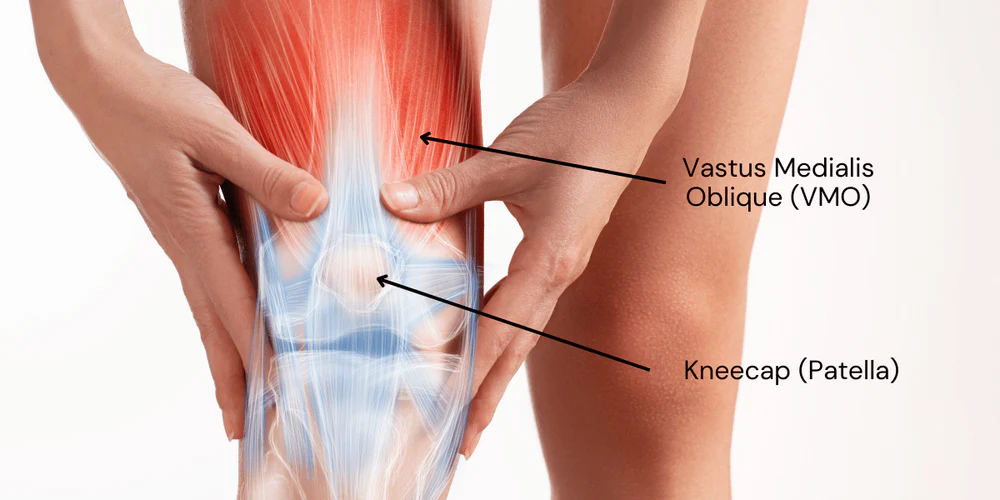
Why Body Pain Feels Worse in Winter and What Physiotherapy Can Do

M
ost people wait for winter with excitement. Cozy blankets. Warm drinks. Soft sweaters. But if you’re someone who struggles with joint pain, back pain, arthritis, muscle tension, or old injuries, winter may feel like the season your body starts complaining louder than ever.
Suddenly:
- Knees ache when climbing stairs
- The back feels stiff in the morning
- Shoulder and neck tightness increases
- Old injuries “wake up” again
- Even small aches feel exaggerated
Patients often ask:
“Why does everything hurt more in winter, and is it just in my head?”
The good news:
No, it’s not in your head. There are very real biological, environmental, and lifestyle factors behind winter pain.
And even better news:
Physiotherapy has powerful, science-backed strategies to reduce winter pain, keep joints mobile, and help you stay active without discomfort.
Let’s dive deeper.
Why Does Pain Feel Worse in Winter?
Winter changes how the body works, from blood flow to hormone balance to how stiff tissues become. Several mechanisms often happen at once.
1. Cold Weather Tightens Muscles and Soft Tissues
Muscles, tendons, and ligaments behave differently depending on temperature.
Cold temperatures cause:
- Decreased elasticity
- Slower contraction and relaxation
- Reduced blood flow
- Increased muscle guarding (protective tightness)
Think of your muscles like rubber bands. Warm rubber stretches easily. Cold rubber becomes stiff and easier to snap.
That’s why many people feel:
- Morning stiffness
- Sharp twinges with sudden movements
- Increased risk of strains during winter workouts
When tissues lose flexibility, they pull on joints, increasing joint discomfort too.
2. Barometric (Atmospheric) Pressure Drops
Many people with arthritis swear they “feel the weather” in their bones.
They’re not wrong.
When barometric pressure drops before cold or rainy weather, pressure on joints slightly decreases. Swollen or inflamed joint tissues then expand, increasing pressure on surrounding nerves.
Result?
- More joint pain
- Increased swelling
- Heaviness or stiffness sensation
This is especially noticeable in:
- Osteoarthritis
- Rheumatoid arthritis
- Old fractures
- Post-surgery joints
3. Reduced Blood Circulation
Cold makes blood vessels constrict (narrow) to preserve warmth for vital organs.
Great for survival. Not so great for muscles and joints.
Reduced circulation leads to:
- Less oxygen to tissues
- Slower healing
- Increased stiffness
- Higher sense of pain
People with diabetes, hypertension, or vascular problems may feel this even more intensely.
4. Less Sunlight = Less Vitamin D
Vitamin D plays a key role in:
- Bone health
- Muscle strength
- Immune function
- Pain regulation
With less sunlight exposure in winter:
- Vitamin D levels fall
- Bones may ache more
- Muscles fatigue sooner
- Inflammation can increase
Low vitamin D is strongly associated with widespread pain, especially in the back and large joints.
5. Winter Means We Move Less
Cold weather often changes lifestyle habits.
We tend to:
- Stay indoors more
- Walk less
- Skip workouts
- Spend longer hours on screens
- Sit in poor postures
When we move less:
- Muscles weaken
- Joints stiffen
- Weight increases
- Pain sensitivity rises
In short: immobility feeds pain.
6. Mood, Stress, and Sleep Changes
Winter can affect mood and sleep because of shorter daylight hours and less outdoor time.
Poor sleep increases pain sensitivity. Low mood increases inflammation and tension.
Together, they amplify pain perception.
Pain science clearly shows:
The brain interprets pain based on signals from the body AND emotional context.
So winter can heighten both.
Who Suffers the Most in Winter?
