Overview
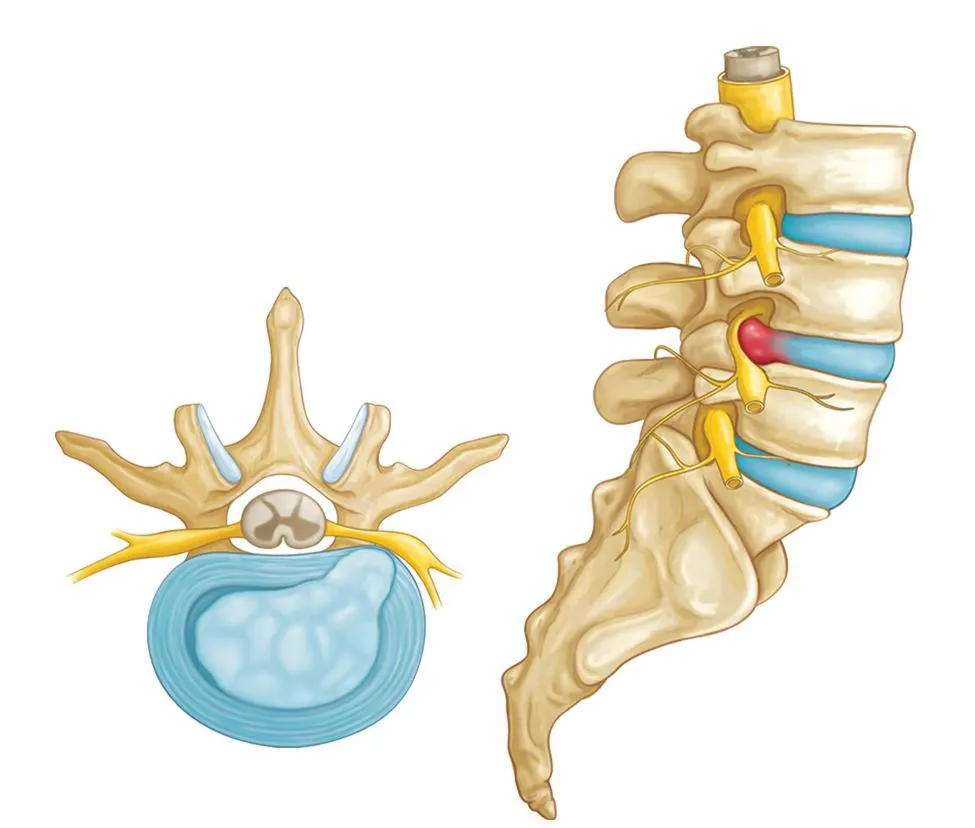
A prolapsed intervertebral disc (PIVD), commonly known as a slipped or herniated disc, is one of the most prevalent causes of back and neck pain worldwide. It occurs when the soft, gel-like inner core of an intervertebral disc (nucleus pulposus) protrudes through the tough outer layer (annulus fibrosus). This protrusion may impinge on nearby nerves or the spinal cord, resulting in pain, numbness, weakness, or altered reflexes.
At DMPhysios, a leading clinic located in Noida specializing in spine and sports conditions with patient-centered rehabilitation, we frequently see patients presenting with symptoms of prolapsed intervertebral disc. Our evidence-based approach focuses not only on relieving pain but also on restoring function and preventing recurrence.
The intervertebral discs act as shock absorbers between the vertebrae in the spine. Any disruption of their integrity, such as in a prolapsed intervertebral disc, can significantly affect spinal stability, mobility, and nerve health. Understanding this condition, its causes, and the available treatments is crucial for recovery and prevention.
Symptoms
The symptoms of a prolapsed intervertebral disc vary depending on the location and severity of the prolapse. Common signs include:
- Localized back or neck pain: Persistent pain at the affected spinal level, often aggravated by movement or prolonged posture.
- Radiating pain: Sciatica (pain radiating down the leg) is a hallmark of lumbar prolapsed intervertebral disc, while cervical prolapse may cause pain radiating into the arm.
- Numbness and tingling: Paresthesia in the extremities corresponding to the compressed nerve root.
- Weakness in muscles: Difficulty lifting the foot (foot drop), gripping objects, or maintaining posture.
