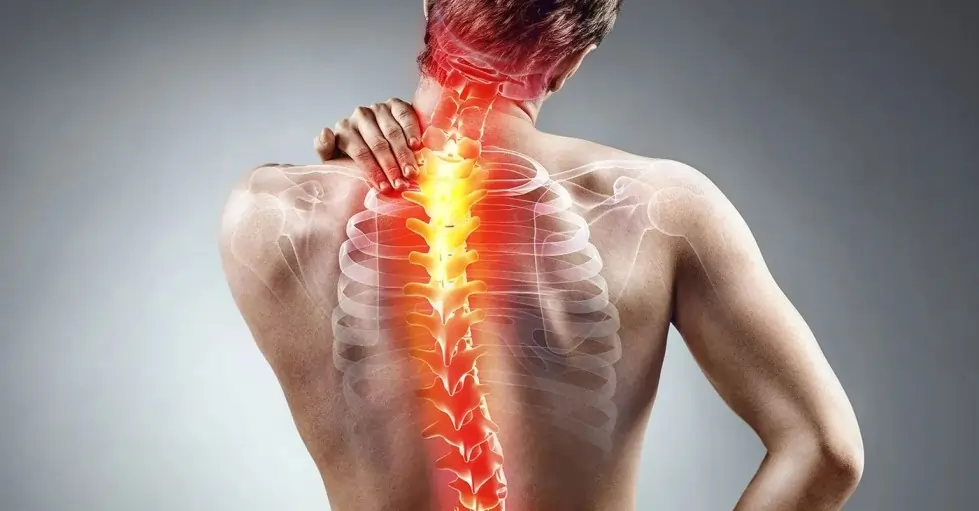
Referred Pain: When the Pain Location Lies to You
I
Have you ever felt pain in one part of your body, but later discovered the real problem was somewhere completely different? A hurting shoulder that turns out to be a gallbladder issue. Jaw pain that has nothing to do with teeth. Back pain that actually starts from the hip. These confusing experiences are not rare. They are examples of something called referred pain
Referred pain is one of the most misunderstood concepts in health and medicine. It can delay diagnosis, cause unnecessary treatments, and create anxiety for people who cannot understand why tests on the painful area keep coming back normal. Yet, once understood, referred pain makes perfect sense.
This article explains referred pain in simple language. You will learn what it is, why it happens, common examples, when it can be serious, and how it is assessed and treated using evidence based approaches.
What is referred pain?
Referred pain means pain that is felt in one area of the body but originates from another area. The place where you feel pain is not the actual source of the problem.
For example, during a heart attack, pain is often felt in the left arm, shoulder, jaw, or neck, even though the heart is located in the chest. Similarly, problems in internal organs like the gallbladder or kidneys may cause pain in the shoulder or back rather than the abdomen.
This happens because the nervous system sometimes struggles to correctly identify where pain signals are coming from. The brain receives the message that something hurts, but it misinterprets the location.
It is important to understand that referred pain is real pain. It is not imagined, exaggerated, or psychological. The pain experience is genuine even if the source is hidden.
Why does referred pain happen?
To understand referred pain, it helps to understand how pain signals travel.
Pain signals move through nerves to the spinal cord and then to the brain. Different body parts can share the same nerve entry points into the spinal cord. When this happens, the brain may confuse the source of the pain.
Shared nerve pathways
Many internal organs and muscles send pain signals to the same spinal cord levels. Since the brain is more familiar with pain coming from skin and muscles than from organs, it often assumes the pain is coming from a more common location.
This is known as nerve convergence. It is the most widely accepted explanation for referred pain.
Central sensitization
When pain persists over time, the nervous system can become more sensitive. The spinal cord and brain amplify pain signals, and the area of pain can spread. This makes pain feel more widespread and harder to pinpoint.
Central sensitization explains why referred pain can sometimes feel intense or persistent even when tissue damage is minimal.
Muscle and joint involvement
Referred pain does not only come from organs. Deep muscles, joints, ligaments, and spinal structures can also produce pain felt in distant areas. Tight or overloaded muscles can refer pain to nearby or even far regions.
