Overview
Trigeminal neuralgia is a chronic and often debilitating pain disorder that involves the trigeminal nerve – the major sensory nerve of the face that transmits sensations such as touch, temperature, and pain from the forehead, cheeks, jaw, and around the eyes to the brain. When this nerve becomes irritated, compressed, or damaged, it can produce episodes of sudden, intense, stabbing, or electric shock–like facial pain. These attacks can last from a few seconds to a couple of minutes and may be triggered by simple activities like speaking, eating, brushing the teeth, or even a light breeze on the face.
Recognized as one of the most severe forms of facial pain, trigeminal neuralgia can occur at any age but is more frequently seen in individuals over 50 years old, and studies show it affects women slightly more often than men. In clinical settings, the condition is sometimes referred to as tic douloureux – a name that reflects the characteristic facial grimacing or twitching that can accompany the sudden surges of pain.
While trigeminal neuralgia may arise spontaneously, it can also be secondary to other conditions such as vascular compression of the nerve, multiple sclerosis, tumors, or post-traumatic changes. Because the pain can be unpredictable and severe, early recognition and prompt intervention are crucial in reducing the impact on daily activities and preventing the transition to chronic, disabling pain.
At DMPhysios, a leading clinic in Noida renowned for its expertise in spine and sports conditions and its patient-centered approach to rehabilitation, individuals with trigeminal neuralgia are provided with comprehensive, multidisciplinary care. This may include tailored medical management, advanced physiotherapy techniques to reduce nerve irritation, education on self-care strategies, and lifestyle modifications aimed at improving long-term outcomes. By combining these approaches, DMPhysios ensures that each patient receives a holistic plan designed not only to control pain but also to restore function and quality of life.
Symptoms
The hallmark symptom of trigeminal neuralgia is intense, sudden facial pain. However, the presentation can vary between individuals. Common symptoms include:
- Sharp, shooting pain: Episodes feel like electric shocks, burning, or stabbing sensations on one side of the face.
- Brief but recurrent attacks: Pain can last from a few seconds to several minutes but may recur multiple times per day.
- Triggering by mild stimuli: Routine actions such as brushing teeth, talking, smiling, eating, or even a light breeze may provoke pain.
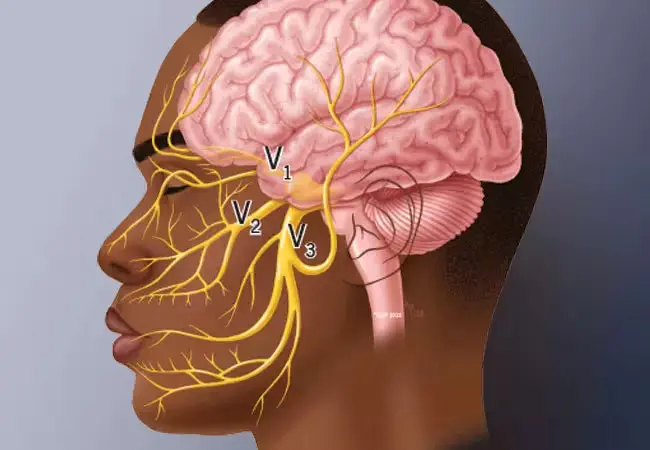
- Pain distribution: Symptoms usually follow the distribution of one or more branches of the trigeminal nerve – ophthalmic (V1), maxillary (V2), or mandibular (V3).
- Progression over time: Initially, there may be pain-free intervals, but without treatment, episodes may become more frequent and severe.
- Associated muscle spasm: Some patients may experience involuntary facial twitching due to pain intensity.
Recognizing these symptoms early and consulting professionals at DMPhysios can ensure timely intervention for trigeminal neuralgia and reduce the risk of chronic pain.
Types of Trigeminal Neuralgia
Trigeminal neuralgia can be classified into two main types based on its cause and presentation:
- Classical (Primary) Trigeminal Neuralgia:
This is the most common form, usually caused by vascular compression of the trigeminal nerve root at its entry point to the brainstem. The compression damages the nerve’s protective myelin sheath, making it hyperactive and prone to firing pain signals. - Secondary (Symptomatic) Trigeminal Neuralgia:
In this form, pain results from an underlying condition such as multiple sclerosis, tumors, or arteriovenous malformations. The symptoms may be more constant and less responsive to typical treatments.
By distinguishing between these types, healthcare professionals, including those at DMPhysios, can create individualized treatment plans tailored to the root cause of trigeminal neuralgia.
Causes
While the exact cause of trigeminal neuralgia is often idiopathic (unknown), several mechanisms have been identified:
- Neurovascular compression: The most common cause, where a blood vessel presses against the trigeminal nerve root.
- Demyelinating diseases: Conditions such as multiple sclerosis can strip the myelin sheath from the trigeminal nerve, increasing pain sensitivity.
- Tumors or cysts: Growths near the nerve can exert pressure and lead to symptoms.
- Trauma or surgery: Prior facial injury, dental procedures, or skull base surgeries may irritate the nerve.
- Structural anomalies: Certain anatomical variations may predispose individuals to nerve compression.