- Altered reflexes: Decreased knee or ankle jerk in lumbar cases; diminished biceps or triceps reflexes in cervical cases.
- Bladder or bowel disturbances: Rare but serious, requiring immediate medical attention (possible cauda equina syndrome).
At DMPhysios, each patient with a prolapsed intervertebral disc undergoes a thorough clinical examination to identify the exact nerve involvement and severity of symptoms. This helps us design a precise rehabilitation plan.
Types of Prolapsed Intervertebral Disc
Although the term prolapsed intervertebral disc is often used as a blanket description, the actual presentation can differ significantly from patient to patient. Understanding these variations is important because the type and stage of disc prolapse directly influence symptoms, prognosis, and the choice of treatment. At DMPhysios, a leading clinic in Noida for spine and sports conditions, we emphasize identifying the exact nature of the disc pathology before designing a rehabilitation program.
Stages of Disc Prolapse
- Disc Protrusion (Bulge)
In this early stage, the inner gel-like material of the disc (nucleus pulposus) begins to push outward, causing the outer layer (annulus fibrosus) to stretch but not tear. The disc remains structurally intact, and symptoms may be mild or intermittent, often presenting as localized back or neck discomfort. Early intervention at this stage can often prevent progression. - Disc Extrusion
Here, the nucleus pulposus pushes through a tear in the annulus fibrosus but remains attached to the main disc body. Because the disc material has breached its outer wall, nerve compression is more likely, and symptoms such as radiating pain, numbness, or weakness become more prominent. This stage is typically more painful and may limit normal activity if left unaddressed. - Disc Sequestration (Free Fragment)
In this advanced stage, a portion of the nucleus pulposus breaks free and becomes a separate fragment within the spinal canal. This “loose” disc material can cause severe nerve irritation or inflammation, often resulting in significant neurological symptoms. Prompt evaluation is crucial at this point to determine whether conservative or surgical management is appropriate. - Contained vs. Uncontained Herniation
A contained herniation means the disc’s outer covering is still intact even though it bulges outward, whereas an uncontained herniation means the inner material has escaped through a rupture. This distinction matters because uncontained herniations tend to produce more intense symptoms and may respond differently to specific treatments.
Location-Based Variations
The region of the spine where the prolapsed intervertebral disc occurs also influences how it presents:
- Cervical Prolapsed Intervertebral Disc – Located in the neck, this form typically produces neck pain radiating into the shoulders, arms, or hands, sometimes with tingling or weakness.
- Thoracic Prolapsed Intervertebral Disc – Rare compared to other levels; it can cause pain around the rib cage or altered trunk sensation and may mimic other conditions.
- Lumbar Prolapsed Intervertebral Disc – The most common site, often presenting with low back pain, sciatica, or difficulty standing and walking due to leg symptoms.
Because each variation of a prolapsed intervertebral disc behaves differently, identifying the exact type and stage is a cornerstone of effective management. DMPhysios employs thorough clinical assessment, neurological testing to accurately diagnose the condition. This detailed evaluation allows the team to tailor treatment plans, whether conservative physiotherapy or referral for medical interventions, ensuring that every patient receives the most appropriate care for their unique presentation.
Causes
A prolapsed intervertebral disc develops due to weakening or damage of the disc structure. Common causes include:
- Age-related degeneration: Natural wear and tear causes discs to lose hydration and elasticity.
- Repetitive strain: Heavy lifting, bending, twisting, or high-impact sports can stress the spine.
- Poor posture: Slouching or prolonged sitting places increased load on lumbar discs.
- Trauma: Sudden injury, falls, or accidents.
- Genetic predisposition: Family history of disc problems.
- Smoking: Reduces disc nutrition, accelerating degeneration.
- Sedentary lifestyle: Weak core muscles fail to support the spine effectively.
At DMPhysios, we emphasize patient education to address these root causes. By correcting movement patterns and ergonomics, we help prevent recurrence of prolapsed intervertebral disc.
Risk Factors
Certain factors make individuals more susceptible to developing a prolapsed intervertebral disc:
- Age between 30–50 years – peak incidence of disc herniation.
- Occupation requiring heavy lifting or prolonged sitting.
- Obesity – increases spinal load.
- Weak core and back muscles.
- High-impact sports like weightlifting, wrestling, or gymnastics.
