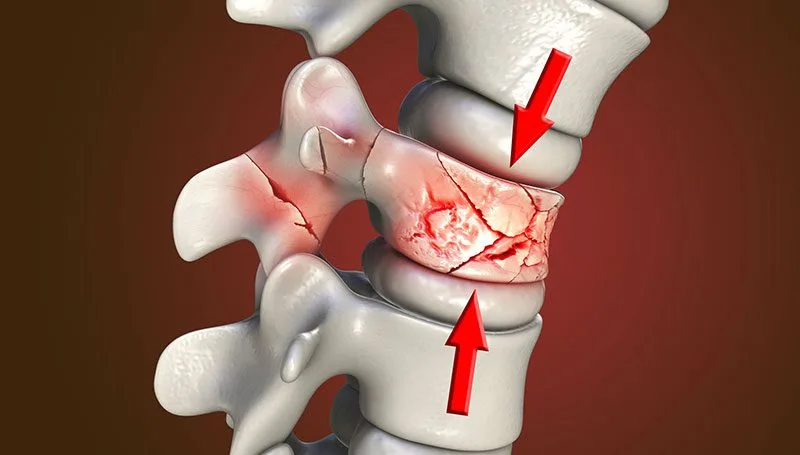
Overview
A vertebral compression fracture (VCF) refers to a condition in which one of the vertebral bodies within the spine collapses or becomes compressed, leading to a reduction in its normal height. This structural compromise typically occurs in the thoracic (mid-back) or lumbar (lower back) regions of the spine, which are responsible for bearing much of the body’s weight and enabling functional movement.
Vertebral compression fractures are most commonly associated with osteoporosis, a condition characterized by weakened and brittle bones, making them more susceptible to fractures even with minimal stress or trauma. However, VCFs may also result from acute trauma, such as a fall or accident, or from pathological causes like the spread of cancer (metastasis) to the bone.
When a vertebral body collapses, it can cause sharp or persistent back pain, limited spinal mobility, spinal deformities such as kyphosis (a forward rounding of the back), and in more advanced cases, pressure on the spinal cord or nerve roots may lead to neurological symptoms. These issues can greatly disrupt everyday functioning and negatively impact overall quality of life.
At DMPhysios, a leading physiotherapy and rehabilitation clinic in Noida with a special focus on spine and sports-related conditions, we understand how disruptive a vertebral compression fracture can be to one’s quality of life. Our team of experienced physiotherapists and spine specialists adopts a patient-centered approach, tailoring each rehabilitation plan to the individual’s needs, condition severity, and recovery goals. Through targeted physiotherapy, postural training, core stabilization, and spine care education, we help patients manage pain, regain mobility, and restore spinal integrity—promoting long-term recovery and reducing the risk of future fractures.
Symptoms of Vertebral Compression Fracture
The symptoms of a vertebral compression fracture may vary depending on the severity and underlying cause, but common signs include:
- Sudden onset of back pain, often sharp and localized
- Pain that intensifies during standing, walking, or physical activity
- Decreased height over time
- A stooped posture or kyphotic deformity (hunched back)
- Limited spinal mobility
- Muscle spasms around the fracture site
- In severe cases: numbness, tingling, or weakness due to spinal cord involvement
Some individuals may not initially feel pain, especially if the fracture is due to osteoporosis and develops gradually.
Types of Vertebral Compression Fractures
Vertebral compression fractures (VCFs) are not uniform in nature—they can vary significantly based on how the vertebral body collapses and the forces involved in the injury. Understanding the different types of VCFs is essential for determining the appropriate treatment strategy and predicting potential complications. These fractures are generally categorized into three main types:
1. Wedge Fracture
This is the most commonly observed form of vertebral compression fracture, particularly among individuals with osteoporosis. In a wedge fracture, the anterior (front) portion of the vertebral body collapses more than the posterior, creating a wedge-shaped deformity. This structural change can lead to:
- Loss of spinal height
- Postural alterations, such as a stooped back or kyphosis
- Chronic back pain due to altered biomechanics
Since wedge fractures often occur silently in osteoporotic patients, early detection and management are crucial to preventing further vertebral damage.
2. Crush Fracture
In a crush fracture, there is uniform collapse of the entire vertebral body, meaning both the front and back of the vertebra compress simultaneously. This type of fracture is more commonly associated with:
- High-impact trauma, such as falls or accidents
- Pathological bone conditions, including metastatic cancer that weakens the vertebrae from within
Crush fractures may lead to significant spinal instability and often present with more severe pain and functional limitations than wedge fractures.
3. Burst Fracture
A burst fracture represents the most serious form of vertebral compression fracture. It occurs when the vertebra literally shatters into multiple fragments, usually as a result of high-energy trauma like a car crash or a significant fall from height. Unlike wedge or crush fractures, a burst fracture:
- Involves fragments that can spread in multiple directions
- May encroach upon the spinal canal, increasing the risk of spinal cord injury
- Often presents with neurological symptoms, such as numbness, tingling, or even paralysis
Because of the potential for serious neurological complications, burst fractures usually require urgent medical and often surgical intervention, along with intensive rehabilitation.
Understanding the type of vertebral compression fracture is essential for planning a suitable treatment and rehabilitation approach at DMPhysios.
Causes of Vertebral Compression Fracture
Several underlying conditions and events can lead to vertebral compression fractures, including:
- Osteoporosis: The primary cause, as it weakens bones, making them fragile and susceptible to collapse.
