crowded or noisy environments.
- Strength and Conditioning
- Neck stabilization exercises to minimize strain.
- Core strengthening for postural control.
- Lower limb strengthening for stability.
- Post-surgical Rehabilitation
- Gentle mobilization exercises after surgery.
- Gradual reintroduction to normal activities.
- Monitoring for recurrence of symptoms.
- Patient Education at DMPhysios
- Counseling patients about activity modifications.
- Stress management strategies, since anxiety worsens dizziness.
- Guidance on safe return to sports or work.
With the expert physiotherapists at DMPhysios, patients with Superior Canal Dehiscence Syndrome can expect tailored rehabilitation that aligns with their personal goals and lifestyle.
Prevention
While Superior Canal Dehiscence Syndrome cannot always be prevented—especially in congenital or age-related cases—some steps can reduce risks and symptom exacerbation:
- Protect head and ears from trauma with proper safety gear.
- Avoid excessive straining during exercise or heavy lifting.
- Manage sinus or ear infections promptly to prevent chronic weakening.
- Use hearing protection in loud environments.
- Regular check-ups for individuals with family history or recurrent vestibular issues.
Early physiotherapy intervention at clinics like DMPhysios helps prevent worsening of balance impairments and reduces long-term disability.
Conclusion
Superior Canal Dehiscence Syndrome is a complex vestibular condition that significantly affects both hearing and balance. From autophony and hearing internal body sounds to vertigo triggered by sound or pressure, its impact on quality of life can be profound. While surgery may be necessary for severe cases, many patients benefit from conservative care, lifestyle adjustments, and especially vestibular physiotherapy rehabilitation.
At DMPhysios in Noida, a clinic dedicated to spine and sports conditions with patient-centered rehabilitation, patients receive individualized physiotherapy programs to manage dizziness, restore balance, and regain confidence in daily life. If you or someone you know struggles with symptoms of Superior Canal Dehiscence Syndrome, don’t delay—early evaluation and targeted rehabilitation can make a remarkable difference.
Take the first step today by reaching out to DMPhysios in Noida for expert care and patient-centered rehabilitation for Superior Canal Dehiscence Syndrome.