Recognizing these risk factors allows the team at DMPhysios to create proactive rehabilitation programs tailored to each patient’s lifestyle.
Treatment
Treatment of prolapsed intervertebral disc ranges from conservative management to surgical intervention, depending on the severity and persistence of symptoms.
Conservative (Non-surgical) Management
- Rest and activity modification: Avoid activities that worsen pain but maintain gentle movement.
- Medications: NSAIDs, analgesics, or muscle relaxants as prescribed by physicians.
- Heat or cold therapy: Reduces inflammation and muscle spasm.
- Epidural steroid injections: In selected cases for reducing nerve root inflammation.
Surgical Options
Surgery is considered when conservative measures fail after several weeks or in the presence of severe neurological deficits. Common procedures include:
- Microdiscectomy: Removal of the prolapsed portion of the disc.
- Laminectomy: Relieving pressure on nerves by removing part of the vertebral bone.
- Disc replacement: In selected cases, replacing the damaged disc with an artificial implant.
However, most cases of prolapsed intervertebral disc improve with non-surgical management, especially when combined with structured physiotherapy.
Physiotherapy Treatment
At DMPhysios, physiotherapy for prolapsed intervertebral discs is the cornerstone of recovery. Our Noida-based clinic specializes in spine and sports conditions and provides patient-centered rehabilitation tailored to individual needs.
A typical physiotherapy program for prolapsed intervertebral disc at DMPhysios includes:
1. Pain Relief and Inflammation Reduction
- Modalities: Accelerated Healing Therapy to reduce pain and muscle spasm.
- Positioning and posture training: Teaching optimal positions that relieve nerve compression.
2. Core Stabilization and Strengthening
- McKenzie exercises (Extension-based movements): Especially beneficial for lumbar disc prolapse to centralize pain.
- Transverse abdominis activation: Strengthens deep abdominal muscles to support the spine.
- Multifidus strengthening: Improves segmental spinal stability.
3. Flexibility and Mobility Training
- Hamstring and hip flexor stretches: Reduce tension on the lumbar spine.
- Thoracic mobility drills: Improve overall spinal biomechanics.
4. Neural Mobilization
- Gentle nerve gliding techniques to reduce nerve root irritation and restore normal neural mobility.
5. Posture Correction and Ergonomics
- Workstation setup: Educating patients on correct chair height, lumbar support, and monitor level.
- Lifting techniques: Teaching safe ways to lift and carry loads.
6. Gradual Return to Activity
- Tailored functional exercises and sport-specific rehabilitation for athletes.
- Graded exposure to movement to reduce fear-avoidance behavior.
7. Education and Self-Management
- Teaching patients about the nature of prolapsed intervertebral disc, warning signs, and relapse prevention strategies.
- Developing home exercise programs to maintain progress between clinic visits.
At DMPhysios, the physiotherapy team continually reassesses progress and modifies the program, ensuring the patient regains not only pain-free movement but also confidence in their spine’s resilience.
Prevention
Preventing a prolapsed intervertebral disc involves maintaining a healthy spine through lifestyle and movement habits:
- Strengthen the core and back muscles with regular exercises.
- Maintain good posture while sitting, standing, and lifting.
- Use ergonomic furniture for work and study.
- Avoid smoking to preserve disc health.
- Maintain healthy body weight to reduce spinal load.
- Regular physical activity such as walking, swimming, or yoga.
- Take breaks from prolonged sitting to stretch and move.
At DMPhysios, we incorporate preventive education into every rehabilitation program, empowering patients to take charge of their spinal health and minimize the risk of future episodes.
Conclusion
A prolapsed intervertebral disc can be debilitating, but with timely diagnosis, effective treatment, and guided rehabilitation, most individuals achieve full recovery. Understanding its symptoms, causes, and risk factors helps in seeking care promptly.
DMPhysios, a renowned clinic in Noida specializing in spine and sports conditions, offers evidence-based, patient-centered rehabilitation for individuals suffering from prolapsed intervertebral disc. With expert physiotherapists, personalized exercise plans, and comprehensive education, DMPhysios not only helps you recover but also equips you to prevent recurrences.If you or someone you know is experiencing back or neck pain suggestive of a prolapsed intervertebral disc, don’t wait for the symptoms to worsen. Contact DMPhysios today to book an assessment and begin your journey toward a healthier, pain-free spine.