Overview
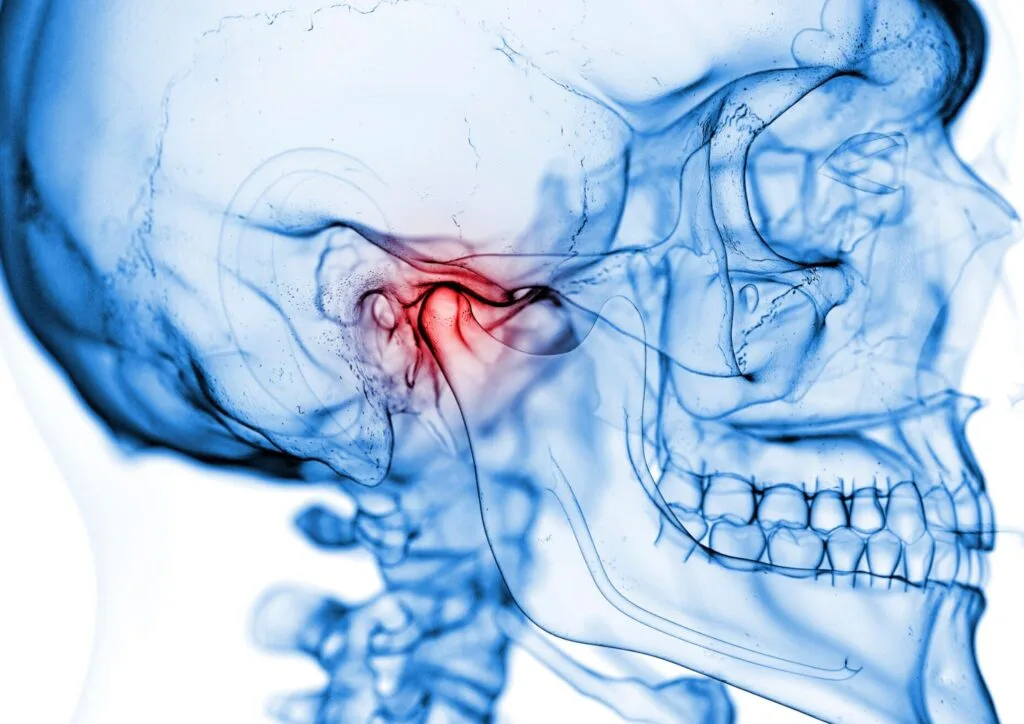
Temporomandibular joint dysfunction, often abbreviated as TMD, refers to a group of conditions that impair the normal functioning of the temporomandibular joints (TMJ)—the hinge-like joints that connect the lower jawbone (mandible) to the temporal bones of the skull, situated just in front of each ear. These joints are essential for performing everyday activities such as chewing, speaking, yawning, and swallowing, as they allow smooth and coordinated movement of the jaw.
Temporomandibular joint dysfunction arises when there is an abnormality, inflammation, or irritation in the joint itself, the surrounding muscles, or related connective tissues. This may present as pain in the jaw or face, difficulty or restriction in opening or closing the mouth, and audible sounds such as clicking, popping, or grinding during jaw movement. The condition can affect one or both sides of the face and may fluctuate in intensity over time.
Although temporomandibular joint dysfunction can occur at any age, it is most commonly seen in adults between the ages of 20 and 40. It is also observed more frequently in women, possibly due to hormonal influences or differences in muscle function and joint mechanics.
At DMPhysios, a trusted physiotherapy clinic located in Noida, we specialize in the management of spine and sports-related conditions, including complex joint dysfunctions such as TMD. Our approach is rooted in patient-centered rehabilitation, combining advanced physiotherapy techniques with personalized care to help individuals regain jaw function, reduce pain, and improve their overall quality of life.
