Overview
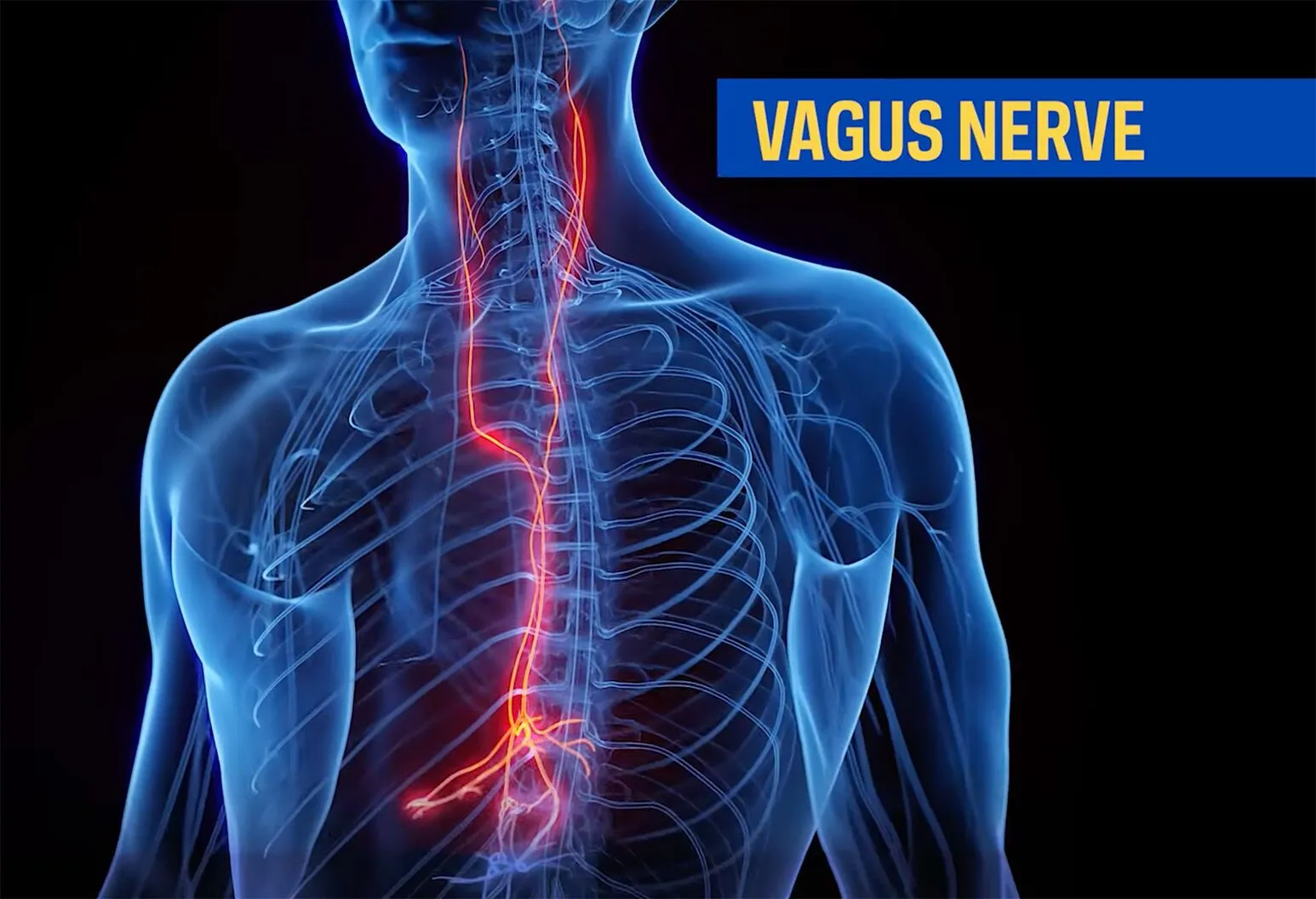
The vagus nerve, also referred to as the tenth cranial nerve, is one of the most vital nerves in the human body. It is a major component of the parasympathetic nervous system and is responsible for controlling a wide range of automatic bodily functions. These include regulating the heart rate, supporting proper digestion, managing respiratory rate, and conveying sensory information from the internal organs to the brain. When this intricate nerve is compromised, a condition known as a vagus nerve injury arises, which can disrupt these essential physiological processes and lead to a variety of symptoms.
