Overview
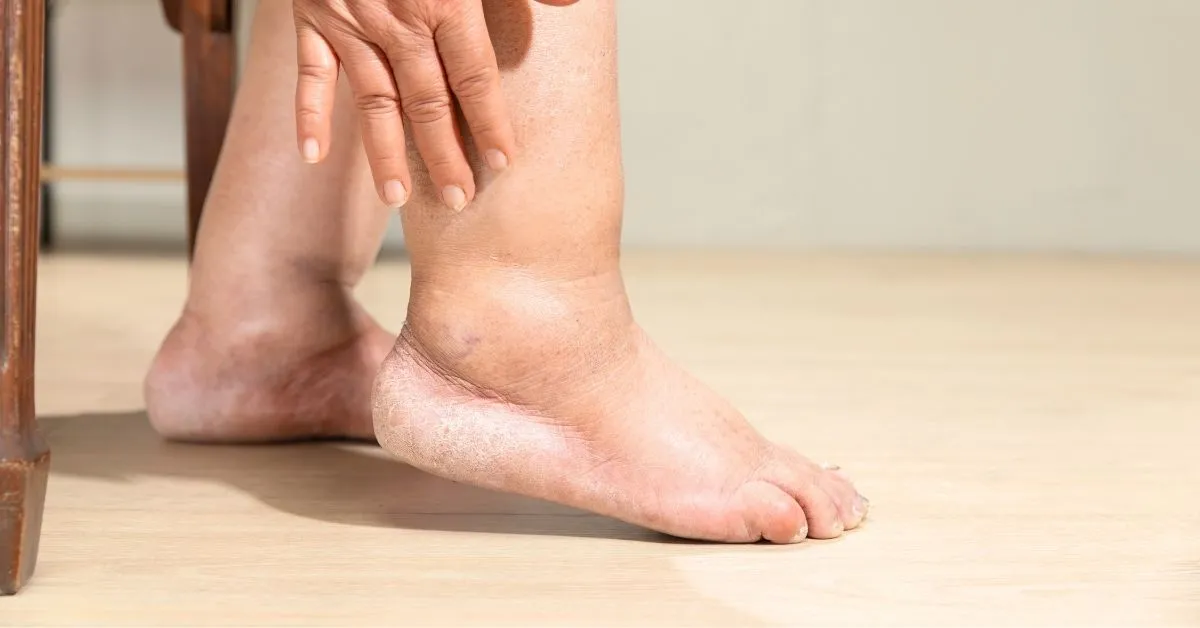
Lymphedema is a long-term (chronic) health condition in which there is an abnormal buildup of lymphatic fluid in the soft tissues of the body, leading to visible swelling—most often affecting the arms or legs, but it can also occur in the face, chest, or other regions. The lymphatic system, made up of vessels, nodes, and specialized organs, plays a vital role in maintaining fluid balance, transporting immune cells, and removing waste products from tissues.
When this intricate drainage network becomes damaged, obstructed, or fails to function effectively, lymph fluid cannot circulate and drain as it should. This results in a gradual accumulation that causes swelling, skin thickening, discomfort, and, in some cases, significant mobility limitations.
The severity of lymphedema can vary widely—from mild, barely noticeable puffiness to severe, disabling swelling that interferes with daily activities. If left untreated, it may lead to complications such as recurrent infections, reduced flexibility, and permanent changes in skin texture (fibrosis).
At DMPhysios, a trusted clinic in Noida specializing in spine and sports conditions with a strong focus on patient-centered rehabilitation, we recognize that lymphedema affects far more than just the body. Beyond the physical swelling, it can impact a person’s self-confidence, emotional well-being, and overall lifestyle.
That’s why our approach goes beyond symptom control—we aim to provide comprehensive care, including accurate diagnosis, timely intervention, and tailored physiotherapy programs. By combining advanced therapeutic techniques with patient education and emotional support, we help individuals manage lymphedema effectively and regain a better quality of life.
Symptoms
The symptoms of lymphedema can develop gradually and may worsen over time if not addressed. Common signs and symptoms include:
- Persistent swelling in one or more parts of the body (commonly arms, legs, or face)
- A sensation of weight or constriction in the affected limb
- Reduced flexibility or range of motion
- Skin changes such as thickening, hardening, or fibrosis
- Recurring skin infections (cellulitis)
- Discomfort, aching, or pain in the swollen area
- Swelling that worsens during the day and improves overnight in early stages
Recognizing the early symptoms of lymphedema is crucial for starting treatment before complications arise.
Types of Lymphedema
Lymphedema is broadly classified into two main categories:
1. Primary Lymphedema
- Resulting from inherited or congenital defects in the lymphatic system.
- May develop at birth (congenital lymphedema), during puberty (lymphedema praecox), or later in life (lymphedema tarda).
- Often results from underdeveloped or absent lymphatic vessels.
2. Secondary Lymphedema
- The more common form, caused by damage to or obstruction of previously normal lymphatic vessels.