Symptoms of Temporomandibular Joint Dysfunction
The symptoms of temporomandibular joint dysfunction can vary widely depending on the severity and underlying cause. Common signs include:
- Jaw discomfort or tenderness, particularly noticeable during activities like chewing or speaking
- Clicking, popping, or grating sounds during jaw movement
- Jaw locking, where the mouth becomes stuck in either an open or closed position
- Difficulty opening the mouth wide
- Headaches and earaches, often mistaken for migraines or inner ear issues
- Pain around the ears, temples, or face
- Neck and shoulder pain, particularly if muscular tension is involved
- Tinnitus (ringing in the ears)
- Dizziness or a sense of imbalance
Symptoms may be intermittent or persistent and can significantly interfere with daily activities like eating, speaking, or sleeping.
Types of Temporomandibular Joint Dysfunction
Temporomandibular joint dysfunction is not a single, uniform condition but rather a broad spectrum of disorders that can impact the jaw joint and its associated structures in different ways. Based on clinical presentation and underlying pathology, TMD can be classified into the following three major types:
1. Myofascial Pain Dysfunction (MPD)
This is the most prevalent form of temporomandibular joint dysfunction. It primarily affects the muscles of mastication—the group of muscles responsible for jaw movement. Patients with MPD often report deep, aching pain in the jaw, face, neck, or shoulders, along with muscle tightness or spasms. Discomfort may intensify with jaw movements like talking, chewing, or yawning. Unlike joint-based TMD, this type is muscular in origin and is often linked to stress, bruxism (teeth grinding), or poor posture. In many cases, referred pain may even mimic headaches or earaches, making diagnosis more challenging.
2. Internal Derangement of the Temporomandibular Joint
This type involves a mechanical or structural disruption within the joint itself. The most common cause is a displacement of the articular disc, which serves as a cushion between the jawbone and the skull. When this disc moves out of its normal position, it can lead to clicking, popping, or grinding sounds during jaw movement, as well as episodes of jaw locking, where the mouth becomes temporarily stuck in an open or closed position. Internal derangement may result from direct trauma, repetitive strain, or congenital abnormalities, and often leads to restricted movement and joint discomfort.
3. Degenerative Joint Disease (DJD)
This category encompasses joint-related conditions like osteoarthritis and rheumatoid arthritis, where the structural integrity of the temporomandibular joint is compromised. Over time, the cartilage lining the joint surfaces wears down, leading to inflammation, stiffness, and chronic pain. In rheumatoid arthritis, the autoimmune destruction of joint tissues can further accelerate degeneration. Patients may experience crepitus (a grating sensation), limited jaw mobility, and progressive joint deformity. DJD often requires a multidisciplinary approach for long-term management, including physiotherapy, medication, and in some cases, surgical consultation.
At DMPhysios, we tailor treatment strategies depending on the specific type and severity of temporomandibular joint dysfunction, ensuring optimal outcomes for each patient.
Causes
Identifying the underlying cause of temporomandibular joint dysfunction is crucial for implementing effective treatment strategies. Common contributing factors include:
- Bruxism (teeth grinding or clenching)
- Jaw trauma or injury, such as fractures or whiplash
- Arthritis, including osteoarthritis or rheumatoid arthritis
- Poor posture, especially forward head posture
- Stress, which may lead to unconscious jaw clenching
- Malocclusion (improper bite)
- Overuse of jaw muscles, such as excessive gum chewing
- Dental work, particularly if it alters jaw alignment
DMPhysios focuses on identifying and addressing these underlying factors through thorough evaluation and individualized rehabilitation.
Risk Factors
Several risk factors increase the likelihood of developing temporomandibular joint dysfunction:
- Gender: Women are more prone to TMD, possibly due to hormonal influences on joint tissues
- Age: Most frequently occurs in individuals between the ages of 20 and 40
- Stress and anxiety: Increase muscle tension and bruxism
- Postural abnormalities, such as tech neck
- Previous injuries: Especially those involving the jaw or cervical spine
- Autoimmune diseases, like lupus or rheumatoid arthritis
Understanding these risks can help with early intervention and prevention strategies, especially under the guidance of a specialized center like DMPhysios in Noida.