Certain conditions flare up significantly in cold weather:
- Osteoarthritis
- Rheumatoid arthritis
- Fibromyalgia
- Low back pain
- Neck and shoulder pain
- Sciatica
- Post-fracture stiffness
- Sports injuries
- Tendinitis
- Frozen shoulder
- Plantar fasciitis
Even people without previous injuries may experience winter-related aches due to stiffness and poor movement.
How Physiotherapy Helps Winter Pain
Physiotherapy doesn’t just treat pain, it improves the way the body moves, heals, and adapts.
Let’s look at how :-
1. Restoring Mobility and Joint Lubrication
Movement is the best natural lubricant for joints.
Physiotherapists use targeted mobility techniques to:
- Improve joint glide
- Reduce stiffness
- Increase synovial fluid production
- Restore natural range of motion
Hands-on therapies may include:
- Joint mobilization
- Soft tissue release
- Stretching techniques
- Muscle energy techniques
When joints glide better, pain reduces naturally.
2. Improving Muscle Strength and Stability
Weak muscles make joints carry more load.
Winter weakens muscles faster because of inactivity, especially:
- Quadriceps
- Hip stabilizers
- Back extensors
- Core
- Rotator cuff muscles
Physiotherapy designs strengthening programs to:
- Support painful joints
- Reduce strain on ligaments
- Prevent re-injury
- Improve posture
- Enhance daily function
Stronger muscles = less winter pain.
3. Heat Therapy and Local Modalities
Physiotherapists may safely apply treatments like:
- Moist heat packs
- Ultrasound therapy
- Accelerated Healing Therapy
Heat increases circulation, relaxes tight muscles, and reduces stiffness, particularly effective before exercises.
4. Correcting Posture and Movement Patterns
Many winter aches come from:
- Slouching on couches
- Working on laptops in bed
- Sitting long hours
- Hunching shoulders against cold
Physiotherapists assess:
- Spine alignment
- Movement efficiency
- Muscle imbalances
- Workplace ergonomics
Then teach corrective strategies and exercises so movement becomes pain-free again.
5. Injury Prevention Education
Winter increases injury risk, especially when people jump into exercise without warming up.
A physiotherapist guides you on:
- Safe warm-ups
- Layering for temperature regulation
- Gradual exercise progression
- Proper footwear
- Avoiding slips and falls
Good education is as important as treatment.
Simple Daily Tips to Reduce Winter Pain
These practical strategies can make winter much more comfortable.
Warm Up Before Moving
Before morning activity:
- Gentle walking inside the house
- Slow stretching
- Warm shower
Warm tissues move better
Stay Consistently Active
Low-impact exercises are ideal:
- Brisk walking
- Stationary cycling
- Swimming in heated pools
- Yoga
- Pilates
- Physiotherapy-guided exercises
Little movement, repeated daily, is better than occasional intense workouts.
Dress Smart
Wear layers, especially around:
- Knees
- Lower back
- Neck
- Hands
Warm tissues equal less stiffness.
Support Vitamin D and Diet
(Always check with your doctor first.)
- Spend a few minutes in sunlight
- Include eggs, dairy, fortified cereals, mushrooms, fish
- Discuss supplements if recommended
Hydration matters too, dehydration worsens cramps and fatigue.
Improve Sleep and Stress Management
- Keep sleep routine consistent
- Avoid screens before bed
- Try breathing exercises or meditation
- Stay socially connected
A calmer nervous system perceives less pain.
When Should You See a Physiotherapist?
Seek professional assessment if you experience:
- Persistent or increasing pain
- Swelling or redness in joints
- Repeated stiffness preventing daily activities
- Pain after injury or fall
- Numbness or radiating pain
- Difficulty walking, lifting, or bending
Early physiotherapy prevents chronic pain patterns and long-term disability.
Why Choose Physiotherapy Support With a Patient-Focused Approach?
Pain is never “just physical.”
Each person has unique needs, goals, body structures, and healing capacity.
A physiotherapist doesn’t simply treat one painful spot, they study:
- Lifestyle
- Daily movement habits
- Work demands
- Past injuries
- Strength and flexibility patterns
- Posture
- Stress levels
This holistic approach empowers long-term recovery.
At DMPhysios, care focuses on understanding your body thoroughly, not just your symptoms. Individualized rehabilitation plans ensure better outcomes and confidence in movement.
Winter may increase discomfort, but with the right guidance, winter does not have to control your life.
Final Thoughts: You Don’t Have to “Just Tolerate” Winter Pain
Body pain worsening during winter is common, but it is not something you must simply endure.
Understanding why it happens gives you power.
And physiotherapy gives you tools to:
- stay mobile
- stay independent
- reduce pain
- prevent injuries
- improve quality of life
A structured rehabilitation plan, tailored exercises, lifestyle guidance, and scientific treatment methods can make winter significantly easier.
If winter pain has been stopping you from enjoying daily life, professional assessment can help you move safely and confidently again.
The team at DMPhysios works closely with patients to identify the real cause of pain, design corrective therapy, and support long-term joint health. Whether it’s arthritis, back pain, neck tightness, sports injuries, or unexplained stiffness, expert physiotherapy guidance can make a remarkable difference.
Stay warm.
Keep moving.
And remember, pain is not simply your fate in winter. With the right approach, you can stay active, strong, and comfortable all year round.