This is common in neck, shoulder, and lower back problems.
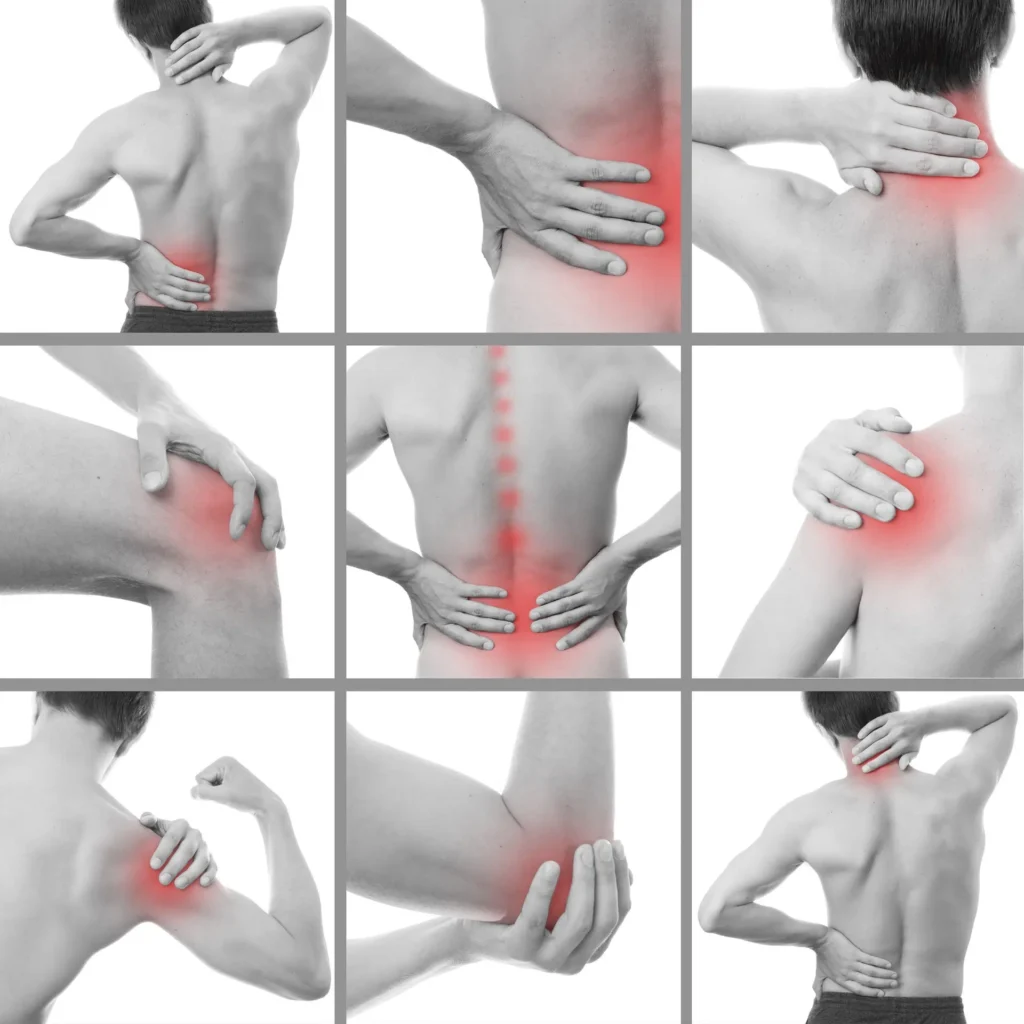
Common examples of referred pain
Understanding common patterns helps people recognize when pain might not be coming from where it is felt.
Heart related pain
Heart pain does not always feel like chest pain. It may appear as discomfort in the left arm, shoulder, neck, jaw, or upper back. This is why unexplained arm or jaw pain should never be ignored, especially if accompanied by breathlessness, sweating, or nausea.
Gallbladder pain
Gallbladder problems often cause pain in the right shoulder or between the shoulder blades. Many people assume this is a muscle strain, but the true source may be digestive.
Kehr’s sign
Pain in the left shoulder caused by irritation inside the abdomen, often from the spleen, is called Kehr’s sign. It is a classic example of referred pain and can be a medical emergency.