Treatment
Treatment of temporomandibular joint dysfunction usually begins with conservative, non-invasive methods before progressing to more aggressive interventions. Common options include:
1. Medications
- Analgesics and anti-inflammatories: To manage pain and inflammation
- Muscle relaxants: Especially helpful for bruxism-related TMD
- Tricyclic antidepressants: Sometimes used for chronic pain management
2. Dental Interventions
- Occlusal splints or night guards: Custom-made devices to prevent teeth grinding
- Corrective dental procedures: In cases of malocclusion or missing teeth
3. Invasive Procedures (if conservative treatment fails)
- Intra-articular injections (e.g., corticosteroids)
- Arthrocentesis or arthroscopy: Minimally invasive surgical procedures
- Open joint surgery: Rare and reserved for severe, unresponsive cases
However, for most patients, physiotherapy is the cornerstone of long-term recovery and symptom management.
Physiotherapy Treatment
At DMPhysios, a trusted name in Noida for spine and sports conditions, physiotherapy is the cornerstone of our patient-centered care for temporomandibular joint dysfunction. Our approach is evidence-based and highly individualized.
Comprehensive Physiotherapy Assessment
We begin with a detailed evaluation that includes:
- Jaw range of motion
- Muscle tenderness and spasm assessment
- Postural evaluation, especially head and cervical spine alignment
- Functional analysis of jaw movements
Manual Therapy Techniques
- Soft tissue release: Targeting tight masticatory muscles such as masseter and temporalis
- Trigger point therapy: To relieve referred pain from hyperirritable muscle spots
- Joint mobilizations: Gentle mobilization of the TMJ to restore joint play
Electrotherapy
- Accelerated Healing Therapy: To promote tissue healing and reduce inflammation
Therapeutic Exercises
- Controlled mouth opening/closing with tongue posture control
- Isometric exercises: To improve jaw stability
- Cervical spine mobility and strengthening
- Postural correction exercises, including chin tucks and scapular retraction
Posture and Ergonomics Training
- Addressing head-forward posture common with prolonged device use
- Ergonomic advice for workstations
Home Care Protocol
- Education on soft food diets
- Jaw relaxation techniques
- Ice/heat therapy guidance
- Avoidance of habits like gum chewing or jaw resting on hands
The DMPhysios team ensures every treatment plan is adapted as per patient progress, empowering recovery and minimizing recurrence.
Prevention
Preventing temporomandibular joint dysfunction involves a mix of awareness, behavior modification, and lifestyle adjustments:
- Avoid jaw overuse: Limit gum chewing and avoid hard foods
- Practice stress management: Yoga, meditation, or counseling can help reduce bruxism
- Maintain good posture: Especially during prolonged sitting or screen time
- Jaw rest: Keep lips together and teeth apart when not eating or speaking
- Regular stretching: Gentle jaw and neck stretches to maintain mobility
- Dental hygiene and alignment checks: Timely correction of bite issues
DMPhysios promotes proactive measures through patient education sessions and ergonomic workshops in Noida to help reduce the incidence of TMD.
Conclusion
Temporomandibular joint dysfunction is a multifactorial condition that can disrupt essential daily functions like eating, speaking, and sleeping. However, with accurate diagnosis and comprehensive treatment—especially physiotherapy—most patients can achieve significant relief and restored function.
At DMPhysios, a premier clinic in Noida for spine and sports conditions, we pride ourselves on delivering patient-centered rehabilitation tailored to individual needs. Our expert team of physiotherapists utilizes advanced techniques and personalized strategies to address every aspect of temporomandibular joint dysfunction, from pain relief to long-term functional recovery.
If you or someone you know is experiencing jaw discomfort, clicking, or facial pain, don’t wait. Early intervention is the key to preventing chronic complications.Book your consultation with DMPhysios today and take the first step toward a pain-free, confident life. Let us help you move, eat, and speak without limits—because your jaw health matters.