Understanding the underlying cause helps in selecting the most effective management approach for trigeminal neuralgia.
Risk Factors
Although anyone can develop trigeminal neuralgia, certain factors increase the risk:
- Age over 50 years
- Female sex
- Family history of neurological conditions
- Presence of multiple sclerosis
- Previous facial trauma or dental surgeries
- Hypertension or vascular abnormalities
Patients with these risk factors are encouraged to undergo early evaluation at clinics like DMPhysios in Noida, which offers specialized care for neurological and musculoskeletal conditions.
Treatment
Treatment of trigeminal neuralgia focuses on controlling pain, addressing the underlying cause, and improving quality of life. The following options are commonly used:
1. Medications
- Anticonvulsants (Carbamazepine, Oxcarbazepine): These are the first-line drugs to calm overactive nerve firing.
- Muscle relaxants (Baclofen): May be used in combination with anticonvulsants.
- Tricyclic antidepressants: For managing associated chronic pain.
- Topical agents: Lidocaine or capsaicin creams may help in mild cases.
2. Interventional Procedures
When medications are ineffective or poorly tolerated, procedures may be recommended:
- Microvascular decompression (MVD): Surgery to relieve vascular pressure on the nerve.
- Radiofrequency ablation: Targeted destruction of nerve fibers to block pain signals.
- Gamma knife radiosurgery: Non-invasive focused radiation to damage the pain fibers.
- Balloon compression: Temporarily compresses the nerve to disrupt pain transmission.
3. Multidisciplinary Approach
Combining medical treatment with physical therapy, counseling, and lifestyle changes yields the best outcomes. DMPhysios emphasizes this patient-centered model for treating trigeminal neuralgia.
Physiotherapy Treatment
Physiotherapy plays an important supportive role in managing trigeminal neuralgia, especially in reducing muscle tension, improving circulation, and teaching pain-control strategies. At DMPhysios, physiotherapists tailor programs to each patient’s needs.
Key components of physiotherapy management include:
1. Patient Education and Counseling
- Explaining the condition and its triggers empowers patients to avoid exacerbating factors.
- Guidance on ergonomics, posture, and relaxation techniques reduces secondary tension in the neck and facial muscles.
2. Gentle Soft Tissue and Myofascial Release
- Targeting the temporalis, masseter, and neck muscles can help alleviate secondary muscle spasm and tension headaches often associated with trigeminal neuralgia.
- Manual therapy should be gentle to avoid triggering pain.
3. Neuromuscular Re-education
- Teaching controlled jaw and facial muscle movements to minimize overuse or irritation of the trigeminal nerve.
- Exercises to improve coordination between neck, jaw, and facial muscles.
4. Modalities for Pain Relief
- Transcutaneous Electrical Nerve Stimulation (TENS): Applied to cervical or facial trigger zones to modulate pain.
- Low-Level Laser Therapy (LLLT): Can reduce inflammation and enhance nerve healing.
- Moist Heat Therapy: Gentle application around the neck and shoulder region may improve circulation and relaxation.
5. Breathing and Relaxation Training
Stress can exacerbate trigeminal neuralgia episodes. Guided breathing, progressive muscle relaxation, and mindfulness exercises taught at DMPhysios help reduce nervous system hyperactivity.
6. Posture Correction and Cervical Care
Since cervical posture can influence cranial nerve dynamics, strengthening deep neck flexors and correcting alignment may reduce the frequency of pain episodes.
7. Home Exercise Program
Patients are taught simple jaw mobility, neck stretches, and relaxation techniques to practice at home. Consistency is key for long-term results.
By combining these interventions, DMPhysios ensures that physiotherapy for trigeminal neuralgia not only targets symptoms but also enhances overall quality of life.
Prevention
While it may not always be possible to prevent trigeminal neuralgia, adopting certain habits can reduce the risk of triggering or worsening the condition:
- Maintain good posture to prevent cervical and cranial nerve strain.
- Manage stress effectively through relaxation, meditation, or yoga.
- Avoid known triggers such as extreme cold wind, excessive chewing on one side, or abrupt facial movements.
- Regular check-ups if you have risk factors like multiple sclerosis or vascular abnormalities.
- Follow home exercise and ergonomic advice provided by your physiotherapist at DMPhysios.
These preventive strategies can help minimize the frequency and severity of attacks in individuals prone to trigeminal neuralgia.
Conclusion
Trigeminal neuralgia is a debilitating condition that significantly impacts daily life. However, with timely diagnosis, appropriate medical management, and a supportive physiotherapy program, most patients can achieve meaningful pain relief and improved function.
At DMPhysios, a leading clinic in Noida for spine and sports conditions offering patient-centered rehabilitation, the focus is on a holistic approach to trigeminal neuralgia. By integrating medical care with advanced physiotherapy techniques and lifestyle counseling, patients receive comprehensive support for long-term recovery.If you or someone you know is struggling with facial pain suggestive of trigeminal neuralgia, don’t wait for the condition to worsen. Contact DMPhysios today for a thorough assessment and a personalized treatment plan. With expert care, it is possible to reclaim a pain-free and active life.