A vagus nerve injury can occur due to numerous factors such as traumatic injuries, complications during surgical procedures, viral or bacterial infections, or long-standing medical conditions like diabetes and hypertension. While such injuries may not be very common, their impact can be profound, affecting not only basic bodily functions but also overall quality of life. Individuals with a vagus nerve injury may experience difficulties with swallowing, voice changes, digestive disturbances, irregular heart rhythms, and even breathing irregularities.
Early recognition of the condition and timely intervention are key to preventing long-term complications. This is where specialized rehabilitation becomes critical. At DMPhysios, a premier clinic in Noida specializing in spine and sports-related conditions, patient-centered rehabilitation is emphasized. Through personalized assessment and targeted therapy, the clinic helps restore optimal function, improve quality of life, and support patients in their journey to recover fully from a vagus nerve injury.
Symptoms
The symptoms of a vagus nerve injury can vary depending on the extent and location of the damage. Common signs include:
- Hoarseness or voice changes – The vagus nerve controls the muscles of the larynx, so injury can lead to vocal cord weakness or paralysis.
- Difficulty swallowing (dysphagia) – Damage can affect the throat and esophagus, making swallowing painful or challenging.
- Loss of gag reflex – A diminished gag reflex is often an indicator of vagus nerve involvement.
- Digestive problems – Such as gastroparesis, nausea, or bloating, due to impaired parasympathetic control.
- Abnormal heart rate – The vagus nerve modulates heart rhythm, and injury may cause tachycardia or bradycardia.
- Respiratory difficulties – Breathing irregularities or shortness of breath may occur.
- Fainting or dizziness – Due to abnormal autonomic regulation.
Patients with a vagus nerve injury may experience one or several of these symptoms, depending on whether the injury is partial or complete.
Types of Vagus Nerve Injury
While vagus nerve injury is not always classified into rigid subtypes, clinicians often recognize two broad categories:
- Unilateral vs. Bilateral Injury
- Unilateral: Only one side of the vagus nerve is affected, leading to mild to moderate symptoms like hoarseness or swallowing difficulties.
- Bilateral: Both sides are involved, which can result in severe voice changes, breathing difficulties, and more significant autonomic dysfunction.
- Traumatic vs. Non-Traumatic Injury
- Traumatic: Caused by physical injury, such as neck trauma, surgical procedures, or stab wounds.
- Non-Traumatic: Results from conditions like infections, tumors, inflammation, or degenerative diseases.
At DMPhysios, understanding the type of vagus nerve injury helps in designing precise physiotherapy and rehabilitation strategies.
Causes
Several factors can cause a vagus nerve injury. Common causes include:
- Surgical complications – Surgeries on the neck, thyroid, esophagus, or heart may inadvertently damage the vagus nerve.
- Trauma – Car accidents, falls, or penetrating injuries to the neck can directly injure the nerve.
- Infections – Viral infections such as herpes or bacterial infections can inflame the nerve.
- Tumors or growths – Tumors in the neck, chest, or brain may compress the vagus nerve.
- Neurological disorders – Conditions such as multiple sclerosis can cause demyelination of the nerve.
- Chronic medical conditions – Diabetes and other metabolic disorders may indirectly damage the nerve over time.
Understanding the cause is crucial for treatment. Early diagnosis at clinics like DMPhysios can prevent further complications.