- It can be triggered by factors such as surgery (particularly lymph node removal during cancer treatment), radiation therapy, injury, infection, or long-term venous insufficiency.
- It can also develop as a result of parasitic infections such as filariasis in certain parts of the world.
Causes
Lymphedema occurs when the lymphatic system is unable to drain lymph fluid effectively. Common causes include:
- Cancer treatment: Procedures like lymph node removal or radiation therapy may harm the lymphatic vessels.
- Infections: Bacterial infections or parasitic infections like filariasis can cause inflammation and blockage.
- Surgery or injury: Damage to the lymphatic vessels can disrupt normal fluid drainage.
- Venous diseases: Chronic venous insufficiency increases lymphatic load.
- Congenital defects: Developmental abnormalities in lymph vessels.
- Obesity: Excess body weight can put strain on lymphatic function.
Risk Factors
While lymphedema can develop in anyone, certain factors increase the likelihood:
- History of cancer surgery or radiation, especially breast, pelvic, or prostate cancers
- Recurrent skin infections
- Chronic venous disorders
- Family history of primary lymphedema
- Severe obesity
- Advanced age
- Lack of physical activity
Patients undergoing cancer treatment should be particularly vigilant about lymphedema prevention.
Treatment
Although lymphedema is generally a chronic condition, it can be effectively managed with the right approach. The goals of treatment include:
- Reducing swelling
- Preventing complications like infections or fibrosis
- Improving mobility and function
- Enhancing overall quality of life
Treatment may involve:
- Manual Lymphatic Drainage (MLD) – A gentle, targeted massage technique designed to stimulate lymphatic circulation.
- Compression therapy – Use of bandages or compression garments to prevent fluid buildup.
- Exercise therapy – Specific, gentle exercises to stimulate lymph movement.
- Skin care – Maintaining skin hygiene to prevent infections.
- Pneumatic compression devices – Mechanical pumps that aid lymph drainage.
Physiotherapy Treatment
At DMPhysios in Noida, our physiotherapy team adopts a patient-centered rehabilitation approach tailored to each individual’s needs. Physiotherapy plays a central role in the Complete Decongestive Therapy (CDT) approach, which is considered the gold standard in lymphedema management.
1. Initial Assessment
Our expert physiotherapists conduct a thorough evaluation to assess the stage and severity of lymphedema, identify contributing factors, and set personalized treatment goals.
2. Manual Lymphatic Drainage (MLD)
- A gentle, hands-on technique that stimulates the lymphatic system.
- Performed in a specific sequence to encourage fluid movement toward functional lymph nodes.
- Helps reduce swelling, discomfort, and skin tension.
3. Compression Therapy
- We prescribe and fit medical-grade compression garments or multilayer bandaging systems.
- Compression prevents fluid reaccumulation after drainage.
- Bandaging techniques are adjusted depending on whether the patient is in the intensive or maintenance phase of treatment.
4. Therapeutic Exercises
- Low-intensity, rhythmic exercises are designed to enhance lymphatic circulation.
- Common activities include ankle pumps, gentle shoulder movements, deep breathing exercises, and resistance training with light weights.
- Exercises are performed while wearing compression garments for maximum benefit.
5. Skin and Nail Care
- Education on keeping skin clean, moisturized, and infection-free.
- Prevention of cuts, insect bites, or burns on the affected limb.
6. Kinesio Taping
- Special elastic tape is applied to lift the skin microscopically, improving lymph flow.
- Particularly useful for difficult-to-bandage areas.
7. Patient Education
- At DMPhysios, we believe empowering patients with knowledge is key.
- We teach self-massage techniques, correct garment usage, and safe exercise routines to maintain results at home.
8. Advanced Rehabilitation Support
- For athletes and active individuals, our sports rehabilitation team ensures lymphedema management is integrated with strength training and performance recovery.
Prevention
While not all cases can be prevented, especially primary lymphedema, risk can be minimized by:
- Avoiding injury or infection in at-risk limbs
- Maintaining a healthy weight and active lifestyle
- Performing gentle range-of-motion exercises after surgery
- Wearing compression garments during activities that strain the limb
- Avoiding extreme temperatures (hot tubs, saunas)
- Seeking early treatment at the first sign of swelling
Patients who have undergone cancer surgery should have a personalized prevention plan, which DMPhysios offers as part of post-surgical rehabilitation.
Conclusion
Lymphedema can be a life-long condition, but with the right care, its effects can be minimized, allowing patients to lead active, healthy lives. Early diagnosis, proper treatment, and consistent physiotherapy can make a remarkable difference in outcomes. At DMPhysios, a leading clinic in Noida for spine and sports conditions with patient-centered rehabilitation, we are committed to helping individuals manage lymphedema through evidence-based therapy, education, and personalized care.If you or someone you know is experiencing swelling, heaviness, or other signs of lymphedema, don’t wait for the condition to progress. Reach out to DMPhysios today and take the first step toward effective, long-term management. Begin your path toward healing and a better quality of life today.