- Trauma: Falls, car accidents, or heavy lifting injuries.
- Cancer: Metastatic tumors compromise bone strength, increasing the risk of fractures.
- Long-term corticosteroid use: Weakens bone structure.
- Spinal infections: Rare but can erode the bone.
- Bone diseases: Such as multiple myeloma or Paget’s disease.
At DMPhysios, we conduct a thorough assessment to determine the exact cause before initiating a personalized rehabilitation plan.
Risk Factors
Various factors increase the likelihood of developing a vertebral compression fracture, including:
- Advanced age, especially postmenopausal women
- Low bone mineral density (osteopenia/osteoporosis)
- History of previous fractures
- Smoking and alcohol use
- Chronic use of medications like steroids
- Nutritional deficiencies (especially Vitamin D and calcium)
- Sedentary lifestyle
Early detection of these risk factors is crucial. At DMPhysios, our prevention-oriented care helps patients manage and reduce these risks effectively.
Medical Treatment Options
Treatment for a vertebral compression fracture depends on the severity, cause, and symptoms. Medical management may include:
- Pain Management
- NSAIDs or acetaminophen
- Muscle relaxants for spasms
- Opioids (short-term) for severe pain
- Bracing
- Thoracolumbar sacral orthosis (TLSO) braces may be used to immobilize and support the spine during healing.
- Vertebroplasty or Kyphoplasty
- Minimally invasive procedures where bone cement is injected to stabilize the fracture.
- Often used in osteoporotic or cancer-related fractures.
- Surgical Intervention
- Reserved for severe cases like burst fractures with spinal instability or neurological compromise.
However, surgery and medications are not the only answers. At DMPhysios, we believe in a holistic and conservative care model that heavily integrates physiotherapy.
Physiotherapy Treatment
Physiotherapy is the cornerstone of non-surgical management for a vertebral compression fracture, especially in stable or healing stages. At DMPhysios, we develop a customized rehabilitation plan that focuses on pain relief, posture correction, spinal strengthening, and functional independence.
Here’s how we approach physiotherapy for vertebral compression fractures:
1. Acute Phase (First 1–3 Weeks)
Goals: Pain control, protection, and preventing further injury.
- Rest and Activity Modification
- Avoid movements that aggravate pain (e.g., forward bending, lifting).
- Modalities
- Ice or heat therapy for pain and inflammation.
- Electrotherapy (TENS or IFT) for pain modulation.
- Positioning Advice
- Sleep with a pillow under knees (supine) or between knees (side-lying) to reduce spinal load.
2. Subacute Phase (3–6 Weeks)
Goals: Restore mobility and start muscle activation.
- Gentle Range of Motion Exercises
- For shoulders, hips, and neck to prevent stiffness.
- Core Stabilization Exercises
- Pelvic tilts, deep abdominal contractions.
- Postural Correction
- Awareness training using mirrors or verbal cues.
- Breathing Exercises
- Diaphragmatic breathing to maintain chest mobility and reduce tension.
3. Strengthening and Functional Phase (6+ Weeks)
Goals: Build strength, endurance, and return to function.
- Back Extensor Strengthening
- Prone arm and leg raises, bird-dog, and Swiss ball extensions.
- Core and Pelvic Muscle Activation
- Planks (modified), glute bridges.
- Gait Training
- Focused work on posture, heel-to-toe walking, and balance.
- Proprioceptive and Balance Exercises
- Use of balance boards, foam surfaces.
- Functional Training
- Sit-to-stand, stair climbing, reaching, and lifting mechanics.
Every treatment plan at DMPhysios is supervised and adapted weekly depending on patient progress and goals. We also incorporate ergonomic counseling, home exercise programs, and osteoporosis education to support long-term spine health.
Prevention of Vertebral Compression Fractures
Prevention is always better than cure, especially when it comes to vertebral compression fractures. Here are key strategies we recommend at DMPhysios:
- Bone Health Maintenance
- Ensure adequate calcium and vitamin D intake.
- Regular DEXA scans after age 50 to assess bone density.
- Fall Prevention
- Home safety assessment (remove rugs, install grab bars).
- Balance and agility training for the elderly.
- Regular Weight-Bearing Exercise
- Walking, low-impact aerobics, resistance training under supervision.
- Avoid Smoking and Excessive Alcohol
- Both reduce bone strength.
- Correct Posture and Lifting Techniques
- Training in spinal-safe movement habits during daily activities.
DMPhysios offers preventive programs and workshops in Noida to help educate individuals at risk of developing vertebral compression fractures.
Conclusion
A vertebral compression fracture can be a debilitating condition if not diagnosed and managed appropriately. While osteoporosis remains the leading cause, trauma and underlying diseases must not be overlooked. Early intervention, combined with a structured physiotherapy regimen, plays a pivotal role in pain management, functional recovery, and preventing further fractures.
At DMPhysios, Noida’s trusted physiotherapy clinic for spine and sports conditions, we emphasize patient-centered rehabilitation. Our expert team of physiotherapists provides comprehensive care, from acute pain management to long-term functional recovery. Whether you’re recovering from a fracture or aiming to prevent one, DMPhysios is here to help you move better and live pain-free.If you or a loved one is suffering from a vertebral compression fracture, don’t delay treatment. Reach out to DMPhysios in Noida today for a personalized assessment and recovery plan. Our experienced spine care specialists are ready to guide you through every step of your healing journey.
Contact us now to book your consultation and take the first step toward a pain-free life.