Risk Factors
Certain factors increase the likelihood of developing a vagus nerve injury:
- History of neck, throat, or chest surgery
- Traumatic injuries involving the cervical region
- Chronic medical conditions like diabetes or hypertension
- Neurological disorders
- Tumors or growths near the vagus nerve
- Viral or bacterial infections affecting cranial nerves
Identifying these risk factors can help patients take preventive measures and seek timely physiotherapy intervention.
Treatment
Treatment for a vagus nerve injury depends on the severity and underlying cause. It may include:
- Medical Management
- Medications for digestive issues (prokinetics)
- Anti-inflammatory drugs or antivirals if infection is present
- Beta-blockers or other heart medications to manage abnormal heart rate
- Surgical Intervention
- Required if the nerve is compressed by a tumor or severely damaged during trauma or surgery.
- Microsurgery may help repair nerve damage in select cases.
- Lifestyle and Supportive Measures
- Dietary modifications for easier digestion
- Voice therapy for patients with hoarseness
- Breathing exercises for respiratory difficulties
While medical and surgical treatments address the root cause, physiotherapy plays a critical role in restoring function and improving quality of life.
Physiotherapy Treatment
Physiotherapy is essential for rehabilitation following a vagus nerve injury. At DMPhysios, treatment is patient-centered, targeting symptoms like swallowing difficulties, voice problems, and autonomic dysfunction.
1. Breathing and Respiratory Exercises
The vagus nerve contributes to parasympathetic control of breathing. Physiotherapists may use:
- Diaphragmatic breathing exercises
- Incentive spirometry to improve lung expansion
- Pursed-lip breathing for better oxygenation
2. Swallowing and Dysphagia Therapy
For patients with difficulty swallowing:
- Gentle oral motor exercises
- Shaping exercises for the tongue and lips
- Postural techniques to aid safe swallowing
- Use of neuromuscular electrical stimulation (NMES) to improve pharyngeal muscle function
3. Voice Rehabilitation
Patients with hoarseness benefit from:
- Vocal cord strengthening exercises
- Resonant voice therapy
- Breath control techniques
- Coordination of voice and breathing to reduce strain
4. Autonomic Function Support
Since the vagus nerve affects heart rate and digestion:
- Guided relaxation and meditation to stimulate parasympathetic activity
- Gentle yoga or tai chi for heart rate variability improvement
- Biofeedback techniques to monitor and improve autonomic regulation
5. Postural and Neck Exercises
If the injury results from trauma or surgery:
- Cervical mobility exercises
- Neck and shoulder strengthening
- Postural correction to reduce nerve compression
6. Nutritional and Lifestyle Counseling
Physiotherapists at DMPhysios also educate patients on:
- Anti-inflammatory diets
- Proper hydration and small, frequent meals to reduce digestive strain
- Avoiding activities that exacerbate symptoms
Rehabilitation at DMPhysios is holistic, combining physical therapy, lifestyle modifications, and patient education to maximize recovery from a vagus nerve injury.
Prevention
While not all vagus nerve injuries are preventable, certain measures can reduce the risk:
- Avoid high-risk activities that may lead to neck or chest trauma
- Ensure proper surgical techniques and follow post-operative care instructions
- Manage chronic conditions like diabetes and hypertension effectively
- Treat infections promptly to prevent nerve involvement
- Seek early physiotherapy intervention if symptoms like hoarseness, swallowing difficulties, or irregular heart rate appear
Prevention is always better than cure, and early engagement with clinics like DMPhysios ensures better outcomes.
Conclusion
A vagus nerve injury can have widespread effects on voice, swallowing, heart rate, digestion, and overall well-being. Early recognition of symptoms, accurate diagnosis, and a comprehensive treatment plan are essential for recovery. Physiotherapy, especially patient-centered rehabilitation as offered at DMPhysios in Noida, plays a vital role in restoring function and improving quality of life.
If you or a loved one are experiencing symptoms suggestive of a vagus nerve injury, it is crucial to seek professional help immediately. DMPhysios combines expert medical guidance with personalized physiotherapy programs to ensure effective recovery from nerve injuries and related complications. Don’t wait, take the first step towards improved health and function today.