Neck related jaw or headache pain
Problems in the upper neck can refer pain to the head, face, or jaw. This is why some headaches and jaw pains persist even after dental or neurological tests are normal.
Muscle trigger points
Tight bands in muscles, commonly called trigger points, can send pain to other areas. For example, a trigger point in the upper back can cause headaches or shoulder pain.
Referred pain vs radiating pain
People often confuse referred pain with radiating pain, but they are different.
Radiating pain follows the path of a nerve. Sciatica is a good example, where pain travels down the leg along the sciatic nerve.
Referred pain does not follow a nerve path. It feels more vague, dull, or deep and does not cause tingling, numbness, or weakness.
This distinction is important because treatment approaches differ.
Why referred pain can be misleading
Referred pain can lead to incorrect assumptions and delayed treatment. People often focus on the painful area and ignore other signs. Imaging tests may appear normal because the real problem lies elsewhere.
For example, repeated shoulder scans may show no damage, while the actual issue lies in the neck, upper back, or internal organs.
This is why a thorough assessment that looks beyond the painful spot is essential.
At DMPhysios, assessments focus on identifying the true source of pain rather than only treating the area where pain is felt. This approach helps prevent repeated flare ups and incomplete recovery.
When referred pain can be serious
Some referred pain patterns require immediate medical attention.
Sudden jaw, arm, or shoulder pain with chest discomfort may indicate heart problems. Shoulder pain after trauma could signal internal bleeding. Back or flank pain with fever may suggest kidney infection.
If pain is severe, sudden, or associated with symptoms like breathlessness, dizziness, fever, or weakness, medical evaluation should not be delayed.
How referred pain is diagnosed
There is no single test for referred pain. Diagnosis relies on clinical reasoning and pattern recognition.
Detailed history
The healthcare provider asks about onset, timing, triggers, and associated symptoms. Pain linked to meals, stress, posture, or activity offers important clues.
Physical examination
Movement testing, muscle palpation, spinal assessment, and posture evaluation help identify musculoskeletal sources. Reproduction of the familiar pain during examination is a key sign.
Ruling out serious causes
If organ related pain is suspected, medical tests such as blood work, scans, or heart tests are used to rule out dangerous conditions.
Response to treatment
Sometimes the diagnosis becomes clear when treating the suspected source reduces the referred pain.
Physiotherapists play a major role in this process. At DMPhysios, a detailed assessment helps differentiate between local pain, referred pain, and nerve related pain, ensuring the right treatment strategy from the start.
How referred pain is treated
The most important rule is this: treat the source, not just the symptom.
Musculoskeletal referred pain
If pain originates from muscles, joints, or the spine, physiotherapy is often highly effective. Treatment may include:
- Therapeutic exercises
- Manual therapy
- Postural correction
- Movement retraining
- Education about pain mechanisms
This approach helps calm the nervous system and restore normal movement patterns.
DMPhysios uses evidence based physiotherapy techniques to address the underlying cause of referred pain rather than offering short term relief alone.
Visceral referred pain
If internal organs are involved, medical treatment is essential. Physiotherapy may support recovery but does not replace medical management.
Persistent or sensitized pain
When pain has been present for a long time, the nervous system may remain sensitive even after tissue healing. Education, graded activity, and confidence building play a crucial role in recovery.
What you can do as a patient
Do not assume pain is coming from where it hurts. Notice patterns related to food, posture, activity, or stress. Avoid self diagnosis based on internet searches alone.
Seek professional assessment if pain persists or keeps returning. Understanding pain reduces fear and improves recovery.
At DMPhysios, patients are guided through understanding their pain, rebuilding trust in movement, and achieving long term relief rather than temporary fixes.
Frequently Asked Questions
Conclusion
Pain location does not always reveal the true problem. Referred pain is common and real. It occurs because of shared nerve pathways and nervous system processing.
Correct diagnosis requires looking beyond the painful area. Treatment is most effective when the underlying source is addressed.
Clinics like DMPhysios focus on root cause assessment and individualized rehabilitation, helping patients recover with clarity and confidence.